Neuropathology of patients with COVID-19 in Germany: a post-mortem case series
- PMID: 33031735
- PMCID: PMC7535629
- DOI: 10.1016/S1474-4422(20)30308-2
Neuropathology of patients with COVID-19 in Germany: a post-mortem case series
Abstract
Background: Prominent clinical symptoms of COVID-19 include CNS manifestations. However, it is unclear whether severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), the causative agent of COVID-19, gains access to the CNS and whether it causes neuropathological changes. We investigated the brain tissue of patients who died from COVID-19 for glial responses, inflammatory changes, and the presence of SARS-CoV-2 in the CNS.
Methods: In this post-mortem case series, we investigated the neuropathological features in the brains of patients who died between March 13 and April 24, 2020, in Hamburg, Germany. Inclusion criteria comprised a positive test for SARS-CoV-2 by quantitative RT-PCR (qRT-PCR) and availability of adequate samples. We did a neuropathological workup including histological staining and immunohistochemical staining for activated astrocytes, activated microglia, and cytotoxic T lymphocytes in the olfactory bulb, basal ganglia, brainstem, and cerebellum. Additionally, we investigated the presence and localisation of SARS-CoV-2 by qRT-PCR and by immunohistochemistry in selected patients and brain regions.
Findings: 43 patients were included in our study. Patients died in hospitals, nursing homes, or at home, and were aged between 51 years and 94 years (median 76 years [IQR 70-86]). We detected fresh territorial ischaemic lesions in six (14%) patients. 37 (86%) patients had astrogliosis in all assessed regions. Activation of microglia and infiltration by cytotoxic T lymphocytes was most pronounced in the brainstem and cerebellum, and meningeal cytotoxic T lymphocyte infiltration was seen in 34 (79%) patients. SARS-CoV-2 could be detected in the brains of 21 (53%) of 40 examined patients, with SARS-CoV-2 viral proteins found in cranial nerves originating from the lower brainstem and in isolated cells of the brainstem. The presence of SARS-CoV-2 in the CNS was not associated with the severity of neuropathological changes.
Interpretation: In general, neuropathological changes in patients with COVID-19 seem to be mild, with pronounced neuroinflammatory changes in the brainstem being the most common finding. There was no evidence for CNS damage directly caused by SARS-CoV-2. The generalisability of these findings needs to be validated in future studies as the number of cases and availability of clinical data were low and no age-matched and sex-matched controls were included.
Funding: German Research Foundation, Federal State of Hamburg, EU (eRARE), German Center for Infection Research (DZIF).
Copyright © 2020 Elsevier Ltd. All rights reserved.
Figures

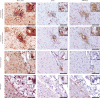



Comment in
-
Catch me if you can: SARS-CoV-2 detection in brains of deceased patients with COVID-19.Lancet Neurol. 2020 Nov;19(11):883-884. doi: 10.1016/S1474-4422(20)30371-9. Epub 2020 Oct 5. Lancet Neurol. 2020. PMID: 33031734 Free PMC article. No abstract available.
-
Isolated bulbar palsy after SARS-CoV-2 infection.Lancet Neurol. 2021 Mar;20(3):169-170. doi: 10.1016/S1474-4422(21)00025-9. Lancet Neurol. 2021. PMID: 33609467 Free PMC article. No abstract available.
References
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Research Materials
Miscellaneous

