Acute Ischemic and Hemorrhagic Stroke in COVID-19: Mounting Evidence
- PMID: 33014653
- PMCID: PMC7526955
- DOI: 10.7759/cureus.10157
Acute Ischemic and Hemorrhagic Stroke in COVID-19: Mounting Evidence
Abstract
The novel coronavirus disease of 2019 (COVID-19) is caused by the binding of severe acute respiratory syndrome coronavirus-2 (SARS-CoV-2) to angiotensin-converting enzyme 2 (ACE2) receptors present on various locations such as the pulmonary alveolar epithelium and vascular endothelium. In COVID-19 patients, the interaction of SARS-CoV-2 with these receptors in the cerebral blood vessels has been attributed to stroke. Although the incidence of acute ischemic stroke is relatively low, ranging from 1% to 6%, the mortality associated with it is substantially high, reaching as high as 38%. This case series describes three distinct yet similar scenarios of COVID-19 positive patients with several underlying comorbidities, wherein two of the patients presented to our hospital with sudden onset right-sided weakness, later diagnosed with ischemic stroke, and one patient who developed an acute intracerebral hemorrhage during his hospital stay. The patients were diagnosed with acute stroke as a complication of COVID-19 infection. We also provide an insight into the possible mechanisms responsible for the life-threatening complication. Physicians should have a low threshold for suspecting stroke in COVID-19 patients, and close observation should be kept on such patients particularly those with clinical evidence of traditional risk factors.
Keywords: co-morbidity; complication; covid-19; intracerebral hemorrhage; mortality; stroke.
Copyright © 2020, Rajdev et al.
Conflict of interest statement
The authors have declared that no competing interests exist.
Figures

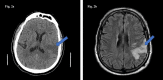
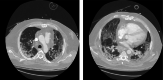
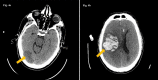
References
-
- Coronavirus disease (COVID-19). Situation Report - 206. [Aug;2020 ];https://www.who.int/docs/default-source/coronaviruse/situation-reports/2... 2020
Publication types
LinkOut - more resources
Full Text Sources
Miscellaneous
