Prediction of poor neurological outcome in comatose survivors of cardiac arrest: a systematic review
- PMID: 32915254
- PMCID: PMC7527362
- DOI: 10.1007/s00134-020-06198-w
Prediction of poor neurological outcome in comatose survivors of cardiac arrest: a systematic review
Abstract
Purpose: To assess the ability of clinical examination, blood biomarkers, electrophysiology, or neuroimaging assessed within 7 days from return of spontaneous circulation (ROSC) to predict poor neurological outcome, defined as death, vegetative state, or severe disability (CPC 3-5) at hospital discharge/1 month or later, in comatose adult survivors from cardiac arrest (CA).
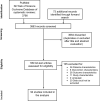
Methods: PubMed, EMBASE, Web of Science, and the Cochrane Database of Systematic Reviews (January 2013-April 2020) were searched. Sensitivity and false-positive rate (FPR) for each predictor were calculated. Due to heterogeneities in recording times, predictor thresholds, and definition of some predictors, meta-analysis was not performed.
Results: Ninety-four studies (30,200 patients) were included. Bilaterally absent pupillary or corneal reflexes after day 4 from ROSC, high blood values of neuron-specific enolase from 24 h after ROSC, absent N20 waves of short-latency somatosensory-evoked potentials (SSEPs) or unequivocal seizures on electroencephalogram (EEG) from the day of ROSC, EEG background suppression or burst-suppression from 24 h after ROSC, diffuse cerebral oedema on brain CT from 2 h after ROSC, or reduced diffusion on brain MRI at 2-5 days after ROSC had 0% FPR for poor outcome in most studies. Risk of bias assessed using the QUIPS tool was high for all predictors.
Conclusion: In comatose resuscitated patients, clinical, biochemical, neurophysiological, and radiological tests have a potential to predict poor neurological outcome with no false-positive predictions within the first week after CA. Guidelines should consider the methodological concerns and limited sensitivity for individual modalities. (PROSPERO CRD42019141169).
Keywords: Cardiac arrest; Clinical examination; Coma; Computed tomography; Diffusion magnetic resonance imaging; Neuron-specific enolase; Prognosis; Somatosensory-evoked potentials.
Conflict of interest statement
Claudio Sandroni is a member of the Editorial Board of Intensive Care Medicine and co-author of studies included in the present review. Massimo Antonelli has received research grants from GE and Estor, and honoraria for board participation from Toray, Pfizer, and Intersurgical. None of these COIs are related to the topic of the present review. Fabio Silvio Taccone is a Scientific Advisor for Neuroptics and Nihon Khoden, and co-author of studies included in the present review. Mauro Oddo is a Scientific Advisor for Neuroptics and co-author of studies included in the present review. Tobias Cronberg, Cornelia WE Hoedemaekers, and Erik Westhall are co-authors of studies included in the present review. The other authors declare that they have no competing interests.
References
-
- Lemiale V, Dumas F, Mongardon N, Giovanetti O, Charpentier J, Chiche JD, Carli P, Mira JP, Nolan J, Cariou A. Intensive care unit mortality after cardiac arrest: the relative contribution of shock and brain injury in a large cohort. Intensive Care Med. 2013;39:1972–1980. doi: 10.1007/s00134-013-3043-4. - DOI - PubMed
-
- Dragancea I, Wise MP, Al-Subaie N, Cranshaw J, Friberg H, Glover G, Pellis T, Rylance R, Walden A, Nielsen N, Cronberg T. Protocol-driven neurological prognostication and withdrawal of life-sustaining therapy after cardiac arrest and targeted temperature management. Resuscitation. 2017;117:50–57. doi: 10.1016/j.resuscitation.2017.05.014. - DOI - PubMed
-
- Sandroni C, Cavallaro F, Callaway CW, D'Arrigo S, Sanna T, Kuiper MA, Biancone M, Della Marca G, Farcomeni A, Nolan JP. Predictors of poor neurological outcome in adult comatose survivors of cardiac arrest: a systematic review and meta-analysis. Part 2: Patients treated with therapeutic hypothermia. Resuscitation. 2013;84:1324–1338. doi: 10.1016/j.resuscitation.2013.06.020. - DOI - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous