Innate immunity during SARS-CoV-2: evasion strategies and activation trigger hypoxia and vascular damage
- PMID: 32978971
- PMCID: PMC7537271
- DOI: 10.1111/cei.13523
Innate immunity during SARS-CoV-2: evasion strategies and activation trigger hypoxia and vascular damage
Abstract
Innate immune sensing of viral molecular patterns is essential for development of antiviral responses. Like many viruses, SARS-CoV-2 has evolved strategies to circumvent innate immune detection, including low cytosine-phosphate-guanosine (CpG) levels in the genome, glycosylation to shield essential elements including the receptor-binding domain, RNA shielding and generation of viral proteins that actively impede anti-viral interferon responses. Together these strategies allow widespread infection and increased viral load. Despite the efforts of immune subversion, SARS-CoV-2 infection activates innate immune pathways inducing a robust type I/III interferon response, production of proinflammatory cytokines and recruitment of neutrophils and myeloid cells. This may induce hyperinflammation or, alternatively, effectively recruit adaptive immune responses that help clear the infection and prevent reinfection. The dysregulation of the renin-angiotensin system due to down-regulation of angiotensin-converting enzyme 2, the receptor for SARS-CoV-2, together with the activation of type I/III interferon response, and inflammasome response converge to promote free radical production and oxidative stress. This exacerbates tissue damage in the respiratory system, but also leads to widespread activation of coagulation pathways leading to thrombosis. Here, we review the current knowledge of the role of the innate immune response following SARS-CoV-2 infection, much of which is based on the knowledge from SARS-CoV and other coronaviruses. Understanding how the virus subverts the initial immune response and how an aberrant innate immune response contributes to the respiratory and vascular damage in COVID-19 may help to explain factors that contribute to the variety of clinical manifestations and outcome of SARS-CoV-2 infection.
Keywords: COVID-19; SARS-CoV-2; endothelia; immunology; inflammation.
© 2020 The Authors. Clinical & Experimental Immunology published by John Wiley & Sons Ltd on behalf of British Society for Immunology.
Conflict of interest statement
D. B. and S. A. have received compensation for consultancies, presentations and advisory board activities, but no companies were involved in the decision to write and submit this manuscript. L. F. B. has nothing to disclose. S. A. has received consultancy from Novartis and Roche. D. B. has received compensation for activities related to Canbex therapeutics, InMune Biol, Lundbeck, Japan Tobacco, Merck and Novartis.
Figures


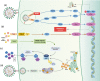

References
-
- Collins AR. HLA class I antigen serves as a receptor for human coronavirus OC43. Immunol Invest 1993; 22:95–103. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

