Association of Mortality and Years of Potential Life Lost With Active Tuberculosis in the United States
- PMID: 32965497
- PMCID: PMC7512053
- DOI: 10.1001/jamanetworkopen.2020.14481
Association of Mortality and Years of Potential Life Lost With Active Tuberculosis in the United States
Abstract
Importance: Active tuberculosis (TB) disease leads to substantial mortality but is preventable through screening and treatment for latent TB infection. Early mortality after TB diagnosis (≤1 year) is well described, but delayed mortality (>1 year) among patients with active TB is poorly understood.
Objective: To compare early and delayed mortality and years of potential life (YPL) lost among patients with active TB disease vs an age-, sex-, and year of diagnosis-matched comparison cohort without active TB disease.
Design, setting, and participants: This retrospective cohort study, conducted in the integrated health system of Kaiser Permanente Northern California, included patients with microbiologically confirmed active TB disease from January 1, 1997, to December 31, 2017, and a control cohort matched by age, sex, and year of diagnosis. Multivariable models were used to adjust for demographic and clinical characteristics. Patients with active TB disease prior to 1997 were excluded. Data were analyzed from January 1, 2019, to January 31, 2020.
Exposure: Microbiologically confirmed TB disease.
Main outcomes and measures: Early (≤1 year after TB diagnosis) and delayed (>1 year after TB diagnosis) all-cause mortality.
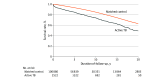
Results: A total of 2522 patients who had active TB from 1997 to 2017 were identified, with 17 166 person-years of follow-up. The comparison cohort included 100 880 persons with 735 726 person-years of follow-up. In the active TB and comparison cohorts, similar percentages of persons were male (56.3% vs 55.6%), aged 45 to 64 years (33.7% vs 33.7%), and aged 65 years or older (24.7% vs 24.7%). Both early mortality (7.0%) and delayed mortality (16.3%) were higher among patients with active TB disease compared with those without active TB disease (1.1% and 12.0%, respectively). Patients with active TB disease had a significantly higher risk for early (adjusted hazard ratio [aHR], 7.29; 95% CI, 6.08-8.73) and delayed (aHR, 1.78; 95% CI, 1.61-1.98) mortality compared with the comparison cohort (P < .001). Active TB disease was associated with an adjusted -7.0 (95% CI, -8.4 to -5.5) YPL lost compared with the comparison cohort.
Conclusions and relevance: In this study, patients with active TB disease had significantly higher early and delayed all-cause mortality when adjusting for demographic and clinical characteristics. These findings suggest that TB prevention through screening and treatment of latent TB infection could reduce mortality and YPL lost due to active TB disease.
Conflict of interest statement
Figures
Similar articles
-
Sociodemographic Characteristics, Comorbidities, and Mortality Among Persons Diagnosed With Tuberculosis and COVID-19 in Close Succession in California, 2020.JAMA Netw Open. 2021 Dec 1;4(12):e2136853. doi: 10.1001/jamanetworkopen.2021.36853. JAMA Netw Open. 2021. PMID: 34860244 Free PMC article.
-
Estimated Impact of World Health Organization Latent Tuberculosis Screening Guidelines in a Region With a Low Tuberculosis Incidence: Retrospective Cohort Study.Clin Infect Dis. 2019 Nov 27;69(12):2101-2108. doi: 10.1093/cid/ciz188. Clin Infect Dis. 2019. PMID: 30856258 Free PMC article.
-
Incidence of active tuberculosis in individuals with latent tuberculosis infection in rural China: follow-up results of a population-based, multicentre, prospective cohort study.Lancet Infect Dis. 2017 Oct;17(10):1053-1061. doi: 10.1016/S1473-3099(17)30402-4. Epub 2017 Jul 14. Lancet Infect Dis. 2017. PMID: 28716677
-
Latent Tuberculosis Infection Testing Strategies for HIV-Positive Individuals in Hong Kong.JAMA Netw Open. 2019 Sep 4;2(9):e1910960. doi: 10.1001/jamanetworkopen.2019.10960. JAMA Netw Open. 2019. PMID: 31490541 Free PMC article.
-
[Children exposed to multidrug-resistant tuberculosis: How should we manage? Analysis of 46 child contacts and review of the literature].Rev Pneumol Clin. 2015 Dec;71(6):335-41. doi: 10.1016/j.pneumo.2015.05.003. Epub 2015 Jul 17. Rev Pneumol Clin. 2015. PMID: 26195117 Review. French.
Cited by
-
Increased DNA methylation, cellular senescence and premature epigenetic aging in guinea pigs and humans with tuberculosis.Aging (Albany NY). 2022 Mar 7;14(5):2174-2193. doi: 10.18632/aging.203936. Epub 2022 Mar 7. Aging (Albany NY). 2022. PMID: 35256539 Free PMC article.
-
Contribution of Posttuberculosis Sequelae to Life-Years Lost from Tuberculosis Disease in the United States, 2015-2019.Am J Respir Crit Care Med. 2025 Jun;211(6):1059-1068. doi: 10.1164/rccm.202411-2213OC. Am J Respir Crit Care Med. 2025. PMID: 39928299 Free PMC article.
-
Mortality Rates after Tuberculosis Treatment, Georgia, USA, 2008-2019.Emerg Infect Dis. 2024 Nov;30(11):2261-2270. doi: 10.3201/eid3011.240329. Emerg Infect Dis. 2024. PMID: 39447141 Free PMC article. Review.
-
Reversing Post-Infectious Epigenetic-Mediated Immune Suppression.Front Immunol. 2021 Jun 7;12:688132. doi: 10.3389/fimmu.2021.688132. eCollection 2021. Front Immunol. 2021. PMID: 34163486 Free PMC article. Review.
-
Lifetime burden of disease due to incident tuberculosis: a global reappraisal including post-tuberculosis sequelae.Lancet Glob Health. 2021 Dec;9(12):e1679-e1687. doi: 10.1016/S2214-109X(21)00367-3. Lancet Glob Health. 2021. PMID: 34798027 Free PMC article.
References
-
- Centers for Disease Control and Prevention Reported Tuberculosis in the United States, 2017. Updated October 22, 2018. Accessed September 10, 2019. https://www.cdc.gov/tb/statistics/reports/2017/default.htm
-
- Tuberculosis Control Branch. Report on tuberculosis in California, 2018. Published July 2019. Accessed September 10, 2019. https://www.cdph.ca.gov/Programs/CID/DCDC/CDPH%20Document%20Library/TBCB...
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical