Association of Intra-arrest Transport vs Continued On-Scene Resuscitation With Survival to Hospital Discharge Among Patients With Out-of-Hospital Cardiac Arrest
- PMID: 32930759
- PMCID: PMC7492914
- DOI: 10.1001/jama.2020.14185
Association of Intra-arrest Transport vs Continued On-Scene Resuscitation With Survival to Hospital Discharge Among Patients With Out-of-Hospital Cardiac Arrest
Abstract
Importance: There is wide variability among emergency medical systems (EMS) with respect to transport to hospital during out-of-hospital cardiac arrest (OHCA) resuscitative efforts. The benefit of intra-arrest transport during resuscitation compared with continued on-scene resuscitation is unclear.
Objective: To determine whether intra-arrest transport compared with continued on-scene resuscitation is associated with survival to hospital discharge among patients experiencing OHCA.
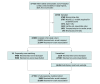
Design, setting, and participants: Cohort study of prospectively collected consecutive nontraumatic adult EMS-treated OHCA data from the Resuscitation Outcomes Consortium (ROC) Cardiac Epidemiologic Registry (enrollment, April 2011-June 2015 from 10 North American sites; follow-up until the date of hospital discharge or death [regardless of when either event occurred]). Patients treated with intra-arrest transport (exposed) were matched with patients in refractory arrest (at risk of intra-arrest transport) at that same time (unexposed), using a time-dependent propensity score. Subgroups categorized by initial cardiac rhythm and EMS-witnessed cardiac arrests were analyzed.
Exposures: Intra-arrest transport (transport initiated prior to return of spontaneous circulation), compared with continued on-scene resuscitation.
Main outcomes and measures: The primary outcome was survival to hospital discharge, and the secondary outcome was survival with favorable neurological outcome (modified Rankin scale <3) at hospital discharge.
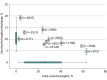
Results: The full cohort included 43 969 patients with a median age of 67 years (interquartile range, 55-80), 37% were women, 86% of cardiac arrests occurred in a private location, 49% were bystander- or EMS-witnessed, 22% had initial shockable rhythms, 97% were treated by out-of-hospital advanced life support, and 26% underwent intra-arrest transport. Survival to hospital discharge was 3.8% for patients who underwent intra-arrest transport and 12.6% for those who received on-scene resuscitation. In the propensity-matched cohort, which included 27 705 patients, survival to hospital discharge occurred in 4.0% of patients who underwent intra-arrest transport vs 8.5% who received on-scene resuscitation (risk difference, 4.6% [95% CI, 4.0%- 5.1%]). Favorable neurological outcome occurred in 2.9% of patients who underwent intra-arrest transport vs 7.1% who received on-scene resuscitation (risk difference, 4.2% [95% CI, 3.5%-4.9%]). Subgroups of initial shockable and nonshockable rhythms as well as EMS-witnessed and unwitnessed cardiac arrests all had a significant association between intra-arrest transport and lower probability of survival to hospital discharge.
Conclusions and relevance: Among patients experiencing out-of-hospital cardiac arrest, intra-arrest transport to hospital compared with continued on-scene resuscitation was associated with lower probability of survival to hospital discharge. Study findings are limited by potential confounding due to observational design.
Conflict of interest statement
Figures

Comment in
-
Challenging the "Scoop and Run" Model for Management of Out-of-Hospital Cardiac Arrest.JAMA. 2020 Sep 15;324(11):1043-1044. doi: 10.1001/jama.2020.9245. JAMA. 2020. PMID: 32930742 No abstract available.
-
Estimating Risk Ratios and Risk Differences: Alternatives to Odds Ratios.JAMA. 2020 Sep 15;324(11):1098-1099. doi: 10.1001/jama.2020.12698. JAMA. 2020. PMID: 32930746 No abstract available.
-
Out-of-Hospital Cardiac Arrest: Handle With Care-Comment on the Resuscitation Outcomes Consortium Cardiac Epidemiologic Registry.Eur Heart J. 2020 Nov 14;41(43):4165-4166. doi: 10.1093/eurheartj/ehaa862. Eur Heart J. 2020. PMID: 33241317 No abstract available.
References
-
- Link MS, Berkow LC, Kudenchuk PJ, et al. . Part 7: adult advanced cardiovascular life support: 2015 American Heart Association guidelines update for cardiopulmonary resuscitation and emergency cardiovascular care. Circulation. 2015;132(18)(suppl 2):S444-S464. doi:10.1161/CIR.0000000000000261 - DOI - PubMed
-
- Kleinman ME, Brennan EE, Goldberger ZD, et al. . Part 5: adult basic life support and cardiopulmonary resuscitation quality: 2015 American Heart Association guidelines update for cardiopulmonary resuscitation and emergency cardiovascular care. Circulation. 2015;132(18)(suppl 2):S414-S435. doi:10.1161/CIR.0000000000000259 - DOI - PubMed
-
- Panchal AR, Berg KM, Hirsch KG, et al. . 2019 American Heart Association Focused Update on Advanced Cardiovascular Life Support: use of advanced airways, vasopressors, and extracorporeal cardiopulmonary resuscitation during cardiac arrest: an update to the American Heart Association Guidelines. Circulation. 2019;140(24). doi:10.1161/CIR.0000000000000732. - DOI - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

