Discrete-Event Simulation Modeling of Critical Care Flow: New Hospital, Old Challenges
- PMID: 32984824
- PMCID: PMC7491890
- DOI: 10.1097/CCE.0000000000000174
Discrete-Event Simulation Modeling of Critical Care Flow: New Hospital, Old Challenges
Abstract
Objectives: As the demand for critical care beds rises each year, hospitals must be able to adapt. Delayed transfer of care reduces available critical care capacity and increases occupancy. The use of mathematic modeling within healthcare systems has the ability to aid planning of resources. Discrete-event simulation models can determine the optimal number of critical care beds required and simulate different what-if scenarios.
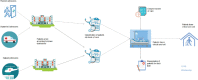
Design: Complex discrete-event simulation model was developed using a warm-up period of 30 days and ran for 30 trials against a 2-year period with the mean calculated for the runs. A variety of different scenarios were investigated to determine the effects of increasing capacity, increasing demand, and reduction of proportion and length of delayed transfer of care out of the ICU.
Setting: Combined data from two ICUs in United Kingdom.
Patients: The model was developed using 1,728 patient records and was validated against an independent dataset of 2,650 patients.
Interventions: None.
Measurements and main results: During model validation, the average bed utilization and admittance rate were equal to the real-world data. In the what-if scenarios, we found that increasing bed numbers from 23 to 28 keeping the arrival rate stable reduces the average occupancy rate to 70%. We found that the projected 4% yearly increase in admissions could overwhelm even the 28-bedded unit, without change in the delayed transfer of care episodes. Reduction in the proportion of patients experiencing delayed transfer of care had the biggest effect on occupancy rates, time spent at full capacity, and average bed utilization.
Conclusions: Using discrete-event simulation of commonly available baseline patient flow and patient care data produces reproducible models. Reducing the proportion of patients with delayed transfer of care had a greater effect in reducing occupancy levels than simply increasing bed numbers even when demand is increased.
Keywords: critical care; delayed transfer of care; discrete-event simulation; modeling.
Copyright © 2020 The Authors. Published by Wolters Kluwer Health, Inc. on behalf of the Society of Critical Care Medicine.
Conflict of interest statement
The authors have disclosed that they do not have any potential conflicts of interest.
Figures
References
-
- Jones A, Toft-Petersen AP, Shankar-Hari M, et al. Demographic shifts, case mix, activity, and outcome for elderly patients admitted to adult general ICUs in England, Wales, and Northern Ireland. Crit Care Med. 2020; 48:466–474 - PubMed
-
- Shahani AK, Ridley SA, Nielsen MS; Intensive Care Society’s and Department of Health’s Working Group on Patient Flows. Modelling patient flows as an aid to decision making for critical care capacities and organisation. Anaesthesia. 2008; 63:1074–1080 - PubMed
-
- Williams J, Dumont S, Parry-Jones J, et al. Mathematical modelling of patient flows to predict critical care capacity required following the merger of two district general hospitals into one. Anaesthesia. 2015; 70:32–40 - PubMed
LinkOut - more resources
Full Text Sources
Research Materials
Miscellaneous