Use of In Situ Simulation to Improve Emergency Department Readiness for the COVID-19 Pandemic
- PMID: 33081859
- PMCID: PMC7653231
- DOI: 10.1017/S1049023X2000134X
Use of In Situ Simulation to Improve Emergency Department Readiness for the COVID-19 Pandemic
Abstract
Introduction: During the world-wide coronavirus disease 2019 (COVID-19) outbreak, there is an urgent need to rapidly increase the readiness of hospitals. Emergency departments (EDs) are at high risk of facing unusual situations and need to prepare extensively in order to minimize risks to health care providers (HCPs) and patients. In situ simulation is a well-known method used in training to detect system gaps that could threaten safety.
Study objectives: One objective is to identify gaps, test hospital systems, and inform necessary modifications to the standard processes required by patients with COVID-19 presenting at the hospital. The other objective is to improve ED staff confidence in managing such patients, and to increase their skills in basic and advanced airway management and proper personal protective equipment (PPE) techniques.
Methods: This is a quasi-experimental study in which 20 unannounced mock codes were carried out in ED resuscitation and isolation rooms. A checklist was designed, validated, and used to evaluate team performances in three areas: donning, basic and advanced airway skills, and doffing. A pre- and post-intervention survey was used to evaluate staff members' perceived knowledge of ED procedures related to COVID-19 and their airway management skills.
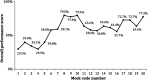
Results: A total of 20 mock codes were conducted in the ED. Overall, 16 issues that posed potential harm to staff or patients were identified and prioritized for immediate resolution. Approximately 57.4% of HCPs felt comfortable dealing with suspected/confirmed, unstable COVID-19 cases after mock codes, compared with 33.3% beforehand (P = .033). Of ED HCPs, 44.4% felt comfortable performing airway procedures for suspected/confirmed COVID-19 cases after mock codes compared with 29.6% beforehand. Performance of different skills was observed to be variable following the 20 mock codes. Skills with improved performance included: request of chest x-ray after intubation (88.0%), intubation done by the most experienced ED physician (84.5%), and correct sequence and procedure of PPE (79.0%).
Conclusion: Mock codes identified significant defects, most of which were easily fixed. They included critical equipment availability, transporting beds that were too large to fit through doors, and location of biohazard bins. Repeated mock codes improved ED staff confidence in dealing with patients, in addition to performance of certain skills. In situ simulation proves to be an effective method for increasing the readiness of the ED to address the COVID-19 pandemic and other infection outbreaks.
Keywords: COVID-19; emergency department; mock codes; simulation.
Figures

References
-
- Neher RA, Dyrdak R, Druelle V, et al. Potential impact of seasonal forcing on a SARS-CoV-2 pandemic. Swiss Medical Weekly. 2020;150:w20224. - PubMed
-
- Fregene TE, Nadarajah P, Buckley JF, et al. Use of in situ simulation to evaluate the operational readiness of a high-consequence infectious disease intensive care unit. Anaesthesia. 2020;75(6):733-738. - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

