Prognostic value of lactate dehydrogenase for in-hospital mortality in severe and critically ill patients with COVID-19
- PMID: 32922185
- PMCID: PMC7484664
- DOI: 10.7150/ijms.47604
Prognostic value of lactate dehydrogenase for in-hospital mortality in severe and critically ill patients with COVID-19
Abstract
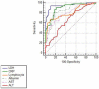
Background: Lactate dehydrogenase (LDH) has been proved to be a prognostic factor for the severity and poor outcomes of coronavirus disease 2019 (COVID-19). In most studies, patients with various levels of COVID-19 severity were pooled and analyzed which may prevent accurate evaluation of the relationship between LDH and disease progression and in-hospital death. In this study, we aimed to evaluate the association of LDH with in-hospital mortality in severe and critically ill patients with COVID-19. Methods: This single-center retrospective study enrolled 119 patients. Survival curves were plotted using Kaplan-Meier method and compared by log-rank test. Multivariate Cox regression models were used to determine the independent risk factors for in-hospital mortality. Receiver-operator curves (ROCs) were constructed to evaluate the predictive accuracy of LDH and other prognostic biomarkers. Results: Compared to the survival group, LDH levels in the dead group were significantly higher [559.5 (172, 7575) U/L vs 228 (117, 490) U/L, (P < 0.001)]. In Multivariate Cox regression, it remained an independent risk factor for in-hospital mortality (Hazard ratio 5.985, 95.0%CI: 1.498-23.905; P=0.011). A cutoff value of 353.5 U/L predicted the in-hospital mortality with a sensitivity of 94.4% and a specificity of 89.2% respectively. Conclusion: LDH is a favorable prognostic biomarker with high accuracy for predicting in-hospital mortality in severe and critically ill patients with COVID-19. This may direct physicians worldwide to effectively prioritize resources for patients at high risk of death and to implement more aggressive treatments at an earlier phase to save patients' lives.
Keywords: COVID-19; lactate dehydrogenase; multiple organ dysfunction; prognostic value.
© The author(s).
Conflict of interest statement
Competing Interests: The authors have declared that no competing interest exists.
Figures

Similar articles
-
Factors associated with death outcome in patients with severe coronavirus disease-19 (COVID-19): a case-control study.Int J Med Sci. 2020 May 18;17(9):1281-1292. doi: 10.7150/ijms.46614. eCollection 2020. Int J Med Sci. 2020. PMID: 32547323 Free PMC article.
-
IL-6-based mortality risk model for hospitalized patients with COVID-19.J Allergy Clin Immunol. 2020 Oct;146(4):799-807.e9. doi: 10.1016/j.jaci.2020.07.009. Epub 2020 Jul 22. J Allergy Clin Immunol. 2020. PMID: 32710975 Free PMC article.
-
CURB-65 may serve as a useful prognostic marker in COVID-19 patients within Wuhan, China: a retrospective cohort study.Epidemiol Infect. 2020 Oct 1;148:e241. doi: 10.1017/S0950268820002368. Epidemiol Infect. 2020. PMID: 32998791 Free PMC article.
-
Laboratory findings of COVID-19: a systematic review and meta-analysis.Scand J Clin Lab Invest. 2020 Oct;80(6):441-447. doi: 10.1080/00365513.2020.1768587. Epub 2020 May 23. Scand J Clin Lab Invest. 2020. PMID: 32449374 Free PMC article.
-
Lactate dehydrogenase levels predict coronavirus disease 2019 (COVID-19) severity and mortality: A pooled analysis.Am J Emerg Med. 2020 Sep;38(9):1722-1726. doi: 10.1016/j.ajem.2020.05.073. Epub 2020 May 27. Am J Emerg Med. 2020. PMID: 32738466 Free PMC article. Review.
Cited by
-
Coronavirus Disease Clinical and Laboratory Parameters: Dismembering the Values Reveals Outcomes.Cureus. 2021 Mar 5;13(3):e13720. doi: 10.7759/cureus.13720. Cureus. 2021. PMID: 33833931 Free PMC article.
-
Relationship Between Blood Lipid Levels and Mortality in Hospitalized COVID-19 Patients.Angiology. 2022 Sep;73(8):724-733. doi: 10.1177/00033197211072346. Epub 2022 Feb 6. Angiology. 2022. PMID: 35124978 Free PMC article.
-
Increased risk of poor clinical outcome in COVID-19 patients with diabetes mellitus and in-hospital mortality predictors: A retrospective cohort from a tertiary hospital in Indonesia.Endocrinol Diabetes Metab. 2023 Nov;6(6):e454. doi: 10.1002/edm2.454. Epub 2023 Oct 9. Endocrinol Diabetes Metab. 2023. PMID: 37807699 Free PMC article.
-
Role of serum lactate as prognostic marker of mortality among emergency department patients with multiple conditions: A systematic review.SAGE Open Med. 2023 Jan 10;11:20503121221136401. doi: 10.1177/20503121221136401. eCollection 2023. SAGE Open Med. 2023. PMID: 36643203 Free PMC article. Review.
-
Impact of serum lactate dehydrogenase on the short-term prognosis of COVID-19 with pre-existing cardiovascular diseases.J Cardiol. 2022 Apr;79(4):501-508. doi: 10.1016/j.jjcc.2021.12.014. Epub 2021 Dec 28. J Cardiol. 2022. PMID: 35000825 Free PMC article.
References
-
- Feron O. Pyruvate into lactate and back: from the Warburg effect to symbiotic energy fuel exchange in cancer cells. Radiotherapy and oncology: journal of the European Society for Therapeutic Radiology and Oncology. 2009;92(3):329–33. - PubMed
-
- Glick JH Jr. Serum lactate dehydrogenase isoenzyme and total lactate dehydrogenase values in health and disease, and clinical evaluation of these tests by means of discriminant analysis. American journal of clinical pathology. 1969;52(3):320–8. - PubMed
-
- Karlsson M, Wiberg-Itzel E, Chakkarapani E, Blennow M, Winbladh B, Thoresen M. Lactate dehydrogenase predicts hypoxic ischaemic encephalopathy in newborn infants: a preliminary study. Acta paediatrica (Oslo, Norway: 1992) 2010;99(8):1139–44. - PubMed
MeSH terms
Substances
LinkOut - more resources
Full Text Sources

