Efficacy of Dapagliflozin on Renal Function and Outcomes in Patients With Heart Failure With Reduced Ejection Fraction: Results of DAPA-HF
- PMID: 33040613
- PMCID: PMC7834909
- DOI: 10.1161/CIRCULATIONAHA.120.050391
Efficacy of Dapagliflozin on Renal Function and Outcomes in Patients With Heart Failure With Reduced Ejection Fraction: Results of DAPA-HF
Abstract
Background: Many patients with heart failure and reduced ejection fraction (HFrEF) have chronic kidney disease that complicates pharmacological management and is associated with worse outcomes. We assessed the safety and efficacy of dapagliflozin in patients with HFrEF, according to baseline kidney function, in the DAPA-HF trial (Dapagliflozin and Prevention of Adverse-outcomes in Heart Failure). We also examined the effect of dapagliflozin on kidney function after randomization.
Methods: Patients who have HFrEF with or without type 2 diabetes and an estimated glomerular filtration rate (eGFR) ≥30 mL·min-1·1.73 m-2 were enrolled in DAPA-HF. We calculated the incidence of the primary outcome (cardiovascular death or worsening heart failure) according to eGFR category at baseline (<60 and ≥60 mL·min-1·1.73 m-2) and used eGFR at baseline as a continuous measure, as well. Secondary cardiovascular outcomes and a prespecified composite renal outcome (≥50% sustained decline eGFR, end-stage renal disease, or renal death) were also examined, along with a decline in eGFR over time.
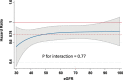
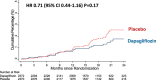
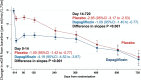
Results: Of 4742 patients with a baseline eGFR, 1926 (41%) had eGFR <60 mL·min-1·1.73 m-2. The effect of dapagliflozin on the primary and secondary outcomes did not differ by eGFR category or examining eGFR as a continuous measurement. The hazard ratio (95% CI) for the primary end point in patients with chronic kidney disease was 0.71 (0.59-0.86) versus 0.77 (0.64-0.93) in those with an eGFR ≥60 mL·min-1·1.73 m-2 (interaction P=0.54). The composite renal outcome was not reduced by dapagliflozin (hazard ratio=0.71 [95% CI, 0.44-1.16]; P=0.17) but the rate of decline in eGFR between day 14 and 720 was less with dapagliflozin, -1.09 (-1.40 to -0.77) versus placebo -2.85 (-3.17 to -2.53) mL·min-1·1.73 m-2 per year (P<0.001). This was observed in those with and without type 2 diabetes (P for interaction=0.92).
Conclusions: Baseline kidney function did not modify the benefits of dapagliflozin on morbidity and mortality in HFrEF, and dapagliflozin slowed the rate of decline in eGFR, including in patients without diabetes. Registration: URL: https://www.clinicaltrials.gov; Unique identifier: NCT03036124.
Keywords: heart failure; kidney function tests; renal insufficiency, chronic; sodium-glucose transporter 2 inhibitors.
