Impact of a pay-for-performance scheme for long-acting reversible contraceptive (LARC) advice on contraceptive uptake and abortion in British primary care: An interrupted time series study
- PMID: 32925909
- PMCID: PMC7489538
- DOI: 10.1371/journal.pmed.1003333
Impact of a pay-for-performance scheme for long-acting reversible contraceptive (LARC) advice on contraceptive uptake and abortion in British primary care: An interrupted time series study
Abstract
Background: Long-acting reversible contraception (LARC) is among the most effective contraceptive methods, but uptake remains low even in high-income settings. In 2009/2010, a target-based pay-for-performance (P4P) scheme in Britain was introduced for primary care physicians (PCPs) to offer advice about LARC methods to a specified proportion of women attending for contraceptive care to improve contraceptive choice. We examined the impact and equity of this scheme on LARC uptake and abortions.
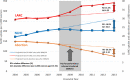
Methods and findings: We examined records of 3,281,667 women aged 13 to 54 years registered with a primary care clinic in Britain (England, Wales, and Scotland) using Clinical Practice Research Datalink (CPRD) from 2004/2005 to 2013/2014. We used interrupted time series (ITS) analysis to examine trends in annual LARC and non-LARC hormonal contraception (NLHC) uptake and abortion rates, stratified by age and deprivation groups, before and after the P4P was introduced in 2009/2010. Between 2004/2005 and 2013/2014, crude LARC uptake rates increased by 32.0% from 29.6 per 1,000 women to 39.0 per 1,000 women, compared with 18.0% decrease in NLHC uptake. LARC uptake among women of all ages increased immediately after the P4P with step change of 5.36 per 1,000 women (all values are per 1,000 women unless stated, 95% CI 5.26-5.45, p < 0.001). Women aged 20 to 24 years had the largest step change (8.40, 8.34-8.47, p < 0.001) and sustained trend increase (3.14, 3.08-3.19, p < 0.001) compared with other age groups. NLHC uptake fell in all women with a step change of -22.8 (-24.5 to -21.2, p < 0.001), largely due to fall in combined hormonal contraception (CHC; -15.0, -15.5 to -14.5, p < 0.001). Abortion rates in all women fell immediately after the P4P with a step change of -2.28 (-2.98 to -1.57, p = 0.002) and sustained decrease in trend of -0.88 (-1.12 to -0.63, p < 0.001). The largest falls occurred in women aged 13 to 19 years (step change -5.04, -7.56 to -2.51, p = 0.011), women aged 20 to 24 years (step change -4.52, -7.48 to -1.57, p = 0.030), and women from the most deprived group (step change -4.40, -6.89 to -1.91, p = 0.018). We estimate that by 2013/2014, the P4P scheme resulted in an additional 4.53 LARC prescriptions per 1,000 women (relative increase of 13.4%) more than would have been expected without the scheme. There was a concurrent absolute reduction of -5.31 abortions per 1,000 women, or -38.3% relative reduction. Despite universal coverage of healthcare, some women might have obtained contraception elsewhere or had abortion procedure that was not recorded on CPRD. Other policies aiming to increase LARC use or reduce unplanned pregnancies around the same time could also explain the findings.
Conclusions: In this study, we found that LARC uptake increased and abortions fell in the period after the P4P scheme in British primary care, with additional impact for young women aged 20-24 years and those from deprived backgrounds.
Conflict of interest statement
I have read the journal's policy and the authors of this manuscript have the following competing interests: RM is an NHS general practitioner, and his practice receives funding for achieving P4P targets. His practice receives extra funding for providing a LARC service for patients registered with his practice. He has also received honoraria for writing commissioned articles for magazines and lectures at educational events paid directly by publishers or organisers of meetings but not directly by pharma. EC has nothing to disclose. AB reports grants from Dr Foster outside the submitted work. RF reports personal fees from Natural Cycles outside the submitted work. SS reports grants from NIHR School for Public Health Research, grants from NIHR Collaboration for Applied Research Collaboration North West London, during the conduct of the study; and grants from The Daily Mile Foundation, outside the submitted work; SS is an NHS general practitioner, and her practice receives funding for achieving P4P targets.
Figures
Similar articles
-
Factors that influence the choice of long-acting reversible contraceptive use among adolescents post-abortion in Chongqing, China: a cross-sectional study.J Obstet Gynaecol. 2024 Dec;44(1):2316625. doi: 10.1080/01443615.2024.2316625. Epub 2024 Feb 14. J Obstet Gynaecol. 2024. PMID: 38353518
-
Cost-benefit analysis of enhancing the uptake of long-acting reversible contraception in Australia.Aust Health Rev. 2020 Jun;44(3):385-391. doi: 10.1071/AH18190. Aust Health Rev. 2020. PMID: 31655632
-
Predictors of choosing long-acting reversible contraceptive methods when provided free-of-charge - A prospective cohort study in Finland.Contraception. 2020 Jun;101(6):370-375. doi: 10.1016/j.contraception.2020.01.018. Epub 2020 Feb 13. Contraception. 2020. PMID: 32061566
-
Uptake of long-acting reversible contraception after telemedicine delivered abortion during Covid-19.Eur J Contracept Reprod Health Care. 2022 Aug;27(4):284-288. doi: 10.1080/13625187.2022.2085680. Epub 2022 Jun 17. Eur J Contracept Reprod Health Care. 2022. PMID: 35713651 Review.
-
Acceptability of immediate postpartum and post-abortion long-acting reversible contraception provision to adolescents: A systematic review.Acta Obstet Gynecol Scand. 2021 Apr;100(4):629-640. doi: 10.1111/aogs.14129. Epub 2021 Mar 9. Acta Obstet Gynecol Scand. 2021. PMID: 33608901
Cited by
-
Preconception indicators and associations with health outcomes reported in UK routine primary care data: a systematic review.Br J Gen Pract. 2025 Jan 30;75(751):e129-e136. doi: 10.3399/BJGP.2024.0082. Print 2025 Feb. Br J Gen Pract. 2025. PMID: 38950944 Free PMC article.
-
Hidden in plain sight: A systematic review of coercion and Long-Acting Reversible Contraceptive methods (LARC).PLOS Glob Public Health. 2023 Aug 18;3(8):e0002131. doi: 10.1371/journal.pgph.0002131. eCollection 2023. PLOS Glob Public Health. 2023. PMID: 37594941 Free PMC article.
-
Using responsive feedback from routine monitoring data to guide course corrections for a family planning intervention in Nigeria.Gates Open Res. 2023 Nov 16;7:75. doi: 10.12688/gatesopenres.14591.2. eCollection 2023. Gates Open Res. 2023. PMID: 38282787 Free PMC article.
-
Sexual and reproductive health and rights of migrant women attending primary care in England: A population-based cohort study of 1.2 million individuals of reproductive age (2009-2018).J Migr Health. 2024 Jan 17;9:100214. doi: 10.1016/j.jmh.2024.100214. eCollection 2024. J Migr Health. 2024. PMID: 38327760 Free PMC article.
-
Characterising and monitoring preconception health in England: a review of national population-level indicators and core data sources.J Dev Orig Health Dis. 2022 Apr;13(2):137-150. doi: 10.1017/S2040174421000258. Epub 2021 Jun 4. J Dev Orig Health Dis. 2022. PMID: 34085623 Free PMC article. Review.
References
-
- National Statistics. Abortion Statistics England and Wales 2018. Department of Health and Social Care, 2019.
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources

