Noninvasive continuous monitoring versus intermittent oscillometric measurements for the detection of hypotension during digestive endoscopy
- PMID: 33007051
- PMCID: PMC7531858
- DOI: 10.1371/journal.pone.0240241
Noninvasive continuous monitoring versus intermittent oscillometric measurements for the detection of hypotension during digestive endoscopy
Abstract
Background: Hemodynamic monitoring during digestive endoscopy is usually minimal and involves intermittent brachial pressure measurements. New continuous noninvasive devices to acquire instantaneous arterial blood pressure may be more sensitive to detect procedural hypotension.
Purpose: To compare the ability of noninvasive continuous monitoring with that of intermittent oscillometric measurements to detect hypotension during digestive endoscopy.
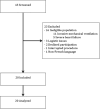
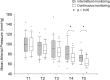
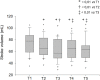
Methods: In this observational prospective study, patients scheduled for gastrointestinal endoscopy and colonoscopy under sedation were monitored using intermittent pressure measurements and a noninvasive continuous technique (ClearSight™, Edwards). Stroke volume was estimated from the arterial pressure waveform. Mean arterial pressure and stroke volume values were recorded at T1 (prior to anesthetic induction), T2 (after anesthetic induction), T3 (gastric insufflation), T4 (end of gastroscopy), T5 (colonic insufflation). Hypotension was defined as mean arterial pressure < 65 mmHg.
Results: Twenty patients (53±17 years) were included. Six patients (30%) had a hypotension detected using intermittent pressure measurements versus twelve patients (60%) using noninvasive continuous monitoring (p = 0.06). Mean arterial pressure decreased during the procedure with respect to T1 (p < 0.05), but the continuous method provided an earlier warning than the intermittent method (T3 vs T4). Nine patients (45%) had at least a 25% reduction in stroke volume, with respect to baseline.
Conclusion: Noninvasive continuous monitoring was more sensitive than intermittent measurements to detect hypotension. Estimation of stroke volume revealed profound reductions in systemic flow. Noninvasive continuous monitoring in high-risk patients undergoing digestive endoscopy under sedation could help in detecting hypoperfusion earlier than the usual intermittent blood pressure measurements.
Conflict of interest statement
We have read the journal’s policy and the authors of this manuscript have the following competing interests: BC has participated to advisory boards organized by Edwards. This does not alter our adherence to PLOS ONE policies on sharing data and materials.
Figures

Similar articles
-
Continuous noninvasive arterial blood pressure monitoring using the vascular unloading technology during complex gastrointestinal endoscopy: a prospective observational study.J Clin Monit Comput. 2019 Feb;33(1):25-30. doi: 10.1007/s10877-018-0131-6. Epub 2018 Mar 20. J Clin Monit Comput. 2019. PMID: 29556885
-
Noninvasive continuous versus intermittent arterial pressure monitoring: evaluation of the vascular unloading technique (CNAP device) in the emergency department.Scand J Trauma Resusc Emerg Med. 2014 Jan 29;22:8. doi: 10.1186/1757-7241-22-8. Scand J Trauma Resusc Emerg Med. 2014. PMID: 24472659 Free PMC article.
-
Continuous Finger-cuff versus Intermittent Oscillometric Arterial Pressure Monitoring and Hypotension during Induction of Anesthesia and Noncardiac Surgery: The DETECT Randomized Trial.Anesthesiology. 2023 Sep 1;139(3):298-308. doi: 10.1097/ALN.0000000000004629. Anesthesiology. 2023. PMID: 37265355 Clinical Trial.
-
Noninvasive BP Monitoring in the Critically Ill: Time to Abandon the Arterial Catheter?Chest. 2018 Apr;153(4):1023-1039. doi: 10.1016/j.chest.2017.10.030. Epub 2017 Nov 3. Chest. 2018. PMID: 29108815 Review.
-
Perioperative blood pressure monitoring.Best Pract Res Clin Anaesthesiol. 2019 Jun;33(2):127-138. doi: 10.1016/j.bpa.2019.05.001. Epub 2019 May 7. Best Pract Res Clin Anaesthesiol. 2019. PMID: 31582093 Review.
Cited by
-
Systemic vasoconstriction and mortality in patients with heart failure and reduced ejection fraction: A cohort of patients who underwent non-invasive hemodynamic monitoring.PLoS One. 2024 Dec 20;19(12):e0312582. doi: 10.1371/journal.pone.0312582. eCollection 2024. PLoS One. 2024. PMID: 39705294 Free PMC article.
-
Patent landscape review of non-invasive medical sensors for continuous monitoring of blood pressure and their validation in critical care practice.Front Med (Lausanne). 2023 Jul 11;10:1138051. doi: 10.3389/fmed.2023.1138051. eCollection 2023. Front Med (Lausanne). 2023. PMID: 37497278 Free PMC article. Review.
References
-
- Kim S-H, Lilot M, Sidhu KS, Rinehart J, Yu Z, Canales C, et al. Accuracy and precision of continuous noninvasive arterial pressure monitoring compared with invasive arterial pressure: a systematic review and meta-analysis. Anesthesiology 2014;120(5):1080–1097. 10.1097/aln.0000000000000226. - DOI - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources

