Total shoulder arthroplasty outcomes after noncorrective, concentric reaming of B2 glenoids
- PMID: 32939500
- PMCID: PMC7479043
- DOI: 10.1016/j.jseint.2020.04.006
Total shoulder arthroplasty outcomes after noncorrective, concentric reaming of B2 glenoids
Abstract
Background: Total shoulder arthroplasty (TSA) is an effective procedure for the treatment of glenohumeral osteoarthritis (GHOA) delivering reliable pain relief and improved shoulder function. Abnormal glenoid morphologies are common, and biconcave glenoids are enigmas that have been associated with poor clinical outcomes and implant survivorship.
Purpose: To assess the clinical outcome scores of patients who underwent noncorrective, concentric reaming for TSA with biconcave glenoids (B2). We hypothesized that patients with B2 glenoids who underwent TSA with glenoid implantation using noncorrective, concentric reaming would have significant improvements in clinical outcome scores and high implant survivorship.
Methods: All patients who underwent anatomic TSA for GHOA with B2 glenoids, performed by a single surgeon, between July 2006 and December 2015 with minimum 2-year follow-up were reviewed. Walch classification was obtained from preoperative imaging (magnetic resonance imaging or computed tomography). Clinical outcome scores were prospectively collected and included American Shoulder and Elbow Surgeons Standardized Shoulder Assessment Form (ASES) score, Single Assessment Numerical Evaluation (SANE) score, Quick Disabilities of the Arm, Shoulder, and Hand (QuickDASH) score, 12-Item Short Form Health Survey physical component summary (PCS), and patient satisfaction. Clinical failures (revision TSA surgery or conversion to reverse TSA) and complications were reported. Paired t test and bivariate correlations level of significance was set at P = .05. Survivorship analysis with implant failure as an endpoint was done using Kaplan-Meier survival curves.
Results: 51 TSA in 49 patients (9 females, 40 males) with primary GHOA with B2 glenoids were performed with a mean age of 64 (range 36-81 years) at the time of surgery. The mean retroversion was 19.1° (range 5.4°-38°), and posterior decentering was 42.0% (range 19.4%-78.5%). At final evaluation, 45/51 anatomic TSAs (88% follow-up) with a mean follow-up of 4.9 years (range 2.0-10.4 years) were assessed. All clinical outcome scores improved significantly pre- to postoperatively: ASES, 52.5 to 79.6 (P < .001); SANE, 52.4 to 74.7 (P < .001); QuickDASH, 39.2 to 19.1 (P = .001); and PCS, 40.9 to 48.9 (P = .001). Median postoperative satisfaction was 9 (range 1-10). There were 2 failures and 4 that required another surgery -subscapularis repair, lysis of adhesions, irrigation and débridement, and one to explore the status of the subscapularis for persistent pain. The implant survivorship rate was 95% at a mean follow-up of 4.9 years.
Conclusion: Anatomic total shoulder replacement with minimally noncorrective, concentric reaming in patients with B2 glenoids had significant improvement in clinical outcome scores, high patient satisfaction, and high survivorship in this cohort.
Keywords: Total shoulder arthroplasty; biconcave glenoids (B2) glenoids; outcomes; survivorship.
© 2020 The Author(s).
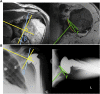
Figures



Similar articles
-
Anatomic total shoulder arthroplasty for B2 glenoids treated with asymmetric reaming has equivalent survivorship and patient outcomes compared with type A glenoids at a mean 9-year follow-up.J Shoulder Elbow Surg. 2024 Nov;33(11):2392-2399. doi: 10.1016/j.jse.2024.03.030. Epub 2024 Apr 28. J Shoulder Elbow Surg. 2024. PMID: 38688420
-
Outcomes of anatomic shoulder arthroplasty performed on B2 vs. A1 type glenoids.J Shoulder Elbow Surg. 2020 Dec;29(12):2571-2577. doi: 10.1016/j.jse.2020.03.050. Epub 2020 Jun 9. J Shoulder Elbow Surg. 2020. PMID: 33190757
-
Early to midterm outcomes of anatomic shoulder arthroplasty performed on dysplastic glenoids.J Shoulder Elbow Surg. 2021 Jul;30(7S):S77-S83. doi: 10.1016/j.jse.2020.08.017. Epub 2020 Sep 2. J Shoulder Elbow Surg. 2021. PMID: 32890678
-
Anatomic vs. reverse shoulder arthroplasty for the treatment of Walch B2 glenoid morphology: a systematic review and meta-analysis.JSES Rev Rep Tech. 2021 Sep 1;1(4):317-328. doi: 10.1016/j.xrrt.2021.08.003. eCollection 2021 Nov. JSES Rev Rep Tech. 2021. PMID: 37588714 Free PMC article. Review.
-
Total Shoulder Arthroplasty Versus Reverse Shoulder Arthroplasty in Primary Glenohumeral Osteoarthritis With Intact Rotator Cuffs: A Meta-Analyses.Cureus. 2024 Apr 8;16(4):e57866. doi: 10.7759/cureus.57866. eCollection 2024 Apr. Cureus. 2024. PMID: 38725735 Free PMC article. Review.
Cited by
-
Early outcomes of augmented glenoid components in anatomic total shoulder arthroplasty: a systematic review.Shoulder Elbow. 2022 Jun;14(3):238-248. doi: 10.1177/17585732211032922. Epub 2021 Aug 18. Shoulder Elbow. 2022. PMID: 35599710 Free PMC article.
-
Evaluating the incidence and associated factors of subscapularis failure following anatomical total shoulder arthroplasty: a systematic review.Eur J Orthop Surg Traumatol. 2025 Jun 19;35(1):258. doi: 10.1007/s00590-025-04388-0. Eur J Orthop Surg Traumatol. 2025. PMID: 40536679
-
Outcomes of anatomic versus reverse shoulder arthroplasty for B2 & B3 glenoids with an intact rotator cuff: An updated systematic review and proportional meta-analysis.Shoulder Elbow. 2025 Jul 17:17585732251359590. doi: 10.1177/17585732251359590. Online ahead of print. Shoulder Elbow. 2025. PMID: 40689354 Free PMC article.
References
-
- Friedman R.J., Hawthorne K.B., Genez B.M. The use of computerized tomography in the measurement of glenoid version. J Bone Joint Surg Am. 1992;74:1032–1037. - PubMed
LinkOut - more resources
Full Text Sources
Research Materials
