Endoscopic ultrasound-guided fiducial marker placement in pancreatic cancer: A systematic review and meta-analysis
- PMID: 32879658
- PMCID: PMC7443822
- DOI: 10.4253/wjge.v12.i8.231
Endoscopic ultrasound-guided fiducial marker placement in pancreatic cancer: A systematic review and meta-analysis
Abstract
Background: Pancreatic cancer (PC) mortality remains high despite advances in therapy. Combination chemoradiotherapy offers modest survival benefit over monotherapy with either. Fiducial markers serve as needed landmarks for image-guided radiotherapy (IGRT). Traditionally, these markers were placed surgically or percutaneously with limitations of each. Endoscopic ultrasound-guided placement overcomes these limitations.
Aim: To evaluate the safety, efficacy, and feasibility of endoscopic ultrasound (EUS)-guided fiducial placement for PC undergoing IGRT.
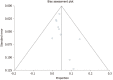
Methods: Articles were searched in MEDLINE, PubMed, and Ovid journals. Pooling was conducted by fixed and random effects models. Heterogeneity was assessed using Cochran's Q test based upon inverse variance weights.
Results: Initial search identified 1024 reference articles for EUS-guided fiducial placement in PC. Of these, 261 relevant articles were reviewed. Data was extracted from 11 studies (n = 820) meeting inclusion criteria. Pooled proportion of successful placement was 96.27% (95%CI: 95.35-97.81) with fiducial migration rates low at 4.33% (95%CI: 2.45-6.71). Adverse event rates remained low, with overall pooled proportion of 4.85% (95%CI: 3.04-7.03).
Conclusion: EUS-guided placement of fiducial markers for IGRT of PC is safe, feasible, and efficacious. The ability to target deep structures under direct visualization while remaining minimally invasive are added benefits. Moreover, the ability to perform fine needle aspiration or celiac plexus neurolysis add value and increase patient-care efficiency. Whether EUS-guided fiducial placement improves outcomes in IGRT or offers any mortality benefits over traditional placement remains unknown and future studies are needed.
Keywords: Endoscopic ultrasound; Fiducial marker; Image-guided radiotherapy; Meta-analysis; Pancreatic cancer; Systematic review.
©The Author(s) 2020. Published by Baishideng Publishing Group Inc. All rights reserved.
Figures

Similar articles
-
EUS-guided fiducial placement for stereotactic body radiotherapy in locally advanced and recurrent pancreatic cancer.Gastrointest Endosc. 2010 Jun;71(7):1178-84. doi: 10.1016/j.gie.2009.12.020. Epub 2010 Apr 1. Gastrointest Endosc. 2010. PMID: 20362284
-
Endoscopic ultrasound-guided fiducial marker placement for image-guided radiation therapy without fluoroscopy: safety and technical feasibility.Endosc Int Open. 2016 Mar;4(3):E378-82. doi: 10.1055/s-0042-100720. Epub 2016 Mar 3. Endosc Int Open. 2016. PMID: 27004258 Free PMC article.
-
Endoscopic ultrasound-guided fiducial marker placement for neoadjuvant chemoradiation therapy for resectable pancreatic cancer.World J Gastrointest Oncol. 2020 Jul 15;12(7):768-781. doi: 10.4251/wjgo.v12.i7.768. World J Gastrointest Oncol. 2020. PMID: 32864044 Free PMC article. Clinical Trial.
-
EUS-guided fiducial placement for GI malignancies: a systematic review and meta-analysis.Gastrointest Endosc. 2019 Apr;89(4):659-670.e18. doi: 10.1016/j.gie.2018.10.047. Epub 2018 Nov 13. Gastrointest Endosc. 2019. PMID: 30445001
-
Endoscopic ultrasound-guided fiducial markers and brachytherapy.Gastrointest Endosc Clin N Am. 2012 Apr;22(2):325-31, x. doi: 10.1016/j.giec.2012.04.012. Gastrointest Endosc Clin N Am. 2012. PMID: 22632954 Review.
Cited by
-
EUS-guided interventional therapies for pancreatic diseases.Front Med (Lausanne). 2024 Jan 8;10:1329676. doi: 10.3389/fmed.2023.1329676. eCollection 2023. Front Med (Lausanne). 2024. PMID: 38259846 Free PMC article. Review.
-
Hot topics in therapeutic EUS.Endosc Ultrasound. 2022 May-Jun;11(3):153-155. doi: 10.4103/EUS-D-22-00080. Endosc Ultrasound. 2022. PMID: 35708368 Free PMC article. No abstract available.
-
Endoscopic Ultrasound-Guided Fiducial Placement for Stereotactic Body Radiation Therapy in Pancreatic Malignancy.Clin Endosc. 2021 May;54(3):314-323. doi: 10.5946/ce.2021.102. Epub 2021 May 28. Clin Endosc. 2021. PMID: 34082487 Free PMC article.
-
Locoregional therapies and their effects on the tumoral microenvironment of pancreatic ductal adenocarcinoma.World J Gastroenterol. 2022 Apr 7;28(13):1288-1303. doi: 10.3748/wjg.v28.i13.1288. World J Gastroenterol. 2022. PMID: 35645539 Free PMC article. Review.
-
Endoscopic Ultrasound-Guided Fiducial Placement for Stereotactic Body Radiation Therapy in Patients with Pancreatic Cancer.Cancers (Basel). 2023 Nov 10;15(22):5355. doi: 10.3390/cancers15225355. Cancers (Basel). 2023. PMID: 38001615 Free PMC article.
References
-
- Siegel RL, Miller KD, Jemal A. Cancer statistics, 2019. CA Cancer J Clin. 2019;69:7–34. - PubMed
-
- Stephens J, Kuhn J, O'Brien J, Preskitt J, Derrick H, Fisher T, Fuller R, Lieberman Z. Surgical morbidity, mortality, and long-term survival in patients with peripancreatic cancer following pancreaticoduodenectomy. Am J Surg. 1997;174:600–3; discussion 603-4. - PubMed
-
- Varadarajulu S, Eloubeidi MA. The role of endoscopic ultrasonography in the evaluation of pancreatico-biliary cancer. Gastrointest Endosc Clin N Am. 2005;15:497–511, viii-viix. - PubMed
-
- Mosca F, Giulianotti PC, Balestracci T, Di Candio G, Pietrabissa A, Sbrana F, Rossi G. Long-term survival in pancreatic cancer: pylorus-preserving versus Whipple pancreatoduodenectomy. Surgery. 1997;122:553–566. - PubMed
LinkOut - more resources
Full Text Sources

