Contribution of Substance Use in Acute Injuries With Regards to the Intent, Nature and Context of Injury: A CHIRPP Database Study
- PMID: 33042717
- PMCID: PMC7538210
- DOI: 10.7759/cureus.10282
Contribution of Substance Use in Acute Injuries With Regards to the Intent, Nature and Context of Injury: A CHIRPP Database Study
Abstract
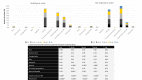
Introduction Using the Canadian Hospitals Injury Reporting and Prevention Program (CHIRPP) sentinel surveillance system, the objective of this study was to compare intent, circumstances, injury type and patient demographics in patients who used a substance prior to the injury versus those who did not use any substances. Methods Data were retrospectively collected from November 1st 2016 to October 31st 2017. All patients presenting to the Hôpital de l'Enfant-Jésus ED following trauma were included, aside from those who left without seeing a physician or had no physical injury (e.g., overdose without any trauma was excluded). Patients voluntarily completed a standardised form or agreed to be contacted later. Medical charts of all attendances were reviewed by the CHIRPP's program coordinator. Substance use included illicit drugs, medications for recreational purposes, alcohol or other used either by the patient or another person involved. Results A total of 12,857 patients were included. Substance use was involved in 701 (5.5%) cases and was associated with injuries sustained by males (p < .001). The mean age of patients injured while using substances was 42.8 years, compared to 45.5 years in those who did not use substances (p < .001). Substance use was involved in 3.6% of unintentional injuries, compared to 26.2% of injuries intentionally inflicted by other and 38.9% for self-inflicted injuries (p < 0.0001). When substances were used, the odds of intentional injuries were 7.5 times greater compared to non-intentional injuries (95% CI 6.7, 8.5). Burns, head injuries and polytraumas were more prevalent when drugs or alcohol were involved. Conclusion This study outlines the significant contribution of substance use in intentional injuries, suggesting that it could potentially be beneficial to specifically target patients who present with deliberate physical injuries in preventive and therapeutic interventions offered in the ED.
Keywords: emergency medicine; intentional injury; intoxication; self-harm; trauma.
Copyright © 2020, Michaud-Germain et al.
Conflict of interest statement
The authors have declared that no competing interests exist.
Figures
Similar articles
-
Sentinel surveillance of injuries and poisonings associated with cocaine and other substance use: results from the Canadian Hospitals Injury Reporting and Prevention Program (CHIRPP).Health Promot Chronic Dis Prev Can. 2022 Jul;42(7):263-271. doi: 10.24095/hpcdp.42.7.01. Health Promot Chronic Dis Prev Can. 2022. PMID: 35830216 Free PMC article.
-
Self-Inflicted Injury-Canadian Hospitals Injury Reporting and Prevention Program (CHIRPP-SI): a new surveillance tool for detecting self-inflicted injury events in emergency departments.Can J Public Health. 2019 Apr;110(2):244-252. doi: 10.17269/s41997-018-0139-1. Epub 2018 Oct 11. Can J Public Health. 2019. PMID: 30311176 Free PMC article.
-
Determining the accuracy of the Canadian Hospitals Injury Reporting and Prevention Program for the representation of the rates of mild traumatic brain injuries in Quebec.Health Promot Chronic Dis Prev Can. 2019 Nov;39(11):291-297. doi: 10.24095/hpcdp.39.11.01. Health Promot Chronic Dis Prev Can. 2019. PMID: 31729311 Free PMC article.
-
Self harm is an independent predictor of mortality in trauma and burns patients admitted to ICU.Injury. 2012 Sep;43(9):1562-5. doi: 10.1016/j.injury.2011.06.005. Epub 2011 Jun 28. Injury. 2012. PMID: 21714967 Review.
-
Intentional Self-inflicted Burn Injuries: Review of the Literature.Psychosomatics. 2017 Nov-Dec;58(6):581-591. doi: 10.1016/j.psym.2017.06.001. Epub 2017 Jun 13. Psychosomatics. 2017. PMID: 28760366 Review.
Cited by
-
Prevalence of Substance Abuse Among Trauma Patients in Rural West Virginia.Cureus. 2023 Mar 21;15(3):e36468. doi: 10.7759/cureus.36468. eCollection 2023 Mar. Cureus. 2023. PMID: 37090413 Free PMC article.
-
Sobering Overview of Traumatic Craniofacial Injuries Involving Drugs and Alcohol: A Comprehensive Analysis of the NEISS Database.Craniomaxillofac Trauma Reconstr. 2025 Feb 7;18(1):13. doi: 10.3390/cmtr18010013. eCollection 2025 Mar. Craniomaxillofac Trauma Reconstr. 2025. PMID: 40271459 Free PMC article.
-
Post-traumatic stress disorder (PTSD) symptoms and alcohol and drug use comorbidity at 25 US level I trauma centers.Trauma Surg Acute Care Open. 2022 Aug 4;7(1):e000913. doi: 10.1136/tsaco-2022-000913. eCollection 2022. Trauma Surg Acute Care Open. 2022. PMID: 35979039 Free PMC article.
-
Impact of substance-related harms on injury hospitalizations in Canada, from 2010 to 2020.Health Promot Chronic Dis Prev Can. 2023 Mar;43(3):130-138. doi: 10.24095/hpcdp.43.3.03. Health Promot Chronic Dis Prev Can. 2023. PMID: 36924466 Free PMC article.
-
Characteristics of Older Adults Attending the Emergency Department for Suicidal Thoughts or Voluntary Intoxication: A Multicenter Retrospective Cohort Study.Cureus. 2022 Oct 18;14(10):e30428. doi: 10.7759/cureus.30428. eCollection 2022 Oct. Cureus. 2022. PMID: 36407250 Free PMC article.
References
-
- Testing for substance use in trauma patients: are we doing enough? London JA, Battistella FD. Arch Surg. 2007;142:633–638. - PubMed
-
- Drug use. [Sep;2020 ];https://ourworldindata.org/substance-use 2019
-
- Alcohol use and injury risk in Thailand: a case-crossover emergency department study. Sornpaisarn B, Sornpaisarn S, Shield KD, Rehm J. Drug Alcohol Rev. 2020;39:539–545. - PubMed
-
- The association between illicit drug use and infectious complications among trauma patients. Agrawal V, Amos JD. Eur J Clin Microbiol Infect Dis. 2017;36:447–450. - PubMed
LinkOut - more resources
Full Text Sources