Time between Symptom Onset, Hospitalisation and Recovery or Death: Statistical Analysis of Belgian COVID-19 Patients
- PMID: 33080869
- PMCID: PMC7589278
- DOI: 10.3390/ijerph17207560
Time between Symptom Onset, Hospitalisation and Recovery or Death: Statistical Analysis of Belgian COVID-19 Patients
Abstract
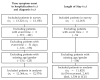
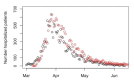
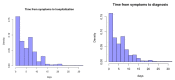
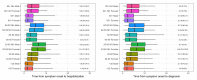
There are different patterns in the COVID-19 outbreak in the general population and amongst nursing home patients. We investigate the time from symptom onset to diagnosis and hospitalization or the length of stay (LoS) in the hospital, and whether there are differences in the population. Sciensano collected information on 14,618 hospitalized patients with COVID-19 admissions from 114 Belgian hospitals between 14 March and 12 June 2020. The distributions of different event times for different patient groups are estimated accounting for interval censoring and right truncation of the time intervals. The time between symptom onset and hospitalization or diagnosis are similar, with median length between symptom onset and hospitalization ranging between 3 and 10.4 days, depending on the age of the patient (longest delay in age group 20-60 years) and whether or not the patient lives in a nursing home (additional 2 days for patients from nursing home). The median LoS in hospital varies between 3 and 10.4 days, with the LoS increasing with age. The hospital LoS for patients that recover is shorter for patients living in a nursing home, but the time to death is longer for these patients. Over the course of the first wave, the LoS has decreased.
Keywords: COVID-19; length of stay in hospital; symptom onset to hospitalization; truncation and interval-censoring.
Conflict of interest statement
The authors declare no conflict of interest. The funders had no role in the design of the study; in the collection, analyses, or interpretation of data; in the writing of the manuscript, or in the decision to publish the results.
Figures



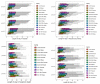


References
-
- Vekaria B., Overton C.E., Wisniowski A., Ahmad S.H., Aparicio-Castro A., Curran-Sebastian J., Eddleston J., Hanley N.A., House T., Kim J., et al. Hospital length of stay for COVID-19 patients: Data-driven methods for forward planning. MedRXiv. 2020 doi: 10.21203/rs.3.rs-56855/v1. - DOI - PMC - PubMed
-
- Donnely C.A., Ghani A.C., Leung G.M., Hedley A.J., Fraser C., Riley S., Abu-Raddad L.J., Ho L.M., Thach T.Q., Chau P. Epidemiological determinants of spread of causal agent of severe acute respiratory syndrom in Hong Kong. Lancet. 2003;361:1761–1766. doi: 10.1016/S0140-6736(03)13410-1. - DOI - PMC - PubMed
-
- Held L., Hens N., O’Neill P., Wallinga J. Handbook of Infectious Diseases Data Analysis. Chapman & Hall/CRC; Boca Raton, FL, USA: 2020.
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources

