Perioperative fluid balance and 30-day unplanned readmission after lung cancer surgery: a retrospective study
- PMID: 32944306
- PMCID: PMC7475599
- DOI: 10.21037/jtd-20-1474
Perioperative fluid balance and 30-day unplanned readmission after lung cancer surgery: a retrospective study
Abstract
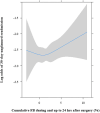
Background: Perioperative positive fluid balance (FB) is associated with increased complications after lung resection surgery. However, its impact on the 30-day unplanned readmission rate is unclear. This study aimed to determine whether perioperative FB status during and up to 24 hours after lung resection surgery is associated with the 30-day unplanned readmission rate.
Methods: This retrospective cohort study examined adult patients aged 19 years or older who underwent lung cancer surgery at a single tertiary academic hospital between January 2005 and February 2018. Weight-based cumulative FB (%) was calculated during and up to 24 hours after surgery and was categorized as positive (≥5%), normal (0-5%), or negative (<0%). Univariable and multivariable logistic regression analyses were performed.
Results: The final analysis included 2,412 patients; 164 patients had unplanned readmission during the first 30 postoperative days (6.9%; 164/2,412). According to the multivariable logistic regression model, the positive FB group had a 2.42-time higher risk of 30-day unplanned readmission compared to the normal FB group [odds ratio (OR): 2.42; 95% confidence interval (CI): 1.20 to 4.89; P=0.014]. However, the risk of the negative FB group did not significantly differ from that of the normal FB group (OR: 1.20; 95% CI: 0.46 to 3.12; P=0.711).
Conclusions: Perioperative positive FB (>5%) during and up to 24 hours after surgery was associated with an increased 30-day unplanned readmission rate after lung cancer surgery. Future prospective studies are needed to confirm these findings.
Keywords: Hospitalization; lung neoplasms; thoracic surgery.
2020 Journal of Thoracic Disease. All rights reserved.
Conflict of interest statement
Conflicts of Interest: All authors have completed the ICMJE uniform disclosure form (available at http://dx.doi.org/10.21037/jtd-20-1474). The authors have no conflicts of interest to declare.
Figures


Similar articles
-
Association Between Perioperative Fluid Balance and 30-Day Unplanned Readmission After Major Abdominal Surgery.Surg Innov. 2019 Aug;26(4):401-407. doi: 10.1177/1553350619836856. Epub 2019 Mar 28. Surg Innov. 2019. PMID: 30920902
-
Factors associated with a 30-day unplanned readmission after elective spine surgery: a retrospective cohort study.Eur Spine J. 2021 Jan;30(1):191-199. doi: 10.1007/s00586-020-06541-1. Epub 2020 Aug 4. Eur Spine J. 2021. PMID: 32754776
-
Perioperative Risk Factors Associated With Postoperative Unplanned Intubation After Lung Resection.J Cardiothorac Vasc Anesth. 2018 Aug;32(4):1739-1746. doi: 10.1053/j.jvca.2018.01.032. Epub 2018 Jan 31. J Cardiothorac Vasc Anesth. 2018. PMID: 29506893
-
Association of Clinical Risk Factors and Postoperative Complications With Unplanned Hospital Readmission After Head and Neck Cancer Surgery.JAMA Otolaryngol Head Neck Surg. 2016 Dec 1;142(12):1184-1190. doi: 10.1001/jamaoto.2016.2807. JAMA Otolaryngol Head Neck Surg. 2016. PMID: 27737442
-
Predictors of unplanned 30-day readmissions after coronary artery bypass graft: a systematic review and meta-analysis of cohort studies.Eur J Cardiovasc Nurs. 2021 Oct 27;20(7):717-725. doi: 10.1093/eurjcn/zvab023. Eur J Cardiovasc Nurs. 2021. PMID: 33864067
Cited by
-
Restricted, optimized or liberal fluid strategy in thoracic surgery: A narrative review.Saudi J Anaesth. 2021 Jul-Sep;15(3):324-334. doi: 10.4103/sja.sja_1155_20. Epub 2021 Jun 19. Saudi J Anaesth. 2021. PMID: 34764839 Free PMC article. Review.
References
LinkOut - more resources
Full Text Sources
