Acute kidney injury in renal transplant recipients undergoing cardiac surgery
- PMID: 32892219
- PMCID: PMC7771983
- DOI: 10.1093/ndt/gfaa063
Acute kidney injury in renal transplant recipients undergoing cardiac surgery
Abstract
Background: Acute kidney injury (AKI) is a key risk factor for chronic kidney disease in the general population, but has not been investigated in detail among renal transplant recipients (RTRs). We investigated the incidence, severity and risk factors for AKI following cardiac surgery among RTRs compared with non-RTRs with otherwise similar clinical characteristics.
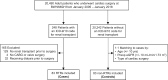
Methods: We conducted a retrospective cohort study of RTRs (n = 83) and non-RTRs (n = 83) who underwent cardiac surgery at two major academic medical centers. Non-RTRs were matched 1:1 to RTRs by age, preoperative (preop) estimated glomerular filtration rate and type of cardiac surgery. We defined AKI according to Kidney Disease: Improving Global Outcomes criteria.
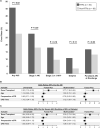
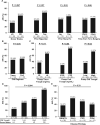
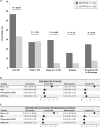
Results: RTRs had a higher rate of AKI following cardiac surgery compared with non-RTRs [46% versus 28%; adjusted odds ratio 2.77 (95% confidence interval 1.36-5.64)]. Among RTRs, deceased donor (DD) versus living donor (LD) status, as well as higher versus lower preop calcineurin inhibitor (CNI) trough levels, were associated with higher rates of AKI (57% versus 33% among DD-RTRs versus LD-RTRs; P = 0.047; 73% versus 36% among RTRs with higher versus lower CNI trough levels, P = 0.02). The combination of both risk factors (DD status and higher CNI trough level) had an additive effect (88% AKI incidence among patients with both risk factors versus 25% incidence among RTRs with neither risk factor, P = 0.004).
Conclusions: RTRs have a higher risk of AKI following cardiac surgery compared with non-RTRs with otherwise similar characteristics. Among RTRs, DD-RTRs and those with higher preop CNI trough levels are at the highest risk.
Keywords: acute kidney injury; calcineurin inhibitor; cardiac surgery; kidney transplant; renal transplant.
© The Author(s) 2020. Published by Oxford University Press on behalf of ERA-EDTA. All rights reserved.
Figures

References
-
- Hart A, Smith JM, Skeans MA. et al. OPTN/SRTR 2017 annual data report: kidney. Am J Transplant 2019; 19 (Suppl 2): 19–123 - PubMed
-
- de Mattos AM, Olyaei AJ, Bennett WM.. Nephrotoxicity of immunosuppressive drugs: long-term consequences and challenges for the future. Am J Kidney Dis 2000; 35: 333–346 - PubMed
-
- Naesens M, Kuypers DR, Sarwal M.. Calcineurin inhibitor nephrotoxicity. Clin J Am Soc Nephrol 2009; 4: 481–508 - PubMed
-
- Chapman JR, O’Connell PJ, Nankivell BJ.. Chronic renal allograft dysfunction. J Am Soc Nephrol 2005; 16: 3015–3026 - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Research Materials

