Coronary Vascular Function and Cardiomyocyte Injury: A Report From the WISE-CVD
- PMID: 33028098
- PMCID: PMC8079158
- DOI: 10.1161/ATVBAHA.120.314260
Coronary Vascular Function and Cardiomyocyte Injury: A Report From the WISE-CVD
Abstract
Objective: Women with symptoms or signs of myocardial ischemia but no obstructive coronary artery disease (INOCA) often have coronary vascular dysfunction and elevated risk for adverse cardiovascular events. We hypothesized that u-hscTnI (ultra-high-sensitivity cardiac troponin I), a sensitive indicator of ischemic cardiomyocyte injury, is associated with coronary vascular dysfunction in women with INOCA. Approach and Results: Women (N=263) with INOCA enrolled in the WISE-CVD study (Women's Ischemic Syndrome Evaluation-Coronary Vascular Dysfunction) underwent invasive coronary vascular function testing and u-hscTnI measurements (Simoa HD-1 Analyzer; Quanterix Corporation, Lexington, MA). Logistic regression models, adjusted for traditional cardiovascular risk factors were used to evaluate associations between u-hscTnI and coronary vascular function. Women with coronary vascular dysfunction (microvascular constriction and limited coronary epicardial dilation) had higher plasma u-hscTnI levels (both P=0.001). u-hscTnI levels were associated with microvascular constriction (odds ratio, 1.38 per doubling of u-hscTnI [95% CI, 1.03-1.84]; P=0.033) and limited coronary epicardial dilation (odds ratio, 1.37 per doubling of u-hscTnI [95% CI, 1.04-1.81]; P=0.026). u-hscTnI levels were not associated with microvascular dilation or coronary epicardial constriction.
Conclusions: Our findings indicate that higher u-hscTnI is associated with coronary vascular dysfunction in women with INOCA. This suggests that ischemic cardiomyocyte injury in the setting of coronary vascular dysfunction has the potential to contribute to adverse cardiovascular outcomes observed in these women. Additional studies are needed to confirm and investigate mechanisms underlying these findings in INOCA. Registration: URL: https://www.clinicaltrials.gov; Unique identifier: NCT00832702.
Keywords: INOCA; acetylcholine; cardiomyocyte injury; coronary artery disease; myocardial ischemia; risk; troponin I; vascular function.
Conflict of interest statement
Figures

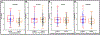
Comment in
-
Establishing the Link Between Coronary Microvascular Disease and Cardiomyocyte Injury.Arterioscler Thromb Vasc Biol. 2020 Dec;40(12):2815-2817. doi: 10.1161/ATVBAHA.120.315368. Epub 2020 Nov 24. Arterioscler Thromb Vasc Biol. 2020. PMID: 33232206 No abstract available.
Similar articles
-
Ultra-high sensitivity cardiac troponin-I concentration and left ventricular structure and function in women with ischemia and no obstructive coronary artery disease.Am Heart J Plus. 2022 Jan;13:100115. doi: 10.1016/j.ahjo.2022.100115. Epub 2022 Mar 3. Am Heart J Plus. 2022. PMID: 35784010 Free PMC article.
-
High-Sensitivity Troponin in Patients With Coronary Artery Endothelial Dysfunction.J Invasive Cardiol. 2018 Nov;30(11):406-410. J Invasive Cardiol. 2018. PMID: 30373950
-
Prevalence of Coronary Endothelial and Microvascular Dysfunction in Women with Symptoms of Ischemia and No Obstructive Coronary Artery Disease Is Confirmed by a New Cohort: The NHLBI-Sponsored Women's Ischemia Syndrome Evaluation-Coronary Vascular Dysfunction (WISE-CVD).J Interv Cardiol. 2019 Mar 11;2019:7169275. doi: 10.1155/2019/7169275. eCollection 2019. J Interv Cardiol. 2019. PMID: 31772544 Free PMC article.
-
Treatment of coronary microvascular dysfunction.Cardiovasc Res. 2020 Mar 1;116(4):856-870. doi: 10.1093/cvr/cvaa006. Cardiovasc Res. 2020. PMID: 32087007 Free PMC article. Review.
-
Ischemia and no obstructive coronary arteries (INOCA): A narrative review.Atherosclerosis. 2022 Dec;363:8-21. doi: 10.1016/j.atherosclerosis.2022.11.009. Epub 2022 Nov 12. Atherosclerosis. 2022. PMID: 36423427 Free PMC article. Review.
