Perinatal Arterial Ischemic Stroke in Fetal Vascular Malperfusion: A Case Series and Literature Review
- PMID: 33122209
- PMCID: PMC7963247
- DOI: 10.3174/ajnr.A6857
Perinatal Arterial Ischemic Stroke in Fetal Vascular Malperfusion: A Case Series and Literature Review
Abstract
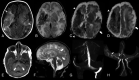
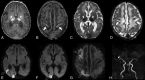
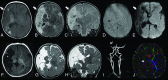
Fetal vascular malperfusion includes a continuum of placental histologic abnormalities increasingly associated with perinatal brain injury, namely arterial ischemic stroke. Here, we describe the clinical-neuroimaging features of 5 neonates with arterial ischemic stroke and histologically proved fetal vascular malperfusion. All infarcts involved the anterior territories and were multiple in 2 patients. In 2 neonates, there were additional signs of marked dural sinus congestion, thrombosis, or both. A mixed pattern of chronic hypoxic-ischemic encephalopathy and acute infarcts was noted in 1 patient at birth. Systemic cardiac or thrombotic complications were present in 2 patients. These peculiar clinical-radiologic patterns may suggest fetal vascular malperfusion and should raise the suspicion of this rare, underdiagnosed condition carrying important implications in patient management, medicolegal actions, and future pregnancy counseling.
© 2020 by American Journal of Neuroradiology.
Figures

References
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
