Geographic Variation in Racial Disparities in Health and Coronavirus Disease-2019 (COVID-19) Mortality
- PMID: 33043273
- PMCID: PMC7538135
- DOI: 10.1016/j.mayocpiqo.2020.09.005
Geographic Variation in Racial Disparities in Health and Coronavirus Disease-2019 (COVID-19) Mortality
Abstract
Objective: To evaluate the race-stratified state-level prevalence of health determinants and the racial disparities in coronavirus disease 2019 (COVID-19) cumulative incidence and mortality in the United States.
Patients and methods: The age-adjusted race-stratified prevalence of comorbidities (hypertension, diabetes, dyslipidemia, and obesity), preexisting medical conditions (pulmonary disease, heart disease, stroke, kidney disease, and malignant neoplasm), poor health behaviors (smoking, alcohol abuse, and physical inactivity), and adverse socioeconomic factors (education, household income, and health insurance) was computed in 435,139 American adult participants from the 2017 Behavioral Risk Factor Surveillance System survey. Correlation was assessed between health determinants and the race-stratified COVID-19 crude mortality rate and infection-fatality ratio computed from respective state public health departments in 47 states.
Results: Blacks had a higher prevalence of comorbidities (63.3%; 95% CI, 62.4% to 64.2% vs 55.1%; 95% CI, 54.7% to 55.5%) and adverse socioeconomic factors (47.0%; 95% CI, 46.0% to 47.9% vs 30.9%; 95% CI, 30.6% to 31.3%) than did whites. The prevalence of preexisting medical conditions was similar in blacks (30.4%; 95% CI, 28.8% to 32.1%) and whites (30.8%; 95% CI, 30.2% to 31.4%). The prevalence of poor health behaviors was higher in whites (57.2%; 95% CI, 56.3% to 58.0%) than in blacks (50.2%; 95% CI,46.2% to 54.2%). Comorbidities and adverse socioeconomic factors were highest in the southern region, and poor health behaviors were highest in the western region. The cumulative incidence rate (per 100,000 persons) was 3-fold higher in blacks (1546.4) than in whites (540.4). The crude mortality rate (per 100,000 persons) was 2-fold higher in blacks (83.2) than in whites (33.2). However, the infection-fatality ratio (per 100 cases) was similar in whites (6.2) and blacks (5.4). Within racial groups, the geographic distribution of health determinants did not correlate with the state-level COVID-19 mortality and infection-fatality ratio (P>.05 for all).
Conclusion: Racial disparities in COVID-19 are largely driven by the higher cumulative incidence of infection in blacks. There is a discordance between the geographic dispersion of COVID-19 mortality and the regional distribution of health determinants.
Keywords: BRFSS, Behavioral Risk Factor Surveillance System; COVID-19, coronavirus disease 2019; IFR, infection-fatality ratio.
Figures
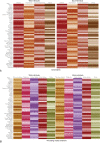





References
-
- Chowkwanyun M., Reed A.L., Jr. Racial health disparities and Covid-19—caution and context. N Engl J Med. 2020;383(3):201–203. - PubMed
-
- Yancy C.W. COVID-19 and African Americans. JAMA. 2020;323(19):1891–1892. - PubMed
-
- Health Equity Considerations and Racial and Ethnic Minority Groups Centers for Disease Control and Prevention website. https://www.cdc.gov/coronavirus/2019-ncov/community/health-equity/race-e...
Grants and funding
LinkOut - more resources
Full Text Sources

