Three‑Dimensional Ultrasonography in Preoperative and Postoperative Volume Assessment of the Undescended Testicle
- PMID: 33046685
- PMCID: PMC7568441
- DOI: 10.12659/MSM.924325
Three‑Dimensional Ultrasonography in Preoperative and Postoperative Volume Assessment of the Undescended Testicle
Abstract
BACKGROUND Ultrasound (US) is the preferred imaging method for cryptorchidism, but most guidelines indicate that its value is questionable. The aim of this study was to evaluate the clinical value of ultrasonic mobility and testicular atrophy index (TAI) based on three‑dimensional US (3DUS) in preoperative and postoperative assessment of the undescended testis. MATERIAL AND METHODS Data from 158 children with unilateral extraperitoneal cryptorchidism were collected and their diagnoses were surgically confirmed. They were divided into different age groups and into 2 ultrasonic mobility groups: the mobile group (MG) and the restricted group (RG). Differences in sonographic characteristics between different groups were compared. Three-dimensional ultrasound performed with virtual organ computer-aided analysis (VOCAL) was used to determined preoperative and postoperative TAI and the reliability of TAI was analyzed. RESULTS Measurement of testicular volume with the VOCAL method was significantly more reliable than that done with the two-dimensional Lambert method. In all age groups, preoperative testicular volumes were smaller than that in the contralateral scrotal testis and postoperatively, they increased steadily. Both preoperative and postoperative TAI were higher in the RG than in the MG. In the MG, postoperative TAI decreased significantly in all age groups. In the RG, in contrast, effective volume growth was only achieved in patients who had undergone surgery before they reached age 1 year. CONCLUSIONS TAI values determined with 3DUS using the VOCAL technique objectively reflect recovery of testicular volume following surgery for undescended testicle. Ultrasonic mobility evaluation is beneficial for clinical management of the condition.
Conflict of interest statement
None.
Figures
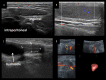
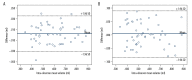
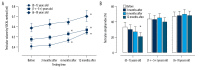

References
-
- Kim JK, Chua ME, Ming JM, et al. A critical review of recent clinical practice guidelines on management of cryptorchidism. J Pediatr Surg. 2018;53(10):2041–47. - PubMed
-
- Kolon TF, Herndon CD, Baker LA, et al. American Urological Association. Evaluation and treatment of cryptorchidism: AUA guideline. J Urol. 2014;192(2):337–45. - PubMed
-
- Shin HJ, Lee YS, Yoon H, et al. Testicular volume and elasticity changes in young children with undescended testes. Med Ultrason. 2017;19(4):380–85. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

