Effects of the COVID-19 Pandemic on Obsessive-Compulsive Symptoms Among University Students: Prospective Cohort Survey Study
- PMID: 32931444
- PMCID: PMC7528732
- DOI: 10.2196/21915
Effects of the COVID-19 Pandemic on Obsessive-Compulsive Symptoms Among University Students: Prospective Cohort Survey Study
Abstract
Background: The COVID-19 pandemic is associated with common mental health problems. However, evidence for the association between fear of COVID-19 and obsessive-compulsive disorder (OCD) is limited.
Objective: This study aimed to examine if fear of negative events affects Yale-Brown Obsessive-Compulsive Scale (Y-BOCS) scores in the context of a COVID-19-fear-invoking environment.
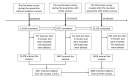
Methods: All participants were medical university students and voluntarily completed three surveys via smartphone or computer. Survey 1 was conducted on February 8, 2020, following a 2-week-long quarantine period without classes; survey 2 was conducted on March 25, 2020, when participants had been taking online courses for 2 weeks; and survey 3 was conducted on April 28, 2020, when no new cases had been reported for 2 weeks. The surveys comprised the Y-BOCS and the Zung Self-Rating Anxiety Scale (SAS); additional items included questions on demographics (age, gender, only child vs siblings, enrollment year, major), knowledge of COVID-19, and level of fear pertaining to COVID-19.
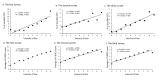
Results: In survey 1, 11.3% of participants (1519/13,478) scored ≥16 on the Y-BOCS (defined as possible OCD). In surveys 2 and 3, 3.6% (305/8162) and 3.5% (305/8511) of participants had scores indicative of possible OCD, respectively. The Y-BOCS score, anxiety level, quarantine level, and intensity of fear were significantly lower at surveys 2 and 3 than at survey 1 (P<.001 for all). Compared to those with a lower Y-BOCS score (<16), participants with possible OCD expressed greater intensity of fear and had higher SAS standard scores (P<.001). The regression linear analysis indicated that intensity of fear was positively correlated to the rate of possible OCD and the average total scores for the Y-BOCS in each survey (P<.001 for all). Multiple regressions showed that those with a higher intensity of fear, a higher anxiety level, of male gender, with sibling(s), and majoring in a nonmedicine discipline had a greater chance of having a higher Y-BOCS score in all surveys. These results were redemonstrated in the 5827 participants who completed both surveys 1 and 2 and in the 4006 participants who completed all three surveys. Furthermore, in matched participants, the Y-BOCS score was negatively correlated to changes in intensity of fear (r=0.74 for survey 2, P<.001; r=0.63 for survey 3, P=.006).
Conclusions: Our findings indicate that fear of COVID-19 was associated with a greater Y-BOCS score, suggesting that an environment (COVID-19 pandemic) × psychology (fear and/or anxiety) interaction might be involved in OCD and that a fear of negative events might play a role in the etiology of OCD.
Keywords: COVID-19; OCD; Yale-Brown Obsessive-Compulsive Scale; anxiety; fear; mental health; obsessive-compulsive disorder; university student.
©Guangjun Ji, Wenjun Wei, Kai-Chen Yue, Heng Li, Li-Jing Shi, Jian-Dong Ma, Chen-Yang He, Sheng-Sheng Zhou, Zongya Zhao, Tao Lou, Jie Cheng, Shi-Chang Yang, Xian-Zhang Hu. Originally published in the Journal of Medical Internet Research (http://www.jmir.org), 30.09.2020.
Conflict of interest statement
Conflicts of Interest: None declared.
Figures

References
-
- Lu H, Stratton CW, Tang Y. Outbreak of pneumonia of unknown etiology in Wuhan, China: The mystery and the miracle. J Med Virol. 2020 Apr;92(4):401–402. doi: 10.1002/jmv.25678. http://europepmc.org/abstract/MED/31950516 - DOI - PMC - PubMed
-
- Rogers JP, Chesney E, Oliver D, Pollak TA, McGuire P, Fusar-Poli P, Zandi MS, Lewis G, David AS. Psychiatric and neuropsychiatric presentations associated with severe coronavirus infections: a systematic review and meta-analysis with comparison to the COVID-19 pandemic. The Lancet Psychiatry. 2020 Jul;7(7):611–627. doi: 10.1016/S2215-0366(20)30203-0. https://linkinghub.elsevier.com/retrieve/pii/S2215-0366(20)30203-0 - DOI - PMC - PubMed
-
- Wang C, Pan R, Wan X, Tan Y, Xu L, Ho CS, Ho RC. Immediate Psychological Responses and Associated Factors during the Initial Stage of the 2019 Coronavirus Disease (COVID-19) Epidemic among the General Population in China. Int J Environ Res Public Health. 2020 Mar 06;17(5):e. doi: 10.3390/ijerph17051729. https://www.mdpi.com/resolver?pii=ijerph17051729 - DOI - PMC - PubMed
-
- Holes R, Yudofsky S, Roberts L. Textbook of Psychiatry, 6th ed. Arlington, VA: The American Psychiatric Publishing; 2014.
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

