Patients' and Nurses' Experiences and Perceptions of Remote Monitoring of Implantable Cardiac Defibrillators in Heart Failure: Cross-Sectional, Descriptive, Mixed Methods Study
- PMID: 32985997
- PMCID: PMC7551113
- DOI: 10.2196/19550
Patients' and Nurses' Experiences and Perceptions of Remote Monitoring of Implantable Cardiac Defibrillators in Heart Failure: Cross-Sectional, Descriptive, Mixed Methods Study
Abstract
Background: The new generation of implantable cardioverter-defibrillators (ICDs) supports wireless technology, which enables remote patient monitoring (RPM) of the device. In Sweden, it is mainly registered nurses with advanced education and training in ICD devices who handle the arrhythmias and technical issues of the remote transmissions. Previous studies have largely focused on the perceptions of physicians, and it has not been explored how the patients' and nurses' experiences of RPM correspond to each other.
Objective: Our objective is to describe, explore, and compare the experiences and perceptions, concerning RPM of ICD, of patients with heart failure (HF) and nurses performing ICD follow-up.
Methods: This study has a cross-sectional, descriptive, mixed methods design. All patients with HF and an ICD with RPM from one region in Sweden, who had transitioned from office-based visits to implementing RPM, and ICD nurses from all ICD clinics in Sweden were invited to complete a purpose-designed, 8-item questionnaire to assess experiences of RPM. The questionnaire started with a neutral question: "What are your experiences of RPM in general?" This was followed by one positive subscale with three questions (score range 3-12), with higher scores reflecting more positive experiences, and one negative subscale with three questions (score range 3-12), with lower scores reflecting more negative experiences. One open-ended question was analyzed with qualitative content analysis.
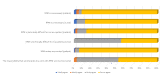
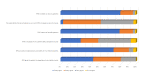
Results: The sample consisted of 175 patients (response rate 98.9%) and 30 ICD nurses (response rate 60%). The majority of patients (154/175, 88.0%) and nurses (23/30, 77%) experienced RPM as very good; however, the nurses noted more downsides than did the patients. The mean scores of the negative experiences subscale were 11.5 (SD 1.1) for the patients and 10.7 (SD 0.9) for the nurses (P=.08). The mean scores of the positive experiences subscale were 11.1 (SD 1.6) for the patients and 8.5 (SD 1.9) for the nurses (P=.04). A total of 11 out of 175 patients (6.3%) were worried or anxious about what the RPM entailed, while 15 out of 30 nurses (50%) felt distressed by the responsibility that accompanied their work with RPM (P=.04). Patients found that RPM increased their own (173/175, 98.9%) and their relatives' (169/175, 96.6%) security, and all nurses (30/30, 100%) answered that they found RPM to be necessary from a safety perspective. Most patients found it to be an advantage with fewer office-based visits. Nurses found it difficult to handle different systems with different platforms, especially for smaller clinics with few patients. Another difficulty was to set the correct number of alarms for the individual patient. This caused a high number of transmissions and a risk to miss important information.
Conclusions: Both patients and nurses found that RPM increased assurance, reliance, and safety. Few patients were anxious about what the RPM entailed, while about half of the nurses felt distressed by the responsibility that accompanied their work with RPM. To increase nurses' sense of security, it seems important to adjust organizational routines and reimbursement systems and to balance the workload.
Keywords: heart failure; implantable cardioverter-defibrillator; remote patient monitoring.
©Maria Liljeroos, Ingela Thylén, Anna Strömberg. Originally published in the Journal of Medical Internet Research (http://www.jmir.org), 28.09.2020.
Conflict of interest statement
Conflicts of Interest: None declared.
Figures
Similar articles
-
Remote monitoring of implantable cardioverter defibrillators: Patient experiences and preferences for follow-up.Pacing Clin Electrophysiol. 2019 Feb;42(2):120-129. doi: 10.1111/pace.13574. Epub 2019 Jan 2. Pacing Clin Electrophysiol. 2019. PMID: 30536931 Free PMC article.
-
Effect of remote monitoring on patient-reported outcomes in European heart failure patients with an implantable cardioverter-defibrillator: primary results of the REMOTE-CIED randomized trial.Europace. 2019 Sep 1;21(9):1360-1368. doi: 10.1093/europace/euz140. Europace. 2019. PMID: 31168604 Clinical Trial.
-
Remote monitoring reduces healthcare use and improves quality of care in heart failure patients with implantable defibrillators: the evolution of management strategies of heart failure patients with implantable defibrillators (EVOLVO) study.Circulation. 2012 Jun 19;125(24):2985-92. doi: 10.1161/CIRCULATIONAHA.111.088971. Epub 2012 May 24. Circulation. 2012. PMID: 22626743 Clinical Trial.
-
The patient perspective on remote monitoring of patients with an implantable cardioverter defibrillator: Narrative review and future directions.Pacing Clin Electrophysiol. 2017 Jul;40(7):826-833. doi: 10.1111/pace.13123. Epub 2017 Jun 30. Pacing Clin Electrophysiol. 2017. PMID: 28612995 Review.
