Gastroesophageal reflux disease in pediatric esophageal atresia: Assessment of clinical symptoms and pH-impedance data
- PMID: 33014720
- PMCID: PMC7515750
- DOI: 10.5409/wjcp.v9.i2.29
Gastroesophageal reflux disease in pediatric esophageal atresia: Assessment of clinical symptoms and pH-impedance data
Abstract
Background: Esophageal atresia (EA) is the most common congenital anomaly of the gastrointestinal tract. Gastroesophageal reflux disease (GERD) is a frequent and lifelong problem in these patients. GERD can be asymptomatic and the incidence of esophageal gastric and intestinal metaplasia (Barrett's esophagus) is increased in adults with EA compared with the general population. Timely and accurate diagnosis of GERD is important to reduce long-term problems and this may be achieved by pH-impedance testing.
Aim: To assess symptoms and pH-impedance data in children after EA, in order to identify their specific features of GERD.
Methods: This study was conducted from November 2017 to February 2020 and involved 37 children who had undergone EA via open surgical repair (51.35% boys, 48.65% girls; age range: 1-14 years, median: 4.99 years). GERD diagnosis was made based on multichannel intraluminal impedance/pH study and two groups were established: EA without GERD, n = 17; EA with GERD, n = 20. A control group was established with 66 children with proven GERD (68.18% boys, 31.82% girls; median age: 7.21 years), composed of a nonerosive reflux disease (referred to as NERD) group (n = 41) and a reflux esophagitis group (n = 25). Upper gastrointestinal endoscopy with a mucosal esophageal biopsy was performed on all patients.
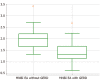
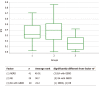
Results: The most frequently observed symptom in EA patients with GERD and without GERD was cough (70% and 76.5% respectively). The number of patients with positive symptom association probability in the EA groups was significantly larger in the EA without GERD group (P = 0.03). In the control reflux esophagitis group, prevalence of gastrointestinal symptoms was significantly higher than in the NERD group (P = 0.017). For both EA groups, there was strong correlation with index of proximal events (IPE) and total proximal events (EA with GERD: 0.96, P < 0.001; EA without GERD: 0.97, P < 0.001) but level of IPE was significantly lower than in GERD patients without any surgical treatment (P < 0.001). Data on distal mean nocturnal baseline impedance were significantly different between the EA with GERD group (P < 0.001) and the two control groups but not between EA without GERD and the two control groups.
Conclusion: Mean nocturnal baseline impedance may have diagnostic value for GERD in EA children after open surgical repair. IPE might be an additional parameter of pH-impedance monitoring.
Keywords: Esophageal atresia; Gastroesophageal reflux disease; Mean nocturnal baseline impedance; Nonerosive reflux disease; Pediatric; Proximal reflux; Reflux esophagitis; pH-impedance testing.
©The Author(s) 2020. Published by Baishideng Publishing Group Inc. All rights reserved.
Conflict of interest statement
Conflict-of-interest statement: The authors declare no potential financial interests.
Figures


Similar articles
-
Assessment of Clinical Symptoms and Multichannel Intraluminal Impedance and pH Monitoring in Children After Thoracoscopic Repair of Esophageal Atresia and Distal Tracheoesophageal Fistula.Adv Clin Exp Med. 2016 Sep-Oct;25(5):917-922. doi: 10.17219/acem/61844. Adv Clin Exp Med. 2016. PMID: 28028956
-
Evaluation of Gastroesophageal Reflux by Combined Multichannel Intraluminal Impedance and pH Monitoring and Esophageal Motility Patterns in Children with Esophageal Atresia.Eur J Pediatr Surg. 2016 Aug;26(4):322-31. doi: 10.1055/s-0035-1564715. Epub 2015 Oct 7. Eur J Pediatr Surg. 2016. PMID: 26445355
-
Detection of reflux-symptom association in children with esophageal atresia by video-pH-impedance study.World J Gastroenterol. 2020 Jul 28;26(28):4159-4169. doi: 10.3748/wjg.v26.i28.4159. World J Gastroenterol. 2020. PMID: 32821077 Free PMC article.
-
Surveillance in Patients With Esophageal Atresia/Tracheoesophageal Fistula.Curr Gastroenterol Rep. 2017 Jan;19(1):4. doi: 10.1007/s11894-017-0541-5. Curr Gastroenterol Rep. 2017. PMID: 28144844 Review.
-
Novel Diagnostic Techniques in the Evaluation of Gastroesophageal Reflux Disease (GERD).Dig Dis Sci. 2023 Jun;68(6):2226-2236. doi: 10.1007/s10620-023-07901-9. Epub 2023 Apr 18. Dig Dis Sci. 2023. PMID: 37071244 Review.
References
-
- Sfeir R, Bonnard A, Khen-Dunlop N, Auber F, Gelas T, Michaud L, Podevin G, Breton A, Fouquet V, Piolat C, Lemelle JL, Petit T, Lavrand F, Becmeur F, Polimerol ML, Michel JL, Elbaz F, Habonimana E, Allal H, Lopez E, Lardy H, Morineau M, Pelatan C, Merrot T, Delagausie P, de Vries P, Levard G, Buisson P, Sapin E, Jaby O, Borderon C, Weil D, Gueiss S, Aubert D, Echaieb A, Fourcade L, Breaud J, Laplace C, Pouzac M, Duhamel A, Gottrand F. Esophageal atresia: data from a national cohort. J Pediatr Surg. 2013;48:1664–1669. - PubMed
-
- Little DC, Rescorla FJ, Grosfeld JL, West KW, Scherer LR, Engum SA. Long-term analysis of children with esophageal atresia and tracheoesophageal fistula. J Pediatr Surg. 2003;38:852–856. - PubMed
-
- Krishnan U, Mousa H, Dall'Oglio L, Homaira N, Rosen R, Faure C, Gottrand F. ESPGHAN-NASPGHAN Guidelines for the Evaluation and Treatment of Gastrointestinal and Nutritional Complications in Children With Esophageal Atresia-Tracheoesophageal Fistula. J Pediatr Gastroenterol Nutr. 2016;63:550–570. - PubMed
-
- Vandenplas Y, Rudolph CD, Di Lorenzo C, Hassall E, Liptak G, Mazur L, Sondheimer J, Staiano A, Thomson M, Veereman-Wauters G, Wenzl TG; North American Society for Pediatric Gastroenterology Hepatology and Nutrition; European Society for Pediatric Gastroenterology Hepatology and Nutrition. Pediatric gastroesophageal reflux clinical practice guidelines: joint recommendations of the North American Society for Pediatric Gastroenterology, Hepatology, and Nutrition (NASPGHAN) and the European Society for Pediatric Gastroenterology, Hepatology, and Nutrition (ESPGHAN) J Pediatr Gastroenterol Nutr. 2009;49:498–547. - PubMed
LinkOut - more resources
Full Text Sources