Cited by
-
The relation of circulating cell division cycle 42 expression with Th1, Th2, and Th17 cells, adhesion molecules, and biochemical indexes in coronary heart disease patients.Ir J Med Sci. 2022 Oct;191(5):2085-2090. doi: 10.1007/s11845-021-02836-4. Epub 2021 Nov 22. Ir J Med Sci. 2022. PMID: 34811660
-
Evaluation of coronary microvascular dysfunction using magnetocardiography: A new application to an old technology.Am Heart J Plus. 2024 Jul 10;44:100424. doi: 10.1016/j.ahjo.2024.100424. eCollection 2024 Aug. Am Heart J Plus. 2024. PMID: 39108843 Free PMC article.
-
Ultra-high sensitivity cardiac troponin-I concentration and left ventricular structure and function in women with ischemia and no obstructive coronary artery disease.Am Heart J Plus. 2022 Jan;13:100115. doi: 10.1016/j.ahjo.2022.100115. Epub 2022 Mar 3. Am Heart J Plus. 2022. PMID: 35784010 Free PMC article.
-
Syndrome of Nonobstructive Coronary Artery Diseases: A Comprehensive Overview of Open Artery Ischemia.Am J Med. 2021 Nov;134(11):1321-1329. doi: 10.1016/j.amjmed.2021.06.038. Epub 2021 Jul 31. Am J Med. 2021. PMID: 34343507 Free PMC article. Review.
-
Latest from the WISE: Contributions to the Understanding of Ischemia and Heart Failure among Women with No Obstructive Coronary Arteries.Rev Cardiovasc Med. 2023 Mar 15;24(3):90. doi: 10.31083/j.rcm2403090. eCollection 2023 Mar. Rev Cardiovasc Med. 2023. PMID: 39077501 Free PMC article. Review.
References
-
- Merz CNB, Pepine CJ, Walsh MN, Fleg JL, Camici PG, Chilian WM, Clayton JA, Cooper LS, Crea F, Carli MD, Douglas PS, Galis ZS, Gurbel P, Handberg EM, Hasan A, Hill JA, Hochman JS, Iturriaga E, Kirby R, Levine GN, Libby P, Lima J, Mehta P, Desvigne-Nickens P, Olive M, Pearson GD, Quyyumi AA, Reynolds H, Robinson B, Sopko G, Taqueti V, Wei J, Wenger N. Ischemia and no obstructive coronary artery disease (inoca). Circulation. 2017;135:1075–1092 - PMC - PubMed
-
- Pepine CJ, Anderson RD, Sharaf BL, Reis SE, Smith KM, Handberg EM, Johnson BD, Sopko G, Bairey Merz CN. Coronary microvascular reactivity to adenosine predicts adverse outcome in women evaluated for suspected ischemia results from the national heart, lung and blood institute wise (women's ischemia syndrome evaluation) study. Journal of the American College of Cardiology. 2010;55:2825–2832 - PMC - PubMed
-
- Reis SE, Holubkov R, Conrad Smith AJ, Kelsey SF, Sharaf BL, Reichek N, Rogers WJ, Merz CN, Sopko G, Pepine CJ. Coronary microvascular dysfunction is highly prevalent in women with chest pain in the absence of coronary artery disease: Results from the nhlbi wise study. American heart journal. 2001;141:735–741 - PubMed
-
- von Mering GO, Arant CB, Wessel TR, McGorray SP, Bairey Merz CN, Sharaf BL, Smith KM, Olson MB, Johnson BD, Sopko G, Handberg E, Pepine CJ, Kerensky RA. Abnormal coronary vasomotion as a prognostic indicator of cardiovascular events in women: Results from the national heart, lung, and blood institute-sponsored women's ischemia syndrome evaluation (wise). Circulation. 2004;109:722–725 - PubMed
Publication types
MeSH terms
Substances
Associated data
Grants and funding
- N01 HV068161/HV/NHLBI NIH HHS/United States
- N01 HV068163/HL/NHLBI NIH HHS/United States
- T32 HL069751/HL/NHLBI NIH HHS/United States
- UL1 TR000124/TR/NCATS NIH HHS/United States
- K23 HL151867/HL/NHLBI NIH HHS/United States
- UL1 TR001427/TR/NCATS NIH HHS/United States
- N01 HV068164/HV/NHLBI NIH HHS/United States
- N01 HV068162/HL/NHLBI NIH HHS/United States
- K23 HL105787/HL/NHLBI NIH HHS/United States
- UL1 TR001881/TR/NCATS NIH HHS/United States
- R01 HL090957/HL/NHLBI NIH HHS/United States
- R03 AG032631/AG/NIA NIH HHS/United States
- U54 AG065141/AG/NIA NIH HHS/United States
- M01 RR000425/RR/NCRR NIH HHS/United States
- R01 HL111362/HL/NHLBI NIH HHS/United States
LinkOut - more resources
Full Text Sources
Medical
Research Materials

