Regulation of hepatic insulin signaling and glucose homeostasis by sphingosine kinase 2
- PMID: 32917816
- PMCID: PMC7533871
- DOI: 10.1073/pnas.2007856117
Regulation of hepatic insulin signaling and glucose homeostasis by sphingosine kinase 2
Abstract
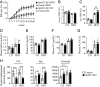
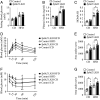
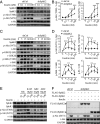
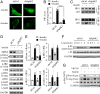
Sphingolipid dysregulation is often associated with insulin resistance, while the enzymes controlling sphingolipid metabolism are emerging as therapeutic targets for improving insulin sensitivity. We report herein that sphingosine kinase 2 (SphK2), a key enzyme in sphingolipid catabolism, plays a critical role in the regulation of hepatic insulin signaling and glucose homeostasis both in vitro and in vivo. Hepatocyte-specific Sphk2 knockout mice exhibit pronounced insulin resistance and glucose intolerance. Likewise, SphK2-deficient hepatocytes are resistant to insulin-induced activation of the phosphoinositide 3-kinase (PI3K)-Akt-FoxO1 pathway and elevated hepatic glucose production. Mechanistically, SphK2 deficiency leads to the accumulation of sphingosine that, in turn, suppresses hepatic insulin signaling by inhibiting PI3K activation in hepatocytes. Either reexpressing functional SphK2 or pharmacologically inhibiting sphingosine production restores insulin sensitivity in SphK2-deficient hepatocytes. In conclusion, the current study provides both experimental findings and mechanistic data showing that SphK2 and sphingosine in the liver are critical regulators of insulin sensitivity and glucose homeostasis.
Keywords: ceramide; hepatocyte; insulin resistance; sphingolipids; type 2 diabetes.
Copyright © 2020 the Author(s). Published by PNAS.
Conflict of interest statement
The authors declare no competing interest.
Figures

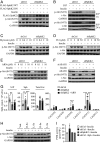
Similar articles
-
Activation of sphingosine kinase 2 by endoplasmic reticulum stress ameliorates hepatic steatosis and insulin resistance in mice.Hepatology. 2015 Jul;62(1):135-46. doi: 10.1002/hep.27804. Epub 2015 Apr 22. Hepatology. 2015. PMID: 25808625
-
Sphingosine kinase 2 regulates insulin receptor trafficking in hepatocytes.Exp Biol Med (Maywood). 2023 Jan;248(1):44-51. doi: 10.1177/15353702221131886. Epub 2022 Nov 20. Exp Biol Med (Maywood). 2023. PMID: 36408724 Free PMC article.
-
Sphingosine 1-phosphate (S1P) regulates glucose-stimulated insulin secretion in pancreatic beta cells.J Biol Chem. 2012 Apr 13;287(16):13457-64. doi: 10.1074/jbc.M111.268185. Epub 2012 Mar 2. J Biol Chem. 2012. PMID: 22389505 Free PMC article.
-
Regulation and function of sphingosine kinase 2 in diseases.Histol Histopathol. 2018 May;33(5):433-445. doi: 10.14670/HH-11-939. Epub 2017 Oct 19. Histol Histopathol. 2018. PMID: 29057430 Review.
-
Regulation of sphingosine kinase and sphingolipid signaling.Trends Biochem Sci. 2011 Feb;36(2):97-107. doi: 10.1016/j.tibs.2010.08.001. Epub 2010 Oct 1. Trends Biochem Sci. 2011. PMID: 20870412 Review.
Cited by
-
Revealing the Hypoglycemic Effects and Mechanism of GABA-Rich Germinated Adzuki Beans on T2DM Mice by Untargeted Serum Metabolomics.Front Nutr. 2021 Dec 14;8:791191. doi: 10.3389/fnut.2021.791191. eCollection 2021. Front Nutr. 2021. PMID: 34970582 Free PMC article.
-
Targeting the SphK1/S1P/PFKFB3 axis suppresses hepatocellular carcinoma progression by disrupting glycolytic energy supply that drives tumor angiogenesis.J Transl Med. 2024 Jan 10;22(1):43. doi: 10.1186/s12967-023-04830-z. J Transl Med. 2024. PMID: 38200582 Free PMC article.
-
Identification of circulating sphingosine kinase-related metabolites for prediction of type 2 diabetes.J Transl Med. 2021 Sep 16;19(1):393. doi: 10.1186/s12967-021-03066-z. J Transl Med. 2021. PMID: 34530846 Free PMC article.
-
Ceramide Regulates Anti-Tumor Mechanisms of Erianin in Androgen-Sensitive and Castration-Resistant Prostate Cancers.Front Oncol. 2021 Sep 17;11:738078. doi: 10.3389/fonc.2021.738078. eCollection 2021. Front Oncol. 2021. PMID: 34604081 Free PMC article.
-
Suppression of endothelial ceramide de novo biosynthesis by Nogo-B contributes to cardiometabolic diseases.Nat Commun. 2025 Feb 25;16(1):1968. doi: 10.1038/s41467-025-56869-9. Nat Commun. 2025. PMID: 40000621 Free PMC article.
References
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical
Molecular Biology Databases
Research Materials
Miscellaneous

