Transjugular intrahepatic portosystemic shunt in cirrhosis: An exhaustive critical update
- PMID: 33088154
- PMCID: PMC7545393
- DOI: 10.3748/wjg.v26.i37.5561
Transjugular intrahepatic portosystemic shunt in cirrhosis: An exhaustive critical update
Abstract
More than five decades after it was originally conceptualized as rescue therapy for patients with intractable variceal bleeding, the transjugular intrahepatic portosystemic shunt (TIPS) procedure continues to remain a focus of intense clinical and biomedical research. By the impressive reduction in portal pressure achieved by this intervention, coupled with its minimally invasive nature, TIPS has gained increasing acceptance in the treatment of complications of portal hypertension. The early years of TIPS were plagued by poor long-term patency of the stents and increased incidence of hepatic encephalopathy. Moreover, the diversion of portal flow after placement of TIPS often resulted in derangement of hepatic functions, which was occasionally severe. While the incidence of shunt dysfunction has markedly reduced with the advent of covered stents, hepatic encephalopathy and instances of early liver failure continue to remain a significant issue after TIPS. It has emerged over the years that careful selection of patients and diligent post-procedural care is of paramount importance to optimize the outcome after TIPS. The past twenty years have seen multiple studies redefining the role of TIPS in the management of variceal bleeding and refractory ascites while exploring its application in other complications of cirrhosis like hepatic hydrothorax, portal hypertensive gastropathy, ectopic varices, hepatorenal and hepatopulmonary syndromes, non-tumoral portal vein thrombosis and chylous ascites. It has also been utilized to good effect before extrahepatic abdominal surgery to reduce perioperative morbidity and mortality. The current article aims to review the updated literature on the status of TIPS in the management of patients with liver cirrhosis.
Keywords: Early transjugular portosystemic shunt; Esophageal varices; Gastric varices; Portal hypertension; Preemptive transjugular intrahepatic portosystemic shunt; Refractory ascites.
©The Author(s) 2020. Published by Baishideng Publishing Group Inc. All rights reserved.
Conflict of interest statement
Conflict-of-interest statement: None to declare.
Figures

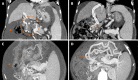
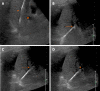
References
-
- Rösch J, Hanafee WN, Snow H. Transjugular portal venography and radiologic portacaval shunt: an experimental study. Radiology. 1969;92:1112–1114. - PubMed
-
- Palmaz JC, Garcia F, Sibbitt RR, Tio FO, Kopp DT, Schwesinger W, Lancaster JL, Chang P. Expandable intrahepatic portacaval shunt stents in dogs with chronic portal hypertension. AJR Am J Roentgenol. 1986;147:1251–1254. - PubMed
-
- García-Pagán JC, Caca K, Bureau C, Laleman W, Appenrodt B, Luca A, Abraldes JG, Nevens F, Vinel JP, Mössner J, Bosch J Early TIPS (Transjugular Intrahepatic Portosystemic Shunt) Cooperative Study Group. Early use of TIPS in patients with cirrhosis and variceal bleeding. N Engl J Med. 2010;362:2370–2379. - PubMed
-
- Miraglia R, Maruzzelli L, Di Piazza A, Mamone G, Caruso S, Gentile G, Tuzzolino F, Floridia G, Petridis I, Volpes R, Luca A. Transjugular Intrahepatic Portosystemic Shunt Using the New Gore Viatorr Controlled Expansion Endoprosthesis: Prospective, Single-Center, Preliminary Experience. Cardiovasc Intervent Radiol. 2019;42:78–86. - PubMed
-
- Coronado WM, Ju C, Bullen J, Kapoor B. Predictors of Occurrence and Risk of Hepatic Encephalopathy After TIPS Creation: A 15-Year Experience. Cardiovasc Intervent Radiol. 2020;43:1156–1164. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Miscellaneous