Conflict of interest statement
Dr Jhund’s employer the University of Glasgow has been remunerated by AstraZeneca for working on the DAPA-HF (Dapagliflozin and Prevention of Adverse-outcomes in Heart Failure) and DELIVER trial (Dapagliflozin Evaluation to Improve the Lives of Patients With Preserved Ejection Fraction Heart Failure) and speakers fees from AstraZeneca and grants from Boehringer Ingelheim. Dr Solomon reports grants from AstraZeneca, Bellerophon, Celladon, Ionis, Lone Star Heart, Mesoblast, National Institutes of Health/National Heart, Lung, and Blood Institute, Sanofi Pasteur, and Eidos; grants and personal fees from Alnylam, Amgen, AstraZeneca, BMS, Gilead, GSK, MyoKardia, Novartis, Theracos, Bayer, and Cytokinetics; and personal fees from Akros, Corvia, Ironwood, Merck, Roche, Takeda, Quantum Genomics, AoBiome, Janssen, Cardiac Dimensions, Tenaya, and Daichi-Sankyo. Dr Docherty’s employer the University of Glasgow has been remunerated by AstraZeneca for working on the DAPA-HF trial. Dr Anand reported receiving personal fees from AstraZeneca during the conduct of the study and personal fees from Amgen, ARCA, Boston Scientific Corporation, Boehringer Ingelheim, LivaNova, and Zensun outside the submitted work. Dr Heerspink reports consulting for AbbVie, Astellas, AstraZeneca, Bayer, Boehringer Ingelheim, Chinook, CSL Behring, Fresenius, Gilead, Janssen, Merck, Mitsubishi Tanabe, Mundi Pharma, and Retrophin, with a policy that honoraria are paid to his employer. Dr de Boer reported receiving grants from Abbott, Bristol-Myers Squibb, and Novo Nordisk; personal fees from Abbott; and grants and personal fees from Novartis, Roche, and AstraZeneca outside the submitted work. Dr Desai reported receiving personal fees from Abbott, Biofourmis, Boston Scientific, Boehringer Ingelheim, Merck, Regeneron, and Relypsa and grants and personal fees from AstraZeneca, Alnylam, and Novartis outside the submitted work. Dr Kitakaze reported receiving grants and personal fees from AstraZeneca during the conduct of the study and grants from the Japanese government, the Japan Heart Foundation, and the Japan Agency for Medical Research and Development; grants and personal fees from Asteras, Sanofi, Pfizer, Ono, Novartis, Tanabe-Mitubishi, and Takeda; and personal fees from Daiichi Sankyo, Bayer, Behringer, Kowa, Sawai, Merck Sharp & Dohme, Shionogi, Kureha, Japan Medical Data, Taisho-Toyama, and Toa Eiyo outside the submitted work. Dr Merkely reported receiving personal fees from AstraZeneca and Servier. Dr O’Meara reported consultation and speaker fees being paid to the Montreal Heart Institute Research Center from Amgen, Merck, and Novartis; receiving consultation and speaker fees from AstraZeneca, Bayer, and Boehringer Ingelheim; serving on a steering committee and as a national leader for clinical studies with fees paid to Montreal Heart Institute Research Center from American Regent, AstraZeneca, Cytokinetics, Merck, and Novartis; and clinical trial participation from Amgen, Abbott, American Regent, AstraZeneca, Bayer, Boehringer Ingelheim, Cytokinetics, Eidos, Novartis, Merck, Pfizer, and Sanofi. Dr Schou reported receiving personal fees and nonfinancial support from AstraZeneca and personal fees from Novo Nordisk and Boehringer Ingelheim. Dr Tereshchenko reports personal fees from Servier, AstraZeneca, Pfizer, Novartis, and Boehringer Ingelheim. Dr Verma received financial support from AstraZeneca for the conduct of DAPA-HF at his institute. He has also received grants and personal fees for speaker honoraria and advisory board participation from AstraZeneca, Bayer, Boehringer Ingelheim, Janssen, and Merck. He has received grants and personal fees for advisory board participation from Amgen, grants from Bristol-Myers Squibb, personal fees for speaker honoraria and advisory board participation from Eli Lilly, Novo Nordisk, and Sanofi, and personal fees for speaker honoraria from EOCI Pharmacomm Ltd, Novartis, Sun Pharmaceuticals, and Toronto Knowledge Translation Working