Anticoagulation practice patterns in COVID-19: A global survey
- PMID: 32838111
- PMCID: PMC7361754
- DOI: 10.1002/rth2.12414
Anticoagulation practice patterns in COVID-19: A global survey
Abstract
Background: Best practice for prevention, diagnosis, and management of venous thromboembolism (VTE) in patients with coronavirus disease 2019 (COVID-19) is unknown due to limited published data in this population.
Objectives: We aimed to assess current global practice and experience in management of COVID-19-associated coagulopathy to identify information to guide prospective and randomized studies.
Methods: Physicians were queried about their current approach to prophylaxis, diagnosis, and treatment of VTE in patients with COVID-19 using an online survey tool distributed through multiple international organizations between April 10 and 14, 2020.
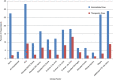
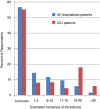
Results: Five hundred fifteen physicians from 41 countries responded. The majority of respondents (78%) recommended prophylactic anticoagulation for all hospitalized patients with COVID-19, with most recommending use of low-molecular-weight heparin or unfractionated heparin. Significant practice variation was found regarding the need for dose escalation of anticoagulation outside the setting of confirmed or suspected VTE. Respondents reported the use of bedside testing when unable to perform standard diagnostic imaging for diagnosis of VTE. Two hundred ninety-one respondents reported observing thrombotic complications in their patients, with 64% noting that the complication was pulmonary embolism. Of the 44% of respondents who estimated incidence of thrombosis in patients with COVID-19 in their hospital, estimates ranged widely from 1% to 50%. One hundred seventy-four respondents noted bleeding complications (34% minor bleeding, 14% clinically relevant nonmajor bleeding, and 12% major bleeding).
Conclusion: Well-designed epidemiologic studies are urgently needed to understand the incidence and risk factors of VTE and bleeding complications in patients with COVID-19. Randomized clinical trials addressing use of anticoagulation are also needed.
Keywords: COVID‐19; anticoagulants; bleeding; blood coagulation; venous thromboembolism.
© 2020 The Authors. Research and Practice in Thrombosis and Haemostasis published by Wiley Periodicals LLC on behalf of International Society on Thrombosis and Haemostasis.
Figures

References
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Miscellaneous

