Correlation of T2* relaxation times of the retropatellar cartilage with tibial tuberosity-trochlea groove distance in professional soccer players
- PMID: 32948810
- PMCID: PMC7501245
- DOI: 10.1038/s41598-020-72299-7
Correlation of T2* relaxation times of the retropatellar cartilage with tibial tuberosity-trochlea groove distance in professional soccer players
Abstract
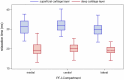
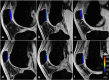
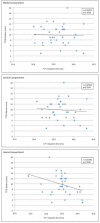
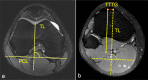
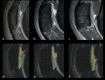
The tibial tuberosity-trochlear groove (TT-TG) distance is a radiographic measurement that is used to quantify malalignment of the patellofemoral joint (PFJ) in cross-sectional imaging. There is an ongoing debate about the impact of the TT-TG-distance on lateral patellar instability and the initiating of cartilage degeneration. In this prospective study, the association of T2* relaxation times and TT-TG distances in professional soccer players was analyzed. 36 knees of 18 professional soccer players (age: 21 ± 2.8 years) were evaluated. Participants underwent knee MRI at 3 T. For qualitative image analysis, fat-saturated 2D PD-weighted Fast Spin Echo (FSE) and T1-weighted FSE sequences were used. For quantitative analysis, T2* measurements in 3D data acquisitions were performed. In a qualitative analysis there was no structural cartilage damage and no abnormalities of the patellar and trochlea shape. The highest T2* values (26.7 ± 5.9 ms) were observed in the central compartment of the patella. The mean TT-TG distance was 10 ± 4 mm (range 3-20 mm). There was no significant correlation between TT-TG distance and T2* relaxation times in all three compartments of the retropatellar cartilage. Our study shows that so long as patellar and trochlear morphology is normal, TT-TG distance alone does not affect the tissue structure of the retropatellar cartilage in professional soccer players.
Conflict of interest statement
The authors declare no competing interests.
Figures
References
-
- Laurin CA, Levesque HP, Dussault R, Labelle H, Peides JP. The abnormal lateral patellofemoral angle: A diagnostic roentgenographic sign of recurrent patellar subluxation. J. Bone Joint Surg. Am. 1978;60:55–60. - PubMed
-
- Smith TO, Donell ST, Chester R, Clark A, Stephenson R. What activities do patients with patellar instability perceive makes their patella unstable? Knee. 2011;18:333–339. - PubMed
-
- Diederichs G, Issever AS, Scheffler S. MR imaging of patellar instability: Injury patterns and assessment of risk factors. Radiographics. 2010;30:961–981. - PubMed
-
- Fithian DC, Paxton EW, Stone ML, Silva P, Davis DK, Elias DA, et al. Epidemiology and natural history of acute patellar dislocation. Am. J. Sports Med. 2004;32:1114–1121. - PubMed
-
- Chan VO, Moran DE, Mwangi I, Eustace SJ. Prevalence and clinical significance of chondromalacia isolated to the anterior margin of the lateral femoral condyle as a component of patellofemoral disease: Observations at MR imaging. Skeletal. Radiol. 2013;42:1127–1133. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

