Central Nervous System Manifestations Associated with COVID-19
- PMID: 33128130
- PMCID: PMC7599061
- DOI: 10.1007/s11910-020-01079-7
Central Nervous System Manifestations Associated with COVID-19
Erratum in
-
Correction to: Central Nervous System Manifestations Associated with COVID-19.Curr Neurol Neurosci Rep. 2020 Nov 12;20(12):66. doi: 10.1007/s11910-020-01086-8. Curr Neurol Neurosci Rep. 2020. PMID: 33184674 Free PMC article.
Abstract
Purpose of review: Coronavirus disease 2019 (COVID-19) has become a global health crisis of our time. The disease arises from severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) that binds to angiotensin-converting enzyme 2 (ACE2) receptors on host cells for its internalization. COVID-19 has a wide range of respiratory symptoms from mild to severe and affects several other organs, increasing the complexity of the treatment. There is accumulating evidence to suggest that SARS-CoV-2 can target the nervous system. In this review, we provide an account of the COVID-19 central nervous system (CNS) manifestations.
Recent findings: A broad spectrum of the CNS manifestations including headache, impaired consciousness, delirium, loss of smell and taste, encephalitis, seizures, strokes, myelitis, acute disseminated encephalomyelitis, neurogenic respiratory failure, encephalopathy, silent hypoxemia, generalized myoclonus, neuroleptic malignant syndrome and Kawasaki syndrome has been reported in patients with COVID-19. CNS manifestations associated with COVID-19 should be considered in clinical practice. There is a need for modification of current protocols and standing orders to provide better care for COVID-19 patients presenting with neurological symptoms.
Keywords: CNS manifestations; COVID-19; Neurological manifestations; Pandemic; SARS-CoV-2; Stroke.
Conflict of interest statement
Afshin A. Divani, Sasan Andalib, José Biller, Mario Di Napoli, Narges Moghimi, Clio A. Rubinos, Christa O’Hana Nobleza, P.N Sylaja, Michel Toledano, Simona Lattanzi, Louise D McCullough, Salvador Cruz-Flores, Michel Torbey, and M. Reza Azarpazhooh each declare no potential conflicts of interest.
Figures
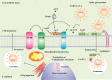
References
-
- WHO. Coronavirus (COVID-19). 2020. https://covid19.who.int/. Accessed August 26 2020.
-
- Arabi YM, Harthi A, Hussein J, Bouchama A, Johani S, Hajeer AH, Saeed BT, Wahbi A, Saedy A, AlDabbagh T, Okaili R, Sadat M, Balkhy H. Severe neurologic syndrome associated with Middle East respiratory syndrome corona virus (MERS-CoV) Infection. 2015;43(4):495–501. doi: 10.1007/s15010-015-0720-y. - DOI - PMC - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Research Materials
Miscellaneous