-
Implantable cardioverter-defibrillators and survival in advanced heart failure patients with continuous-flow left ventricular assist devices: a systematic review and meta-analysis.Europace. 2019 Sep 1;21(9):1353-1359. doi: 10.1093/europace/euz125. Europace. 2019. PMID: 31086951
Cited by
-
Willingness to use remote patient monitoring among cardiovascular patients in a resource-limited setting: a cross-sectional study.Front Digit Health. 2024 Sep 17;6:1437134. doi: 10.3389/fdgth.2024.1437134. eCollection 2024. Front Digit Health. 2024. PMID: 39364012 Free PMC article.
-
2023 HRS/EHRA/APHRS/LAHRS Expert Consensus Statement on Practical Management of the Remote Device Clinic.J Arrhythm. 2023 May 19;39(3):250-302. doi: 10.1002/joa3.12851. eCollection 2023 Jun. J Arrhythm. 2023. PMID: 37324757 Free PMC article.
-
2023 HRS/EHRA/APHRS/LAHRS Expert Consensus Statement on Practical Management of the Remote Device Clinic.Europace. 2023 May 19;25(5):euad123. doi: 10.1093/europace/euad123. Europace. 2023. PMID: 37208301 Free PMC article.
-
Implementation of Telemonitoring in Health Care: Facilitators and Barriers for Using eHealth for Older Adults with Chronic Conditions.Risk Manag Healthc Policy. 2023 Jan 10;16:43-53. doi: 10.2147/RMHP.S396495. eCollection 2023. Risk Manag Healthc Policy. 2023. PMID: 36647422 Free PMC article.
-
Virtual healthcare solutions in heart failure: a literature review.Front Cardiovasc Med. 2023 Sep 7;10:1231000. doi: 10.3389/fcvm.2023.1231000. eCollection 2023. Front Cardiovasc Med. 2023. PMID: 37745104 Free PMC article. Review.
References
-
- Ponikowski P, Voors AA, Anker SD, Bueno H, Cleland JGF, Coats AJS, Falk V, González-Juanatey JR, Harjola V, Jankowska EA, Jessup M, Linde C, Nihoyannopoulos P, Parissis JT, Pieske B, Riley JP, Rosano GMC, Ruilope LM, Ruschitzka F, Rutten FH, van der Meer P, Authors/Task Force Members. Document Reviewers 2016 ESC Guidelines for the diagnosis and treatment of acute and chronic heart failure: The Task Force for the diagnosis and treatment of acute and chronic heart failure of the European Society of Cardiology (ESC). Developed with the special contribution of the Heart Failure Association (HFA) of the ESC. Eur J Heart Fail. 2016 Aug;18(8):891–975. doi: 10.1002/ejhf.592. doi: 10.1002/ejhf.592. - DOI - DOI - PubMed
-
- Wijers SC, van der Kolk BYM, Tuinenburg AE, Doevendans PAF, Vos MA, Meine M. Implementation of guidelines for implantable cardioverter-defibrillator therapy in clinical practice: Which patients do benefit? Neth Heart J. 2013 Jun;21(6):274–283. doi: 10.1007/s12471-013-0407-x. http://europepmc.org/abstract/MED/23572330 - DOI - PMC - PubMed
-
- Ploux S, Varma N, Strik M, Lazarus A, Bordachar P. Optimizing implantable cardioverter-defibrillator remote monitoring: A practical guide. JACC Clin Electrophysiol. 2017 Apr;3(4):315–328. doi: 10.1016/j.jacep.2017.02.007. https://linkinghub.elsevier.com/retrieve/pii/S2405-500X(17)30183-4 - DOI - PubMed
-
- Brignole M, Auricchio A, Baron-Esquivias G, Bordachar P, Boriani G, Breithardt O, Cleland J, Deharo J, Delgado V, Elliott PM, Gorenek B, Israel CW, Leclercq C, Linde C, Mont L, Padeletti L, Sutton R, Vardas PE, ESC Committee for Practice Guidelines (CPG) Zamorano JL, Achenbach S, Baumgartner H, Bax JJ, Bueno H, Dean V, Deaton C, Erol C, Fagard R, Ferrari R, Hasdai D, Hoes AW, Kirchhof P, Knuuti J, Kolh P, Lancellotti P, Linhart A, Nihoyannopoulos P, Piepoli MF, Ponikowski P, Sirnes PA, Tamargo JL, Tendera M, Torbicki A, Wijns W, Windecker S, Document Reviewers. Kirchhof P, Blomstrom-Lundqvist C, Badano LP, Aliyev F, Bänsch D, Baumgartner H, Bsata W, Buser P, Charron P, Daubert J, Dobreanu D, Faerestrand S, Hasdai D, Hoes AW, Le Heuzey J, Mavrakis H, McDonagh T, Merino JL, Nawar MM, Nielsen JC, Pieske B, Poposka L, Ruschitzka F, Tendera M, Van Gelder IC, Wilson CM. 2013 ESC Guidelines on cardiac pacing and cardiac resynchronization therapy: The Task Force on cardiac pacing and resynchronization therapy of the European Society of Cardiology (ESC). Developed in collaboration with the European Heart Rhythm Association (EHRA) Eur Heart J. 2013 Aug;34(29):2281–2329. doi: 10.1093/eurheartj/eht150. - DOI - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Research Materials
Miscellaneous