Innovative use of contegra valved conduit in left iliocaval stent thrombosis
- PMID: 33060901
- PMCID: PMC7525597
- DOI: 10.1007/s12055-017-0593-z
Innovative use of contegra valved conduit in left iliocaval stent thrombosis
Abstract
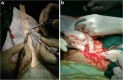
Thrombosis of an iliofemoral vein accounts for 25% of all lower extremity deep vein thrombosis (DVT) and is associated with an increased risk of pulmonary embolism (PE), limb malperfusion, and post-thrombotic syndrome (PTS). Endothelial injury, hypercoagulability and stasis constitute Virchow's triad of thrombogenesis. Common predisposing conditions include the postoperative state, prolonged immobility (e.g., travel, hospitalization), malignancy, pregnancy, and inherited hypercoagulable conditions. Long-term complications of DVT include persistent lower extremity edema, venous claudication, hyperpigmentation, and ulceration-collectively called as PTS and are associated with a reduced quality of life with increased health care expenses. The indications for open surgical revascularization are rare and usually reserved for patients whose symptoms are refractory to anticoagulation and endovascular treatment. Here, we report a successful decompression of severe venous edema of left lower limb post left iliocaval stent thrombosis in a 50-year-old female patient. We used two contegra valved conduits which were sutured end to end with each other in the same direction as a bypass graft. Proximal end of the conduit was anastomosed to left common femoral vein and the distal end to the distal inferior vena cava (IVC). It provided prompt and effective venous outflow with complete resolution of the venous edema of left lower limb. computed tomography (CT) venogram done after 3 months of surgery showed patent contegra valved conduit with thrombosed iliocaval stent.
Keywords: Contegra valved conduit; PE-Pulmonary embolism; PTS-Post thrombotic syndrome.
© Indian Association of Cardiovascular-Thoracic Surgeons 2017.
Conflict of interest statement
Conflict of interestThe authors declare that they have no conflict of interest.
Figures


References
-
- Plate G, Hollier LH, Gloviczki P, Dewanjee MK, Kaye MP. Overcoming failure of venous vascular prosthesis. Surg. 1984;96:503–510. - PubMed
Publication types
LinkOut - more resources
Full Text Sources
