Prevalence of Antibiotic-Resistant Pulmonary Tuberculosis in Bangladesh: A Systematic Review and Meta-Analysis
- PMID: 33080862
- PMCID: PMC7602942
- DOI: 10.3390/antibiotics9100710
Prevalence of Antibiotic-Resistant Pulmonary Tuberculosis in Bangladesh: A Systematic Review and Meta-Analysis
Abstract
Resistance to anti-tuberculosis (anti-TB) antibiotics is a major public health concern for many high-TB burden countries in Asia, including Bangladesh. Therefore, to represent the overall drug-resistance pattern against TB in Bangladesh, a systematic review and meta-analysis was conducted. Databases such as PubMed, Scopus, and Google Scholar were searched to identify studies related to antibiotic-resistant TB. A total of 24 studies covering 13,336 patients with TB were secured and included. The random-effects model was used to calculate the summary estimates. The pooled prevalence of any, mono, multi, poly, and extensive anti-TB antibiotic-resistances were 45.3% [95% CI: 33.5-57.1], 14.3% [95% CI: 11.4-17.2], 22.2% [95% CI: 18.8-25.7], 7.7% [95% CI: 5.6-9.7], and 0.3% [95% CI: 0.0-1.0], respectively. Among any first and second-line anti-TB drugs, isoniazid (35.0%) and cycloserine (44.6%) resistances were the highest, followed by ethambutol (16.2%) and gatifloxacin (0.2%). Any, multi, and poly drug-resistances were higher in retreatment cases compared to the newly diagnosed cases, although mono drug-resistance tended to be higher in newly diagnosed cases (15.7%) than that in retreatment cases (12.5%). The majority (82.6%) of the included studies were of high quality, with most not exhibiting publication bias. Sensitivity analyses confirmed that all outcomes are robust and reliable. It is concluded that resistance to anti-TB drugs in Bangladesh is rampant and fast growing. Therefore, the implementation of a nationwide surveillance system to detect suspected and drug-resistant TB cases, as well as to ensure a more encompassing treatment management by national TB control program, is highly recommended.
Keywords: Bangladesh; antibiotic resistance; epidemiology; meta-analysis; prevalence; pulmonary tuberculosis; systematic review.
Conflict of interest statement
The authors declare no conflict of interest.
Figures

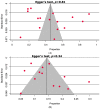



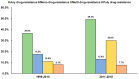
References
-
- WHO . Global Tuberculosis Report 2019. WHO; Geneva, Switzerland: 2019.
-
- Khatun U.F., Amin R., Islam M., Rob A., Rahim A. Socio-demographic Profile and Drug Sensitivity Pattern of Suspected Drug Resistant Tuberculosis among Patients in Regional Tuberculosis Reference Laboratory (RTRL) of a Tertiary Hospital. J. Med. 2017;18:62–67. doi: 10.3329/jom.v18i2.33680. - DOI
-
- Heysell S.K., Ahmed S., Ferdous S.S., Khan M.S.R., Rahman S.M., Gratz J., Rahman M.T., Mahmud A.M., Houpt E.R., Banu S. Quantitative drug-susceptibility in patients treated for multidrug-resistant tuberculosis in Bangladesh: Implications for regimen choice. PLoS ONE. 2015;10:e0116795. doi: 10.1371/journal.pone.0116795. - DOI - PMC - PubMed
-
- Ahuja S.D., Ashkin D., Avendano M., Banerjee R., Bauer M., Bayona J.N., Becerra M.C., Benedetti A., Burgos M., Centis R. Multidrug resistant pulmonary tuberculosis treatment regimens and patient outcomes: An individual patient data meta-analysis of 9,153 patients. PLoS Med. 2012;9:e1001300. doi: 10.1371/annotation/230240bc-bcf3-46b2-9b21-2e6e584f7333. - DOI - PMC - PubMed
LinkOut - more resources
Full Text Sources

