SPONTANEOUS RESOLUTION OF PRIMARY HYPERCORTISOLISM OF CUSHING DISEASE AFTER PITUITARY HEMORRHAGE
- PMID: 32984518
- PMCID: PMC7279773
- DOI: 10.4158/ACCR-2019-0292
SPONTANEOUS RESOLUTION OF PRIMARY HYPERCORTISOLISM OF CUSHING DISEASE AFTER PITUITARY HEMORRHAGE
Abstract
Objective: To describe a case of spontaneous resolution of primary hypercortisolism from Cushing disease (CD) due to pituitary apoplexy (PA).
Methods: Clinical, laboratory, and pathologic information are described.
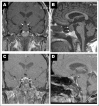
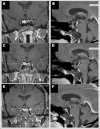
Results: A 59-year-old female presented with a headache, a 2.3 cm sellar mass with a questionable hemorrhagic component, and clinical signs of hypercortisolism. On further evaluation, she had an increased 24-hour urine free cortisol, abnormal serum cortisol during a low dose dexamethasone suppression test, and an elevated plasma adrenocorticotropic hormone (ACTH), consistent with pituitary CD. As she was being prepared for surgical resection, she was noted to have spontaneous biochemical remission associated with resolution of her symptoms of hypercortisolism, and a repeat magnetic resonance imaging scan showed shrinkage of the sellar mass. She has been managed conservatively since and remains in clinical/biochemical remission until present time, 18 months following her initial presentation.
Conclusion: We report a case of spontaneous resolution of CD from symptomatic hemorrhage within an ACTH-secreting pituitary adenoma, or PA. This has been rarely reported in the medical literature. The fact that she did not pass through a phase of adrenal withdrawal, makes us suspect a residual functional adenoma within or around the sella which may eventually grow, causing her disease to recur, as has been reported. Hence, continued monitoring will be required.
Copyright © 2020 AACE.
Conflict of interest statement
DISCLOSURE The authors have no multiplicity of interest to disclose.
Figures
Similar articles
-
Spontaneous Cushing's Disease Remission Induced by Pituitary Apoplexy.Cureus. 2024 Jul 10;16(7):e64231. doi: 10.7759/cureus.64231. eCollection 2024 Jul. Cureus. 2024. PMID: 39130944 Free PMC article.
-
Spontaneous remission of hypercortisolism presumed due to asymptomatic tumor apoplexy in ACTH-producing pituitary macroadenoma.Arq Bras Endocrinol Metabol. 2013 Aug;57(6):486-9. doi: 10.1590/s0004-27302013000600012. Arq Bras Endocrinol Metabol. 2013. PMID: 24030190
-
ACTH adenomas transforming their clinical expression: report of 5 cases.Neurosurg Focus. 2015 Feb;38(2):E15. doi: 10.3171/2014.11.FOCUS14679. Neurosurg Focus. 2015. PMID: 25639317
-
Endoscopic Endonasal Surgery for Remission of Cushing Disease Caused by Ectopic Intracavernous Macroadenoma: Case Report and Literature Review.World Neurosurg. 2017 Feb;98:870.e5-870.e10. doi: 10.1016/j.wneu.2016.12.021. Epub 2016 Dec 18. World Neurosurg. 2017. PMID: 28003168 Review.
-
Classic and recent etiologies of Cushing's syndrome: diagnosis and therapy.Treat Endocrinol. 2002;1(2):79-94. doi: 10.2165/00024677-200201020-00002. Treat Endocrinol. 2002. PMID: 15765624 Review.
Cited by
-
Pituitary apoplexy in cushing's disease: a single center study and systematic literature review.Pituitary. 2024 Aug;27(4):335-344. doi: 10.1007/s11102-024-01411-1. Epub 2024 Jun 8. Pituitary. 2024. PMID: 38850401
-
Sparsely Granulated Corticotroph Pituitary Macroadenoma Presenting With Pituitary Apoplexy Resulting in Remission of Hypercortisolism.AACE Clin Case Rep. 2022 Apr 8;8(4):166-170. doi: 10.1016/j.aace.2022.04.003. eCollection 2022 Jul-Aug. AACE Clin Case Rep. 2022. PMID: 35959088 Free PMC article.
-
Spontaneous Cushing's Disease Remission Induced by Pituitary Apoplexy.Cureus. 2024 Jul 10;16(7):e64231. doi: 10.7759/cureus.64231. eCollection 2024 Jul. Cureus. 2024. PMID: 39130944 Free PMC article.
-
Pituitary Apoplexy in Patients with Pituitary Neuroendocrine Tumors (PitNET).Biomedicines. 2023 Feb 23;11(3):680. doi: 10.3390/biomedicines11030680. Biomedicines. 2023. PMID: 36979658 Free PMC article. Review.
References
-
- Broder MS, Neary MP, Chang E, Cherepanov D, Ludlam WH. Incidence of Cushing's syndrome and Cushing's disease in commercially-insured patients <65 years old in the United States. Pituitary. 2015;18:283–289. - PubMed
-
- Pivonello R, De Martino MC, De Leo M, Simeoli C, Colao A. Cushing's disease: the burden of illness. Endocrine. 2017;56:10–18. - PubMed
-
- Hammer GD, Tyrrell JB, Lamborn KR et al. Transsphenoidal microsurgery for Cushing's disease: initial outcome and long-term results. J Clin Endocrinol Metab. 2004;89:6348–6357. - PubMed
-
- Onesti ST, Wisniewski T, Post KD. Clinical versus subclinical pituitary apoplexy: presentation, surgical management, and outcome in 21 patients. Neurosurgery. 1990;26:980–986. - PubMed
Publication types
LinkOut - more resources
Full Text Sources
Research Materials
