Racial, Economic, and Health Inequality and COVID-19 Infection in the United States
- PMID: 32875535
- PMCID: PMC7462354
- DOI: 10.1007/s40615-020-00833-4
Racial, Economic, and Health Inequality and COVID-19 Infection in the United States
Abstract
Objectives: There is preliminary evidence of racial and social economic disparities in the population infected by and dying from COVID-19. The goal of this study is to report the associations of COVID-19 with respect to race, health, and economic inequality in the United States.
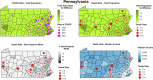
Methods: We performed an ecological study of the associations between infection and mortality rate of COVID-19 and demographic, socioeconomic, and mobility variables from 369 counties (total population, 102,178,117 [median, 73,447; IQR, 30,761-256,098]) from the seven most affected states (Michigan, New York, New Jersey, Pennsylvania, California, Louisiana, Massachusetts).
Results: The risk factors for infection and mortality are different. Our analysis shows that counties with more diverse demographics, higher population, education, income levels, and lower disability rates were at a higher risk of COVID-19 infection. However, counties with higher proportion with disability and poverty rates had a higher death rate. African Americans were more vulnerable to COVID-19 than other ethnic groups (1981 African American infected cases versus 658 Whites per million). Data on mobility changes corroborate the impact of social distancing.
Conclusion: Our study provides evidence of racial, economic, and health inequality in the population infected by and dying from COVID-19. These observations might be due to the workforce of essential services, poverty, and access to care. Counties in more urban areas are probably better equipped at providing care. The lower rate of infection, but a higher death rate in counties with higher poverty and disability could be due to lower levels of mobility, but a higher rate of comorbidities and health care access.
Keywords: COVID-19; Ecological-based study; Economic inequality; Health status disparities; Healthcare disparities; Population-based analysis; Racial disparity; Socioeconomic factors; United States.
Conflict of interest statement
The authors declare that they have no conflict of interest.
Figures
Update of
-
Racial, Economic and Health Inequality and COVID-19 Infection in the United States.medRxiv [Preprint]. 2020 May 1:2020.04.26.20079756. doi: 10.1101/2020.04.26.20079756. medRxiv. 2020. Update in: J Racial Ethn Health Disparities. 2021 Jun;8(3):732-742. doi: 10.1007/s40615-020-00833-4. PMID: 32511647 Free PMC article. Updated. Preprint.
References
-
- Branswell H, Joseph A. WHO declares the coronavirus outbreak a pandemic. n.d. Retrieved April 14, 2020, from https://www.statnews.com/2020/03/11/who-declares-the-coronavirus-outbrea...
-
- JHU. Coronavirus COVID-19 global cases by the center for systems science and engineering [Internet]. Johns Hopkins Univ. 2020;Available from: https://coronavirus.jhu.edu/map.html
-
- Zhu L, She ZG, Cheng X, Qin JJ, Zhang XJ, Cai J, Lei F, Wang H, Xie J, Wang W, Li H. Association of Blood Glucose Control and Outcomes in Patients with COVID-19 and Pre-existing Type 2 Diabetes. Cell Metabolism. 2020 May 1. https://www.cell.com/cell-metabolism/pdfExtended/S1550-4131(20)30238-2. - PMC - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical