Consumption of Foods Derived from Subsidized Crops Remains Associated with Cardiometabolic Risk: An Update on the Evidence Using the National Health and Nutrition Examination Survey 2009-2014
- PMID: 33113961
- PMCID: PMC7690710
- DOI: 10.3390/nu12113244
Consumption of Foods Derived from Subsidized Crops Remains Associated with Cardiometabolic Risk: An Update on the Evidence Using the National Health and Nutrition Examination Survey 2009-2014
Abstract
In this study, we examined the associations between the consumption of foods derived from crops subsidized under the 2008 United States (US) Farm Bill and cardiometabolic risk factors and whether the magnitude of these associations has changed since the 2002 US Farm Bill. Four federal databases were used to estimate daily consumption of the top seven subsidized commodities (corn, soybeans, wheat, rice, sorghum, dairy, and livestock) and to calculate a subsidy score (0-1 scale) for Americans' daily dietary intake during 2009-2014, with a higher score indicative of a higher proportion of the diet derived from subsidized commodities. The cardiometabolic risk factors included obesity, abdominal adiposity, hypertension, dyslipidemia, and dysglycemia. Linear and logistic regression models were adjusted for age, sex, race/ethnicity, the poverty-income ratio, the smoking status, educational attainment, physical activity, and daily calorie intake. During 2009-2014, adults with the highest subsidy score had higher probabilities of obesity, abdominal adiposity, and dysglycemia compared to the lowest subsidy score. After the 2002 Farm Bill (measured using data from 2001-2006), the subsidy score decreased from 56% to 50% and associations between consuming a highly-subsidized diet and dysglycemia did not change (p = 0.54), whereas associations with obesity (p = 0.004) and abdominal adiposity (p = 0.002) significantly attenuated by more than half. The proportion of calories derived from subsidized food commodities continues to be associated with adverse cardiometabolic risk factors, though the relationship with obesity and abdominal adiposity has weakened in recent years.
Keywords: cardiometabolic disease; farm subsidies; food policy; obesity.
Conflict of interest statement
The authors declare no conflict of interest.
Figures
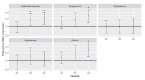

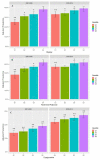
References
-
- Hales C., Carroll M., Fryar C., Ogden C. Prevalence of Obesity and Severe Obesity Among Adults: United States, 2017–2018. National Center for Health Statistics; Hyattsville, MD, USA: 2020. (NCHS Data Brief n. 360). - PubMed
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

