R0 resection following chemo (radio)therapy improves survival of primary inoperable pancreatic cancer patients. Interim results of the German randomized CONKO-007± trial
- PMID: 32914237
- PMCID: PMC7801312
- DOI: 10.1007/s00066-020-01680-2
R0 resection following chemo (radio)therapy improves survival of primary inoperable pancreatic cancer patients. Interim results of the German randomized CONKO-007± trial
Abstract
Purpose: Chemotherapy with or without radiotherapy is the standard in patients with initially nonmetastatic unresectable pancreatic cancer. Additional surgery is in discussion. The CONKO-007 multicenter randomized trial examines the value of radiotherapy. Our interim analysis showed a significant effect of surgery, which may be relevant to clinical practice.
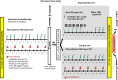
Methods: One hundred eighty patients received induction chemotherapy (gemcitabine or FOLFIRINOX). Patients without tumor progression were randomized to either chemotherapy alone or to concurrent chemoradiotherapy. At the end of therapy, a panel of five independent pancreatic surgeons judged the resectability of the tumor.
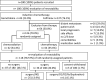
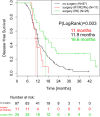
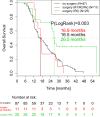
Results: Following induction chemotherapy, 126/180 patients (70.0%) were randomized to further treatment. Following study treatment, 36/126 patients (28.5%) underwent surgery; (R0: 25/126 [19.8%]; R1/R2/Rx [n = 11/126; 6.1%]). Disease-free survival (DFS) and overall survival (OS) were significantly better for patients with R0 resected tumors (median DFS and OS: 16.6 months and 26.5 months, respectively) than for nonoperated patients (median DFS and OS: 11.9 months and 16.5 months, respectively; p = 0.003). In the 25 patients with R0 resected tumors before treatment, only 6/113 (5.3%) of the recommendations of the panel surgeons recommended R0 resectability, compared with 17/48 (35.4%) after treatment (p < 0.001).
Conclusion: Tumor resectability of pancreatic cancer staged as unresectable at primary diagnosis should be reassessed after neoadjuvant treatment. The patient should undergo surgery if a resectability is reached, as this significantly improves their prognosis.
Keywords: Neoadjuvant chemoradiotherapy; Pancreatic adenocarcinoma; Prospective randomized multicenter trial; Surgery; Tumor resectability.
Conflict of interest statement
R. Fietkau, R. Grützmann, U.A. Wittel, R.S. Croner, L. Jacobasch, U.P. Neumann, A. Reinacher-Schick, D. Imhoff, S. Boeck, L. Keilholz, H. Oettle, W.M. Hohenberger, H. Golcher, W.O. Bechstein, W. Uhl, A. Pirkl, W. Adler, S. Semrau, S. Rutzner, M. Ghadimi, and D. Lubgan declare that they have no competing interests.
Figures
Comment in
-
[Preoperative radiochemotherapy improves oncological results in borderline resectable pancreatic cancer, but not overall survival in resectable cancers : Results from the Dutch PREOPANC study].Strahlenther Onkol. 2021 Jan;197(1):85-88. doi: 10.1007/s00066-020-01717-6. Strahlenther Onkol. 2021. PMID: 33258046 Free PMC article. German. No abstract available.
References
-
- Lutz MP, Zalcberg JR, Ducreux M, Aust D, Bruno MJ, Buchler MW, Delpero JR, Gloor B, Glynne-Jones R, Hartwig W, et al. 3rd St. Gallen EORTC Gastrointestinal Cancer Conference: Consensus recommendations on controversial issues in the primary treatment of pancreatic cancer. Eur J Cancer. 2017;79:41–49. doi: 10.1016/j.ejca.2017.03.022. - DOI - PubMed
-
- Petrucciani N, Debs T, Nigri G, Giannini G, Sborlini E, Kassir R, Ben Amor I, Iannelli A, Valabrega S, D’Angelo F, et al. Pancreatectomy combined with multivisceral resection for pancreatic malignancies: is it justified? Results of a systematic review. HPB (Oxford) 2018;20(1):3–10. doi: 10.1016/j.hpb.2017.08.002. - DOI - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical

