Myh11+ microvascular mural cells and derived mesenchymal stem cells promote retinal fibrosis
- PMID: 32978500
- PMCID: PMC7519078
- DOI: 10.1038/s41598-020-72875-x
Myh11+ microvascular mural cells and derived mesenchymal stem cells promote retinal fibrosis
Abstract
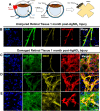
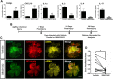
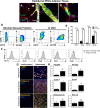
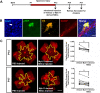
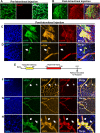
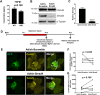
Retinal diseases are frequently characterized by the accumulation of excessive scar tissue found throughout the neural retina. However, the pathophysiology of retinal fibrosis remains poorly understood, and the cell types that contribute to the fibrotic response are incompletely defined. Here, we show that myofibroblast differentiation of mural cells contributes directly to retinal fibrosis. Using lineage tracing technology, we demonstrate that after chemical ocular injury, Myh11+ mural cells detach from the retinal microvasculature and differentiate into myofibroblasts to form an epiretinal membrane. Inhibition of TGFβR attenuates Myh11+ retinal mural cell myofibroblast differentiation, and diminishes the subsequent formation of scar tissue on the surface of the retina. We demonstrate retinal fibrosis within a murine model of oxygen-induced retinopathy resulting from the intravitreal injection of adipose Myh11-derived mesenchymal stem cells, with ensuing myofibroblast differentiation. In this model, inhibiting TGFβR signaling does not significantly alter myofibroblast differentiation and collagen secretion within the retina. This work shows the complexity of retinal fibrosis, where scar formation is regulated both by TGFβR and non-TGFβR dependent processes involving mural cells and derived mesenchymal stem cells. It also offers a cautionary note on the potential deleterious, pro-fibrotic effects of exogenous MSCs once intravitreally injected into clinical patients.
Conflict of interest statement
P.A.Y. is the founder of RetiVue, LLC, a company that develops innovative, affordable, and convenient retinal screening technologies for patients. P.A.Y. is also a consultant of Genentech/Roche. All other authors declare no competing interests.
Figures
Similar articles
-
Umbilical Cord-Derived Mesenchymal Stem Cell-Derived Exosomal MicroRNAs Suppress Myofibroblast Differentiation by Inhibiting the Transforming Growth Factor-β/SMAD2 Pathway During Wound Healing.Stem Cells Transl Med. 2016 Oct;5(10):1425-1439. doi: 10.5966/sctm.2015-0367. Epub 2016 Jul 7. Stem Cells Transl Med. 2016. PMID: 27388239 Free PMC article.
-
Cardiac mesenchymal stem cells contribute to scar formation after myocardial infarction.Cardiovasc Res. 2011 Jul 1;91(1):99-107. doi: 10.1093/cvr/cvr061. Epub 2011 Feb 28. Cardiovasc Res. 2011. PMID: 21357194 Free PMC article.
-
Lysophosphatidic acid accelerates lung fibrosis by inducing differentiation of mesenchymal stem cells into myofibroblasts.J Cell Mol Med. 2014 Jan;18(1):156-69. doi: 10.1111/jcmm.12178. Epub 2013 Nov 19. J Cell Mol Med. 2014. PMID: 24251962 Free PMC article.
-
Understanding the origin, activation and regulation of matrix-producing myofibroblasts for treatment of fibrotic disease.J Pathol. 2013 Nov;231(3):273-89. doi: 10.1002/path.4253. J Pathol. 2013. PMID: 24006178 Review.
-
METTL3-mediated m6A RNA methylation induces the differentiation of lung resident mesenchymal stem cells into myofibroblasts via the miR-21/PTEN pathway.Respir Res. 2023 Nov 28;24(1):300. doi: 10.1186/s12931-023-02606-z. Respir Res. 2023. PMID: 38017523 Free PMC article. Review.
Cited by
-
A Long-Term Safety and Efficacy Report on Intravitreal Delivery of Adipose Stem Cells and Secretome on Visual Deficits After Traumatic Brain Injury.Transl Vis Sci Technol. 2022 Oct 3;11(10):1. doi: 10.1167/tvst.11.10.1. Transl Vis Sci Technol. 2022. PMID: 36180031 Free PMC article.
-
Protein Tyrosine Phosphatase 1B Deficiency in Vascular Smooth Muscle Cells Promotes Perivascular Fibrosis following Arterial Injury.Thromb Haemost. 2022 Oct;122(10):1814-1826. doi: 10.1055/s-0042-1755329. Epub 2022 Sep 8. Thromb Haemost. 2022. PMID: 36075234 Free PMC article.
-
Extracellular matrix remodelling in dental pulp tissue of carious human teeth through the prism of single-cell RNA sequencing.Int J Oral Sci. 2023 Aug 2;15(1):30. doi: 10.1038/s41368-023-00238-z. Int J Oral Sci. 2023. PMID: 37532703 Free PMC article.
-
Single-Cell RNA Sequencing of Rabbit Sclera at Different Developmental Stages: Unveiling Scleral Cells Atlas and the Heterogeneity of Fibroblasts.Invest Ophthalmol Vis Sci. 2025 Jun 2;66(6):83. doi: 10.1167/iovs.66.6.83. Invest Ophthalmol Vis Sci. 2025. PMID: 40576432 Free PMC article.
-
Brain Microvascular Pericyte Pathology Linking Alzheimer's Disease to Diabetes.Microcirculation. 2024 Oct;31(7):e12877. doi: 10.1111/micc.12877. Epub 2024 Sep 2. Microcirculation. 2024. PMID: 39222475 Review.
References
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Molecular Biology Databases

