Relationships between hyperinsulinaemia, magnesium, vitamin D, thrombosis and COVID-19: rationale for clinical management
- PMID: 32938758
- PMCID: PMC7496570
- DOI: 10.1136/openhrt-2020-001356
Relationships between hyperinsulinaemia, magnesium, vitamin D, thrombosis and COVID-19: rationale for clinical management
Abstract
Risk factors for COVID-19 patients with poorer outcomes include pre-existing conditions: obesity, type 2 diabetes mellitus, cardiovascular disease (CVD), heart failure, hypertension, low oxygen saturation capacity, cancer, elevated: ferritin, C reactive protein (CRP) and D-dimer. A common denominator, hyperinsulinaemia, provides a plausible mechanism of action, underlying CVD, hypertension and strokes, all conditions typified with thrombi. The underlying science provides a theoretical management algorithm for the frontline practitioners.Vitamin D activation requires magnesium. Hyperinsulinaemia promotes: magnesium depletion via increased renal excretion, reduced intracellular levels, lowers vitamin D status via sequestration into adipocytes and hydroxylation activation inhibition. Hyperinsulinaemia mediates thrombi development via: fibrinolysis inhibition, anticoagulation production dysregulation, increasing reactive oxygen species, decreased antioxidant capacity via nicotinamide adenine dinucleotide depletion, haem oxidation and catabolism, producing carbon monoxide, increasing deep vein thrombosis risk and pulmonary emboli. Increased haem-synthesis demand upregulates carbon dioxide production, decreasing oxygen saturation capacity. Hyperinsulinaemia decreases cholesterol sulfurylation to cholesterol sulfate, as low vitamin D regulation due to magnesium depletion and/or vitamin D sequestration and/or diminished activation capacity decreases sulfotransferase enzyme SULT2B1b activity, consequently decreasing plasma membrane negative charge between red blood cells, platelets and endothelial cells, thus increasing agglutination and thrombosis.Patients with COVID-19 admitted with hyperglycaemia and/or hyperinsulinaemia should be placed on a restricted refined carbohydrate diet, with limited use of intravenous dextrose solutions. Degree/level of restriction is determined by serial testing of blood glucose, insulin and ketones. Supplemental magnesium, vitamin D and zinc should be administered. By implementing refined carbohydrate restriction, three primary risk factors, hyperinsulinaemia, hyperglycaemia and hypertension, that increase inflammation, coagulation and thrombosis risk are rapidly managed.
Keywords: cytokines; deep vein thrombosis; inflammation; oxidative stress; venous thromboembol.
© Author(s) (or their employer(s)) 2020. Re-use permitted under CC BY-NC. No commercial re-use. See rights and permissions. Published by BMJ.
Conflict of interest statement
Competing interests: JJD is Director of Scientific Affairs at Analyze. Invest. Develop. Partner.
Figures
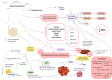

References
-
- Malhotra A, Kamepalli RK, Bamrah JS. Perspective: poor metabolic health is a major issue for increased COVID-19 mortality in BamE groups. The Physician 2020;6:1–4. 10.38192/1.6.2.4 - DOI
-
- Crofts CAP. Hyperinsulinemia: a unifying theory of chronic disease? Diabesity 2015;1:34 10.15562/diabesity.2015.19 - DOI
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical
Research Materials
Miscellaneous