Group. Dr Inzucchi reports personal fees and nonfinancial support from AstraZeneca, Boehringer Ingelheim, Sanofi/Lexicon, Merck, VTV Therapeutics, and Abbott/Alere, as well as personal fees from AstraZeneca and Zafgen. Dr Køber reports other support from AstraZeneca and personal fees from Novartis and Bristol-Myers Squibb as a speaker. Dr Kosiborod reports personal fees from AstraZeneca; grants, personal fees, and other from AstraZeneca; grants and personal fees from Boehringer Ingelheim; and personal fees from Sanofi, Amgen, NovoNordisk, Merck (Diabetes), Eisai, Janssen, Bayer, GlaxoSmithKline, Glytec, Intarcia, Novartis, Applied Therapeutics, Amarin, and Eli Lilly. Dr Martinez reports personal fees from AstraZeneca. Dr Ponikowski reports personal fees and other from AstraZeneca, Boehringer Ingelheim, Bayer, BMS, Cibiem, Novartis, and RenalGuard; personal fees from Pfizer, Servier, Respicardia, and Berlin-Chemie; other from Amgen; and grants, personal fees, and other from Vifor Pharma. Dr Sabatine reports grants from Bayer, Daiichi-Sankyo, Eisai, GlaxoSmithKline, Pfizer, Poxel, Quark Pharmaceuticals, and Takeda; grants and personal fees from Amgen, AstraZeneca, Intarcia, Janssen Research and Development, The Medicines Company, MedImmune, Merck, and Novartis; and personal fees from Anthos Therapeutics, Bristol-Myers Squibb, CVS Caremark, DalCor, Dynamix, Esperion, IFM Therapeutics, and Ionis. Dr Sabatine is a member of the TIMI Study Group, which has also received institutional research grant support through Brigham and Women’s Hospital from Abbott, Aralez, Roche, and Zora Biosciences. Drs Langkilde, Bengtsson, and Sjöstrand are full-time employees of AstraZeneca. Dr McMurray s employer the University of Glasgow has been remunerated by AstraZeneca for working on the DAPA-HF and DELIVER trial, Cardiorentis, Amgen, Oxford University/Bayer, Theracos, Abbvie, Novartis, Glaxo Smith Kline, Vifor-Fresenius, Kidney Research UK, and Novartis, and other support from Bayer, DalCor, Pfizer, Merck, Bristol Myers, and Squibb, as well.
Figures

Comment in
-
Sodium-Glucose Cotransporter 2 Inhibitors in Patients With Heart Failure With Reduced Ejection Fraction: The Heart and Kidney Working Better Together.Circulation. 2021 Jan 26;143(4):322-325. doi: 10.1161/CIRCULATIONAHA.120.052048. Epub 2021 Jan 25. Circulation. 2021. PMID: 33493029 Free PMC article. No abstract available.
References
-
- Damman K, Valente MA, Voors AA, O’Connor CM, van Veldhuisen DJ, Hillege HL. Renal impairment, worsening renal function, and outcome in patients with heart failure: an updated meta-analysis. Eur Heart J. 2014; 35:455–469. doi: 10.1093/eurheartj/eht386 - PubMed
-
- Damman K, Masson S, Lucci D, Gorini M, Urso R, Maggioni AP, Tavazzi L, Tarantini L, Tognoni G, Voors A, et al. Progression of renal impairment and chronic kidney disease in chronic heart failure: an analysis from GISSI-HF. J Card Fail. 2017; 23:2–9. doi: 10.1016/j.cardfail.2016.09.006 - PubMed
-
- Beldhuis IE, Streng KW, Ter Maaten JM, Voors AA, Van Der Meer P, Rossignol P, McMurray JJV, Damman K. Renin-angiotensin system inhibition, worsening renal function, and outcome in heart failure patients with reduced and preserved ejection fraction: a meta-analysis of published study data. Circ Hear Fail. 2017; 10:e003588 doi: 10.1161/CIRCHEARTFAILURE.116.003588 - PubMed
-
- Zinman B, Wanner C, Lachin JM, Fitchett D, Bluhmki E, Hantel S, Mattheus M, Devins T, Johansen OE, Woerle HJ, et al. Empagliflozin, cardiovascular outcomes, and mortality in type 2 diabetes. N Engl J Med. 2015; 373:2117–2128. doi: 10.1056/NEJMc1600827 - PubMed
-
- Neal B, Perkovic V, Mahaffey KW, de Zeeuw D, Fulcher G, Erondu N, Shaw W, Law G, Desai M, Matthews DR; CANVAS Program Collaborative Group. Canagliflozin and cardiovascular and renal events in type 2 diabetes. N Engl J Med. 2017; 377:644–657. doi: 10.1056/NEJMoa1611925 - PubMed
Publication types
MeSH terms
Substances
Associated data
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Research Materials
Miscellaneous

