Confirmation of Pulmonary Vein Isolation with High-Density Mapping: Comparison to Traditional Workflows
- PMID: 33024494
- PMCID: PMC7533127
- DOI: 10.4022/jafib.2361
Confirmation of Pulmonary Vein Isolation with High-Density Mapping: Comparison to Traditional Workflows
Abstract
Pulmonary vein isolation (PVI) is the cornerstone of atrial fibrillation (AF) ablation. Yet tools and techniques used for confirmation of PVI vary greatly, and it is unclear whether the use of any particular combination of tools and techniques provides greater sensitivity for identifying gaps periprocedurally. It has been suggested the use of a high-density mapping catheter, which enables simultaneous recording of adjacent bipolar EGMs in two directions, may provide improved sensitivity for gap identification. Anonymized, acute procedural data was prospectively collected in AF ablation cases utilizing various workflows for confirmation of PVI. Post-hoc analysis was performed to evaluate the incidence of gaps detected by different diagnostic catheter technologies, including a high-density mapping catheter and circular mapping catheters (CMCs), and common techniques such as pacing the ablation lines. A total of 139 cases were included across three subgroup analyses: 99 cases were included in an indirect comparison of three mapping catheter technologies, revealing gaps in 36.7%, 38.9%, and 81.8% of cases utilizing a 10-pole CMC, 20-pole CMC, and a high-density mapping catheter, respectively; a direct comparison of diagnostic catheter technologies in 18 cryoballoon ablation cases revealed residual gaps in 22.2% of patients identified by high-density mapping which were missed previously with the use of a 3.3F CMC; in 22 cases utilizing a technique of pacing the ablation lines, high-density mapping identified residual gaps in 68.2% of patients. This proof of concept analysis demonstrated that the use of a high-density catheter which records orthogonal bipoles simultaneously, appears to improve acute detection of gaps in PVI lines relative to other commonly utilized techniques and technologies. The long-term impact of ablating these concealed gaps remains unclear. Further study, including direct comparison of diagnostic catheter technologies in a randomized setting with long-term followup, is warranted.
Keywords: Atrial fibrillation; High density mapping; Pulmonary vein isolation (PVI).
Figures


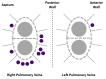
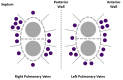
References
-
- Gerstenfeld Edward P, Dixit Sanjay, Callans David, Rho Robert, Rajawat Yadavendra, Zado Erica, Marchlinski Francis E. Utility of exit block for identifying electrical isolation of the pulmonary veins. J. Cardiovasc. Electrophysiol. 2002 Oct;13 (10):971–9. - PubMed
-
- Vijayaraman Pugazhendhi, Dandamudi Gopi, Naperkowski Angela, Oren Jess, Storm Randle, Ellenbogen Kenneth A. Assessment of exit block following pulmonary vein isolation: far-field capture masquerading as entrance without exit block. Heart Rhythm. 2012 Oct;9 (10):1653–9. - PubMed
-
- Yamane Teiichi, Matsuo Seiichiro, Date Taro, Lellouche Nicolas, Hioki Mika, Narui Ryosuke, Ito Keiichi, Tanigawa Shin-ichi, Yamashita Seigo, Tokuda Michifumi, Yoshida Hiroshi, Inada Keiichi, Shibayama Kenri, Miyanaga Satoru, Miyazaki Hidekazu, Abe Kunihiko, Sugimoto Ken-ichi, Yoshimura Michihiro. Repeated provocation of time- and ATP-induced early pulmonary vein reconnections after pulmonary vein isolation: eliminating paroxysmal atrial fibrillation in a single procedure. Circ Arrhythm Electrophysiol. 2011 Oct;4 (5):601–8. - PubMed
-
- Macle Laurent, Khairy Paul, Weerasooriya Rukshen, Novak Paul, Verma Atul, Willems Stephan, Arentz Thomas, Deisenhofer Isabel, Veenhuyzen George, Scavée Christophe, Jaïs Pierre, Puererfellner Helmut, Levesque Sylvie, Andrade Jason G, Rivard Lena, Guerra Peter G, Dubuc Marc, Thibault Bernard, Talajic Mario, Roy Denis, Nattel Stanley. Adenosine-guided pulmonary vein isolation for the treatment of paroxysmal atrial fibrillation: an international, multicentre, randomised superiority trial. Lancet. 2015 Aug 15;386 (9994):672–9. - PubMed
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous
