Shift work influences the outcomes of Chlamydia infection and pathogenesis
- PMID: 32958779
- PMCID: PMC7505842
- DOI: 10.1038/s41598-020-72409-5
Shift work influences the outcomes of Chlamydia infection and pathogenesis
Erratum in
-
Author Correction: Shift work influences the outcomes of Chlamydia infection and pathogenesis.Sci Rep. 2020 Dec 11;10(1):22183. doi: 10.1038/s41598-020-79099-z. Sci Rep. 2020. PMID: 33311582 Free PMC article. No abstract available.
Abstract
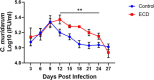
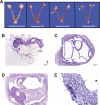
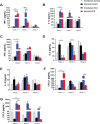
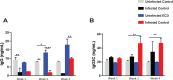
Shift work, performed by approximately 21 million Americans, is irregular or unusual work schedule hours occurring after 6:00 pm. Shift work has been shown to disrupt circadian rhythms and is associated with several adverse health outcomes and chronic diseases such as cancer, gastrointestinal and psychiatric diseases and disorders. It is unclear if shift work influences the complications associated with certain infectious agents, such as pelvic inflammatory disease, ectopic pregnancy and tubal factor infertility resulting from genital chlamydial infection. We used an Environmental circadian disruption (ECD) model mimicking circadian disruption occurring during shift work, where mice had a 6-h advance in the normal light/dark cycle (LD) every week for a month. Control group mice were housed under normal 12/12 LD cycle. Our hypothesis was that compared to controls, mice that had their circadian rhythms disrupted in this ECD model will have a higher Chlamydia load, more pathology and decreased fertility rate following Chlamydia infection. Results showed that, compared to controls, mice that had their circadian rhythms disrupted (ECD) had higher Chlamydia loads, more tissue alterations or lesions, and lower fertility rate associated with chlamydial infection. Also, infected ECD mice elicited higher proinflammatory cytokines compared to mice under normal 12/12 LD cycle. These results imply that there might be an association between shift work and the increased likelihood of developing more severe disease from Chlamydia infection.
Conflict of interest statement
The authors declare no competing interests.
Figures


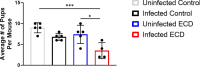
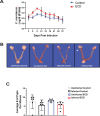
References
Publication types
MeSH terms
Grants and funding
- 1SC1GM109861/GM/NIGMS NIH HHS/United States
- U54 MD007588/MD/NIMHD NIH HHS/United States
- R35 GM127044/GM/NIGMS NIH HHS/United States
- SC1 GM112567/GM/NIGMS NIH HHS/United States
- UL1 TR002378/TR/NCATS NIH HHS/United States
- 5R01AI126897/AI/NIAID NIH HHS/United States
- R35 GM136661/GM/NIGMS NIH HHS/United States
- 1SC2HD086066-01A1/HD/NICHD NIH HHS/United States
- R01 AI126897/AI/NIAID NIH HHS/United States
- G12 MD007602/MD/NIMHD NIH HHS/United States
- R25 MD007589/MD/NIMHD NIH HHS/United States
- 1SC1AII03041-01A1/GM/NIGMS NIH HHS/United States
- 1R35GM13666101/GM/NIGMS NIH HHS/United States
- T32 HL103104/HL/NHLBI NIH HHS/United States
- SC2 HD086066/HD/NICHD NIH HHS/United States
LinkOut - more resources
Full Text Sources
Medical
Research Materials

