Mitochondrial Dysfunction in Obesity and Reproduction
- PMID: 32945868
- PMCID: PMC7709214
- DOI: 10.1210/endocr/bqaa158
Mitochondrial Dysfunction in Obesity and Reproduction
Abstract
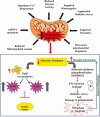
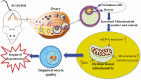
Mounting evidence suggests a role for mitochondrial dysfunction in the pathogenesis of many diseases, including type 2 diabetes, aging, and ovarian failure. Because of the central role of mitochondria in energy production, heme biosynthesis, calcium buffering, steroidogenesis, and apoptosis signaling within cells, understanding the molecular mechanisms behind mitochondrial dysregulation and its potential implications in disease is critical. This review will take a journey through the past and summarize what is known about mitochondrial dysfunction in various disorders, focusing on metabolic alterations and reproductive abnormalities. Evidence is presented from studies in different human populations, and rodents with genetic manipulations of pathways known to affect mitochondrial function.
Keywords: insulin resistance; lipid accumulation; mitochondrial dynamics; mitochondrial function; mitophagy; ovarian dysfunction; oxidative stress.
Published by Oxford University Press on behalf of the Endocrine Society 2020.
Figures
References
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

