Anemia and iron metabolism in COVID-19: a systematic review and meta-analysis
- PMID: 32816244
- PMCID: PMC7438401
- DOI: 10.1007/s10654-020-00678-5
Anemia and iron metabolism in COVID-19: a systematic review and meta-analysis
Abstract
Iron metabolism and anemia may play an important role in multiple organ dysfunction syndrome in Coronavirus disease 2019 (COVID-19). We conducted a systematic review and meta-analysis to evaluate biomarkers of anemia and iron metabolism (hemoglobin, ferritin, transferrin, soluble transferrin receptor, hepcidin, haptoglobin, unsaturated iron-binding capacity, erythropoietin, free erythrocyte protoporphyrine, and erythrocyte indices) in patients diagnosed with COVID-19, and explored their prognostic value. Six bibliographic databases were searched up to August 3rd 2020. We included 189 unique studies, with data from 57,563 COVID-19 patients. Pooled mean hemoglobin and ferritin levels in COVID-19 patients across all ages were 129.7 g/L (95% Confidence Interval (CI), 128.51; 130.88) and 777.33 ng/mL (95% CI, 701.33; 852.77), respectively. Hemoglobin levels were lower with older age, higher percentage of subjects with diabetes, hypertension and overall comorbidities, and admitted to intensive care. Ferritin level increased with older age, increasing proportion of hypertensive study participants, and increasing proportion of mortality. Compared to moderate cases, severe COVID-19 cases had lower hemoglobin [weighted mean difference (WMD), - 4.08 g/L (95% CI - 5.12; - 3.05)] and red blood cell count [WMD, - 0.16 × 1012 /L (95% CI - 0.31; - 0.014)], and higher ferritin [WMD, - 473.25 ng/mL (95% CI 382.52; 563.98)] and red cell distribution width [WMD, 1.82% (95% CI 0.10; 3.55)]. A significant difference in mean ferritin levels of 606.37 ng/mL (95% CI 461.86; 750.88) was found between survivors and non-survivors, but not in hemoglobin levels. Future studies should explore the impact of iron metabolism and anemia in the pathophysiology, prognosis, and treatment of COVID-19.
Keywords: Anemia; Covid-19; Ferritin; Hemoglobin; Iron; Prognosis.
Conflict of interest statement
Dr. Michele F. Eisenga has received funding from Vitam Pharma. Other authors declare no conflicts of interest.
Figures

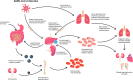
References
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical

