Aerosolisation during tracheal intubation and extubation in an operating theatre setting
- PMID: 33047327
- PMCID: PMC7675280
- DOI: 10.1111/anae.15301
Aerosolisation during tracheal intubation and extubation in an operating theatre setting
Abstract
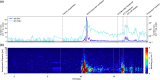
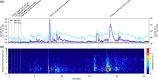
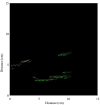
Aerosol-generating procedures such as tracheal intubation and extubation pose a potential risk to healthcare workers because of the possibility of airborne transmission of infection. Detailed characterisation of aerosol quantities, particle size and generating activities has been undertaken in a number of simulations but not in actual clinical practice. The aim of this study was to determine whether the processes of facemask ventilation, tracheal intubation and extubation generate aerosols in clinical practice, and to characterise any aerosols produced. In this observational study, patients scheduled to undergo elective endonasal pituitary surgery without symptoms of COVID-19 were recruited. Airway management including tracheal intubation and extubation was performed in a standard positive pressure operating room with aerosols detected using laser-based particle image velocimetry to detect larger particles, and spectrometry with continuous air sampling to detect smaller particles. A total of 482,960 data points were assessed for complete procedures in three patients. Facemask ventilation, tracheal tube insertion and cuff inflation generated small particles 30-300 times above background noise that remained suspended in airflows and spread from the patient's facial region throughout the confines of the operating theatre. Safe clinical practice of these procedures should reflect these particle profiles. This adds to data that inform decisions regarding the appropriate precautions to take in a real-world setting.
기관내 삽관 및 발관과 같은 에어로졸 생성 시술은 공기매 개 전파의 가능성이 있으므로 의료 종사자에게 잠재적 위험 을 초래할 수 있다. 에어로졸의 양, 입자 크기 및 생성 활동에 대한 자세한 특성 분석이 다수의 모의상황에서 수행되었으나, 실제 임상에서는 수행되지 않았다. 본 연구의 목적은 마스크 환기, 기관내 삽관 및 발관 과정이 임상에서 에어로졸을 생성 하는지 여부를 파악하고 생성된 모든 에어로졸의 특성을 분석 하는 것이었다. 본 관찰 연구에서는 코로나‐19의 증상이 없으 며 경비강 접근법을 이용한 선택적 뇌하수체 수술을 받을 예 정이었던 환자를 모집하였다. 기관내 삽관 및 발관을 포함한 기도 관리는 에어로졸이 검출된 표준 양압 수술실에서 수행되 었다. 레이저 기반 입자영상유속계를 사용하여 크기가 큰 입 자를 검출하였으며, 연속식 공기 샘플링을 이용한 분광분석법 으로 작은 크기의 입자를 검출하였다. 3명의 환자를 대상으로 전체 시술에 대해 총 482,960개의 데이터 포인트를 평가하였 다. 마스크 환기, 기관내 튜브 삽입 및 커프 팽창은 기류에 부 유하는 배경 노이즈를 30‐300배 초과하는 작은 입자를 생성 하였으며, 환자의 안면부로부터 수술실 영역 전체로 확산되었 다. 이러한 시술의 안전한 임상 진료 지침에는 이와 같은 입자 프로파일을 반영해야 한다. 이는 실제 환경에 적합한 예방조 치와 관련된 의사결정 정보를 제공하는 데이터에 추가된다.
Keywords: aerosol-generating procedures; extubation; intubation; occupational exposure.
© 2020 Association of Anaesthetists.
Figures

Comment in
-
Are tracheal intubation and extubation aerosol-generating procedures?Anaesthesia. 2021 Feb;76(2):151-155. doi: 10.1111/anae.15328. Epub 2020 Dec 4. Anaesthesia. 2021. PMID: 33274761 Free PMC article. No abstract available.
-
Reconciling aerosol generation data with actual rates of infection data.Anaesthesia. 2021 Mar;76 Suppl 3:27-28. doi: 10.1111/anae.15330. Epub 2020 Dec 6. Anaesthesia. 2021. PMID: 33280082 No abstract available.
Similar articles
-
A quantitative evaluation of aerosol generation during tracheal intubation and extubation.Anaesthesia. 2021 Feb;76(2):174-181. doi: 10.1111/anae.15292. Epub 2020 Oct 22. Anaesthesia. 2021. PMID: 33022093 Free PMC article.
-
Aerosolisation in endonasal endoscopic pituitary surgery.Pituitary. 2021 Aug;24(4):499-506. doi: 10.1007/s11102-021-01125-8. Epub 2021 Jan 19. Pituitary. 2021. PMID: 33469830 Free PMC article.
-
Quantitative evaluation of aerosol generation from upper airway suctioning assessed during tracheal intubation and extubation sequences in anaesthetized patients.J Hosp Infect. 2022 Jun;124:13-21. doi: 10.1016/j.jhin.2022.02.021. Epub 2022 Mar 9. J Hosp Infect. 2022. PMID: 35276282 Free PMC article.
-
Difficult Airway Management in Adult Coronavirus Disease 2019 Patients: Statement by the Society of Airway Management.Anesth Analg. 2021 Oct 1;133(4):876-890. doi: 10.1213/ANE.0000000000005554. Anesth Analg. 2021. PMID: 33711004 Review.
-
Could "safe practice" be compromising safe practice? Should anesthetists have to deflate the cuff of the endotracheal tube before extubation?Minerva Anestesiol. 2016 Feb;82(2):236-9. Epub 2015 Jul 1. Minerva Anestesiol. 2016. PMID: 26126979 Review.
Cited by
-
Impact of the Coronavirus Pandemic on Patients Requiring Tracheal Intubation by Helicopter Emergency Medical Services: A Retrospective, Single-Center, Observational Study.J Clin Med. 2024 Jun 25;13(13):3694. doi: 10.3390/jcm13133694. J Clin Med. 2024. PMID: 38999261 Free PMC article.
-
Effects of wearing surgical masks on fraction of inspired oxygen in spontaneously breathing patients: improving safety for frontline healthcare professionals under pandemic situations.BMC Anesthesiol. 2022 Apr 18;22(1):108. doi: 10.1186/s12871-022-01649-x. BMC Anesthesiol. 2022. PMID: 35436860 Free PMC article.
-
Human Factors and Airway Management in COVID-19 Patients: The Perfect Storm?J Clin Med. 2022 Jul 22;11(15):4271. doi: 10.3390/jcm11154271. J Clin Med. 2022. PMID: 35893372 Free PMC article.
-
Aerosol generation during general anesthesia is comparable to coughing: An observational clinical study.Acta Anaesthesiol Scand. 2022 Apr;66(4):463-472. doi: 10.1111/aas.14022. Epub 2022 Jan 11. Acta Anaesthesiol Scand. 2022. PMID: 34951703 Free PMC article.
-
The role of airborne particles and environmental considerations in the transmission of SARS-CoV-2.Geosci Front. 2021 Sep;12(5):101189. doi: 10.1016/j.gsf.2021.101189. Epub 2021 Apr 5. Geosci Front. 2021. PMID: 38620834 Free PMC article. Review.
References
-
- Cook TM. Personal protective equipment during the coronavirus disease (COVID) 2019 pandemic – a narrative review. Anaesthesia 2020; 75: 920–7. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources

