Prevalence of treatment resistance and clozapine use in early intervention services
- PMID: 32938513
- PMCID: PMC7576650
- DOI: 10.1192/bjo.2020.89
Prevalence of treatment resistance and clozapine use in early intervention services
Abstract
Background: Treatment resistance causes significant burden in psychosis. Clozapine is the only evidence-based pharmacologic intervention available for people with treatment-resistant schizophrenia; current guidelines recommend commencement after two unsuccessful trials of standard antipsychotics.
Aims: This paper aims to explore the prevalence of treatment resistance and pathways to commencement of clozapine in UK early intervention in psychosis (EIP) services.
Method: Data were taken from the National Evaluation of the Development and Impact of Early Intervention Services study (N = 1027) and included demographics, medication history and psychosis symptoms measured by the Positive and Negative Syndrome Scale (PANSS) at baseline, 6 months and 12 months. Prescribing patterns and pathways to clozapine were examined. We adopted a strict criterion for treatment resistance, defined as persistent elevated positive symptoms (a PANSS positive score ≥16, equating to at least two items of at least moderate severity), across three time points.
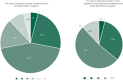
Results: A total of 143 (18.1%) participants met the definition of treatment resistance of having continuous positive symptoms over 12 months, despite treatment in EIP services. Sixty-one (7.7%) participants were treatment resistant and eligible for clozapine, having had two trials of standard antipsychotics; however, only 25 (2.4%) were prescribed clozapine over the 12-month study period. Treatment-resistant participants were more likely to be prescribed additional antipsychotic medication and polypharmacy, instead of clozapine.
Conclusions: Prevalent treatment resistance was observed in UK EIP services, but prescription of polypharmacy was much more common than clozapine. Significant delays in the commencement of clozapine may reflect a missed opportunity to promote recovery in this critical period.
Keywords: Treatment resistance; clozapine; early intervention; early psychosis; schizophrenia.
Conflict of interest statement
Supplementary material
Figures
Similar articles
-
Delays and barriers to the commencement of clozapine in eligible people with a psychotic disorder: A literature review.Early Interv Psychiatry. 2019 Feb;13(1):18-23. doi: 10.1111/eip.12683. Epub 2018 Jul 9. Early Interv Psychiatry. 2019. PMID: 29984888 Review.
-
Clozapine for treatment resistance in early psychosis: a survey of UK clinicians' training, knowledge and confidence.Ther Adv Psychopharmacol. 2022 Dec 26;12:20451253221141222. doi: 10.1177/20451253221141222. eCollection 2022. Ther Adv Psychopharmacol. 2022. PMID: 36601352 Free PMC article.
-
Randomised controlled trials of conventional antipsychotic versus new atypical drugs, and new atypical drugs versus clozapine, in people with schizophrenia responding poorly to, or intolerant of, current drug treatment.Health Technol Assess. 2006 May;10(17):iii-iv, ix-xi, 1-165. doi: 10.3310/hta10170. Health Technol Assess. 2006. PMID: 16707074 Clinical Trial.
-
Early access to clozapine in Early Intervention in Psychosis: Hope vs reality. A mixed method service analysis.Early Interv Psychiatry. 2021 Feb;15(1):193-200. doi: 10.1111/eip.12962. Epub 2020 Apr 13. Early Interv Psychiatry. 2021. PMID: 32281741
-
The acute efficacy of antipsychotics in schizophrenia: a review of recent meta-analyses.Ther Adv Psychopharmacol. 2018 Oct 8;8(11):303-318. doi: 10.1177/2045125318781475. eCollection 2018 Nov. Ther Adv Psychopharmacol. 2018. PMID: 30344997 Free PMC article. Review.
Cited by
-
Five-year illness trajectories across racial groups in the UK following a first episode psychosis.Soc Psychiatry Psychiatr Epidemiol. 2023 Apr;58(4):569-579. doi: 10.1007/s00127-023-02428-w. Epub 2023 Jan 30. Soc Psychiatry Psychiatr Epidemiol. 2023. PMID: 36717434 Free PMC article.
-
Clozapine Treatment Is Associated With Higher Prescription Rate of Antipsychotic Monotherapy and Lower Prescription Rate of Other Concomitant Psychotropics: A Real-World Nationwide Study.Int J Neuropsychopharmacol. 2022 Oct 25;25(10):818-826. doi: 10.1093/ijnp/pyac036. Int J Neuropsychopharmacol. 2022. PMID: 35723038 Free PMC article.
-
Implementing and Evaluating a National Integrated Digital Registry and Clinical Decision Support System in Early Intervention in Psychosis Services (Early Psychosis Informatics Into Care): Co-Designed Protocol.JMIR Res Protoc. 2024 Mar 19;13:e50177. doi: 10.2196/50177. JMIR Res Protoc. 2024. PMID: 38502175 Free PMC article.
-
What are the barriers and facilitators of clozapine use in early psychosis? A survey of UK early intervention clinicians.Schizophrenia (Heidelb). 2023 Apr 28;9(1):26. doi: 10.1038/s41537-023-00353-0. Schizophrenia (Heidelb). 2023. PMID: 37117237 Free PMC article.
-
Neuropsychological differences between treatment-resistant and treatment-responsive schizophrenia: a meta-analysis.Psychol Med. 2022 Jan;52(1):1-13. doi: 10.1017/S0033291721004128. Epub 2021 Nov 1. Psychol Med. 2022. PMID: 36415088 Free PMC article.
References
-
- Lally J, Ajnakina O, Stubbs B, Cullinane M, Murphy KC, Gaughran F, et al. Remission and recovery from first-episode psychosis in adults: systematic review and meta-analysis of long-term outcome studies. Br J Psychiatry 2017; 211: 350–8. - PubMed
-
- Zipursky RB, Menezes NM, Streiner DL. Risk of symptom recurrence with medication discontinuation in first-episode psychosis: a systematic review. Schizophr Res 2014; 152: 408–14. - PubMed
-
- Alvarez-Jimenez M, O'Donoghue B, Thompson A, Gleeson JF, Bendall S, Gonzalez-Blanch C, et al. Beyond clinical remission in first episode psychosis: thoughts on antipsychotic maintenance vs. guided discontinuation in the functional recovery era. CNS Drugs 2016; 30: 357–68. - PubMed
LinkOut - more resources
Full Text Sources
Miscellaneous