Household spraying in cholera outbreaks: Insights from three exploratory, mixed-methods field effectiveness evaluations
- PMID: 32866145
- PMCID: PMC7485970
- DOI: 10.1371/journal.pntd.0008661
Household spraying in cholera outbreaks: Insights from three exploratory, mixed-methods field effectiveness evaluations
Abstract
Household spraying is a commonly implemented, yet an under-researched, cholera response intervention where a response team sprays surfaces in cholera patients' houses with chlorine. We conducted mixed-methods evaluations of three household spraying programs in the Democratic Republic of Congo and Haiti, including 18 key informant interviews, 14 household surveys and observations, and 418 surface samples collected before spraying, 30 minutes and 24 hours after spraying. The surfaces consistently most contaminated with Vibrio cholerae were food preparation areas, near the patient's bed and the latrine. Effectiveness varied between programs, with statistically significant reductions in V. cholerae concentrations 30 minutes after spraying in two programs. Surface contamination after 24 hours was variable between households and programs. Program challenges included difficulty locating households, transportation and funding limitations, and reaching households quickly after case presentation (disinfection occurred 2-6 days after reported cholera onset). Program advantages included the concurrent deployment of hygiene promotion activities. Further research is indicated on perception, recontamination, cost-effectiveness, viable but nonculturable V. cholerae, and epidemiological coverage. We recommend that, if spraying is implemented, spraying agents should: disinfect surfaces systematically until wet using 0.2/2.0% chlorine solution, including kitchen spaces, patients' beds, and latrines; arrive at households quickly; and, concurrently deploy hygiene promotion activities.
Conflict of interest statement
The authors have declared that no competing interests exist.
Figures

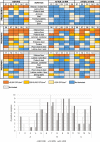
References
-
- Sack DA, Sack RB, Nair GB, Siddique AK. Cholera. The Lancet. 2004;363(9404):223. - PubMed
-
- WHO. Ten Facts on Cholera [Internet]. 2016 [cited 2016 Oct 23]. Available from: http://www.who.int/features/factfiles/cholera/en/
-
- WHO. Cholera—Fact sheet. [Internet]. Media centre. 2016 [cited 2018 Feb 24]. Available from: http://www.who.int/mediacentre/factsheets/fs107/en/
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical

