RAAS inhibitors are not associated with mortality in COVID-19 patients: Findings from an observational multicenter study in Italy and a meta-analysis of 19 studies
- PMID: 32992048
- PMCID: PMC7521934
- DOI: 10.1016/j.vph.2020.106805
RAAS inhibitors are not associated with mortality in COVID-19 patients: Findings from an observational multicenter study in Italy and a meta-analysis of 19 studies
Abstract
Objective: The hypothesis that been set forward that use of Renin Angiotensin Aldosterone System (RAAS) inhibitors is associated with COVID-19 severity. We set-up a multicenter Italian collaboration (CORIST Project, ClinicalTrials.gov ID: NCT04318418) to retrospectively investigate the relationship between RAAS inhibitors and COVID-19 in-hospital mortality. We also carried out an updated meta-analysis on the relevant studies.
Methods: We analyzed 4069 unselected patients with laboratory-confirmed SARS-CoV-2 infection and hospitalized in 34 clinical centers in Italy from February 19, 2020 to May 23, 2020. The primary end-point in a time-to event analysis was in-hospital death, comparing patients who received angiotensin-converting-enzyme inhibitors (ACEI) or angiotensin-receptor blockers (ARB) with patients who did not. Articles for the meta-analysis were retrieved until July 13th, 2020 by searching in web-based libraries, and data were combined using the general variance-based method.
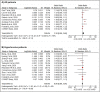
Results: Out of 4069 COVID-19 patients, 13.5% and 13.3% received ACE-I or ARB, respectively. Use of neither ACE-I nor ARB was associated with mortality (multivariable hazard ratio (HR) adjusted also for COVID-19 treatments: 0.96, 95% confidence interval 0.77-1.20 and HR = 0.89, 0.67-1.19 for ACE-I and ARB, respectively). Findings were similar restricting the analysis to hypertensive (N = 2057) patients (HR = 1.00, 0.78-1.26 and HR = 0.88, 0.65-1.20) or when ACE-I or ARB were considered as a single group. Results from the meta-analysis (19 studies, 29,057 COVID-19 adult patients, 9700 with hypertension) confirmed the absence of association.
Conclusions: In this observational study and meta-analysis of the literature, ACE-I or ARB use was not associated with severity or in-hospital mortality in COVID-19 patients.
Keywords: ACE-I; ARB; Angiotensin converting enzyme inhibitors; Angiotensin receptor blockers; COVID−19; Mortality; Sartans.
Copyright © 2020 Elsevier Inc. All rights reserved.
Figures
References
-
- Wu F., Zhao S., Yu B., Chen Y.-M., Wang W., Song Z.-G., Hu Y., Tao Z.-W., Tian J.-H., Pei Y.-Y., Yuan M.-L., Zhang Y.-L., Dai F.-H., Liu Y., Wang Q.-M., Zheng J.-J., Xu L., Holmes E.C., Zhang Y.-Z. A new coronavirus associated with human respiratory disease in China. Nature. 2020;579:265–269. - PMC - PubMed
-
- Hoffmann M., Kleine-Weber H., Schroeder S., Krüger N., Herrler T., Erichsen S., Schiergens T.S., Herrler G., Wu N.H., Nitsche A., Müller M.A., Drosten C., Pöhlmann S. Sars-cov-2 cell entry depends on ace2 and tmprss2 and is blocked by a clinically proven protease inhibitor. Cell. 2020;181:271–280.e278. - PMC - PubMed
Publication types
MeSH terms
Substances
Associated data
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous