Current Practice and Emerging Molecular Imaging Technologies in Oral Cancer Screening
- PMID: 32852263
- PMCID: PMC6287312
- DOI: 10.1177/1536012118808644
Current Practice and Emerging Molecular Imaging Technologies in Oral Cancer Screening
Abstract
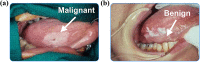
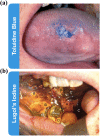
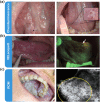
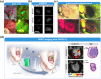
Oral cancer is one of the most common cancers globally. Survival rates for patients are directly correlated with stage of diagnosis; despite this knowledge, 60% of individuals are presenting with late-stage disease. Currently, the initial evaluation of a questionable lesion is performed by a conventional visual examination with white light. If a lesion is deemed suspicious, a biopsy is taken for diagnosis. However, not all lesions present suspicious under visual white light examination, and there is limited specificity in differentiating between benign and malignant transformations. Several vital dyes, light-based detection systems, and cytology evaluation methods have been formulated to aid in the visualization process, but their lack of specific biomarkers resulted in high false-positive rates and thus limits their reliability as screening and guidance tools. In this review, we will analyze the current methodologies and demonstrate the need for specific intraoral imaging agents to aid in screening and diagnosis to identify patients earlier. Several novel molecular imaging agents will be presented as, by result of their molecular targeting, they aim to have high specificity for tumor pathways and can support in identifying dysplastic/cancerous lesions and guiding visualization of biopsy sites. Imaging agents that are easy to use, inexpensive, noninvasive, and specific can be utilized to increase the number of patients who are screened and monitored in a variety of different environments, with the ultimate goal of increasing early detection.
Keywords: conventional oral examination (COE); molecular markers; molecularly targeted approaches; oral squamous cell carcinoma (OSCC); specificity; vital dyes.
Conflict of interest statement
Figures

References
-
- Bagan J, Sarrion G, Jimenez Y. Oral cancer: clinical features. Oral Oncol. 2010;46(6):414–417. - PubMed
-
- Warnakulasuriya S. Global epidemiology of oral and oropharyngeal cancer. Oral Oncol. 2009;45(4-5):309–316. - PubMed
-
- Ferlay J, Shin HR, Bray F, Forman D, Mathers C, Parkin DM. Estimates of worldwide burden of cancer in 2008: GLOBOCAN 2008. Int J Cancer. 2010;127(12):2893–2917. - PubMed
-
- Shield KD, Ferlay J, Jemal A, et al. The global incidence of lip, oral cavity, and pharyngeal cancers by subsite in 2012. CA Cancer J Clin. 2017;67(1):51–64. - PubMed
Grants and funding
LinkOut - more resources
Full Text Sources

