Pattern of treatment of behavioural and psychological symptoms of dementia and pain: evidence on pharmacoutilization from a large real-world sample and from a centre for cognitive disturbances and dementia
- PMID: 32935181
- PMCID: PMC7803691
- DOI: 10.1007/s00228-020-02995-w
Pattern of treatment of behavioural and psychological symptoms of dementia and pain: evidence on pharmacoutilization from a large real-world sample and from a centre for cognitive disturbances and dementia
Abstract
Purpose: Data concerning the number of diagnoses and of the drugs prescribed to patients affected by dementia are still scarce. Here we test whether or not (1) prescription of symptomatic drugs against Alzheimer's disease (AD) may approximate the number of patients affected by dementia in Italy and (2) adherence to this treatment affects the pattern of prescription of drugs (i.e. antipsychotics and antidepressants) for behavioural and psychological symptoms of dementia (BPSD) and the previously reported limited prescription of analgesics.
Methods: This retrospective observational study concerns 84,235 subjects older than 60 years and registered in the provincial prescription database of the health district of Cosenza accounting for a population of 298,000 inhabitants. The prescribing pattern of antipsychotics, antidepressants, and analgesics has been investigated in patients receiving concurrent prescriptions of acetylcholinesterase inhibitors (AChEI) and/or memantine. Data from a single centre for cognitive disturbances and dementia (CDCD) in the same health district were used to explore at which stage dementia was diagnosed. The study was approved by Calabria Region Ethical Committee no. 31/2017 and registered on October 31, 2017.
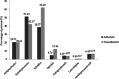
Results: The data show that 859 patients are treated with AChEI and/or memantine; 420 patients (48.89%) receive at least 80% of the recommended medications. CDCD data indicate a delay in dementia diagnosis, which often was made when the patients were moderately to severely demented (Mini Mental State Examination, MMSE ≤ 20). Adherence did not influence prescription of most of the drugs explored, but use of non-steroidal anti-inflammatory drugs was higher in non-adherent patients. Antipsychotics and antidepressants are frequently used (20.61-20.71% and 42.37-51.43%, respectively), and this, at least in part, might stem from the observed under-treatment of chronic pain (opioids are prescribed in the 4.76% and 12.46% of adherent and non-adherent patients and gabapentin and pregabalin are used in the 4.29% and 4.07% of adherent and non-adherent patients respectively), resulting in more frequent BPSD. 16.43% of patients receive antipsychotics for longer than 6-12 weeks.
Conclusion: This 2-year period study, including a wide cohort of community demented patients, shows that dementia is diagnosed late and that prevalence of BPSD prescriptions is high and not impacted by adherence to anti-dementia drugs. The rate of prescription of potentially harmful antipsychotics and antidepressants appears to be high though whether the concomitantly observed limited prescription of analgesics might be a contributing factor needs to be further investigated. Our data support the development of strategies to improve the management of BPSD.
Keywords: Alzheimer’s disease; Analgesics; Antidepressants; Antipsychotics; BPSD; Pain.
Conflict of interest statement
The authors declare that they have no conflict of interest.
Figures
Similar articles
-
Dementia Medications and Their Association with Pain Medication Use in Medicare Beneficiaries with Alzheimer's Disease/Alzheimer's Disease-Related Dementias and Chronic Pain.Drugs Aging. 2025 Mar;42(3):267-274. doi: 10.1007/s40266-025-01181-w. Epub 2025 Feb 26. Drugs Aging. 2025. PMID: 40009144 Free PMC article.
-
Sex differences in psychotropic and analgesic drug use before and after initiating treatment with acetylcholinesterase inhibitors.PLoS One. 2021 Sep 20;16(9):e0243804. doi: 10.1371/journal.pone.0243804. eCollection 2021. PLoS One. 2021. PMID: 34543268 Free PMC article.
-
Antipsychotics for BPSD: an audit of prescribing practice in a specialist psychiatric inpatient unit.Int Psychogeriatr. 2008 Aug;20(4):790-9. doi: 10.1017/S1041610208006819. Epub 2008 Feb 29. Int Psychogeriatr. 2008. PMID: 18307825
-
Pharmacological treatment of Alzheimer's Disease.Aging Clin Exp Res. 2006 Apr;18(2):158-62. doi: 10.1007/BF03327433. Aging Clin Exp Res. 2006. PMID: 16702787 Review.
-
[Pharmacological treatment of behavioral symptoms in dementia patients].Przegl Lek. 2014;71(4):215-20. Przegl Lek. 2014. PMID: 25141581 Review. Polish.
Cited by
-
Role of CGRP pathway polymorphisms in migraine: a systematic review and impact on CGRP mAbs migraine therapy.J Headache Pain. 2021 Jul 30;22(1):87. doi: 10.1186/s10194-021-01295-7. J Headache Pain. 2021. PMID: 34330208 Free PMC article.
-
Progress in the Treatment of Migraine Attacks: From Traditional Approaches to Eptinezumab.Pharmaceuticals (Basel). 2021 Sep 13;14(9):924. doi: 10.3390/ph14090924. Pharmaceuticals (Basel). 2021. PMID: 34577624 Free PMC article.
-
Efficacy of Essential Oils in Pain: A Systematic Review and Meta-Analysis of Preclinical Evidence.Front Pharmacol. 2021 Mar 1;12:640128. doi: 10.3389/fphar.2021.640128. eCollection 2021. Front Pharmacol. 2021. PMID: 33732159 Free PMC article.
-
Efficacy of therapeutic intervention with NanoBEO to manage agitation and pain in patients suffering from severe dementia: a pilot clinical trial.Front Pharmacol. 2024 Aug 1;15:1417851. doi: 10.3389/fphar.2024.1417851. eCollection 2024. Front Pharmacol. 2024. PMID: 39148533 Free PMC article.
-
Factors associated with cognitive function in patient with Alzheimer's disease with newly prescribed acetylcholinesterase inhibitors: A 1-year retrospective cohort study.Aging Med (Milton). 2024 Jun 18;7(3):312-319. doi: 10.1002/agm2.12324. eCollection 2024 Jun. Aging Med (Milton). 2024. PMID: 38975305 Free PMC article.
References
-
- Patterson C. World Alzheimer Report 2018. The state of the art of dementia research: new frontiers. London: Alzheimer’s Disease International (ADI); 2018.
-
- Scuteri D, Morrone LA, Rombola L, Avato PR, Bilia AR, Corasaniti MT, Sakurada S, Sakurada T, Bagetta G. Aromatherapy and aromatic plants for the treatment of behavioural and psychological symptoms of dementia in patients with Alzheimer’s disease: clinical evidence and possible mechanisms. Evidence-Based Complement Altern Med eCAM. 2017;2017:9416305–9416308. doi: 10.1155/2017/9416305. - DOI - PMC - PubMed
-
- Scuteri D, Rombola L, Tridico L, Mizoguchi H, Watanabe C, Sakurada T, Sakurada S, Corasaniti MT, Bagetta G, Morrone LA. Neuropharmacological properties of the essential oil of bergamot for the clinical management of pain-related BPSDs. Curr Med Chem. 2019;26(20):3764–3774. doi: 10.2174/0929867325666180307115546. - DOI - PubMed
-
- Vernooij-Dassen MJ, Moniz-Cook ED, Woods RT, De Lepeleire J, Leuschner A, Zanetti O, de Rotrou J, Kenny G, Franco M, Peters V, Iliffe S. Factors affecting timely recognition and diagnosis of dementia across Europe: from awareness to stigma. Int J Geriatric Psych. 2005;20(4):377–386. doi: 10.1002/gps.1302. - DOI - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical

