Impact of Ophthalmic Viscosurgical Devices in Cataract Surgery
- PMID: 33133677
- PMCID: PMC7593745
- DOI: 10.1155/2020/7801093
Impact of Ophthalmic Viscosurgical Devices in Cataract Surgery
Abstract
Background: Ophthalmic viscoelastic devices (OVDs) used during small-incision cataract surgery have numerous advantages. However, OVDs have longer retention time in an eye after surgery resulting in intraocular pressure (IOP) spikes. The purpose of this study is to analyze and quantify the effect of various OVDs on both IOP and best corrected visual acuity (BCVA) by systematically reviewing the literature and performing meta-analysis.
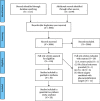
Methods: Numerous databases from January 1, 1985, to present were systematically searched. Thirty-six (3893 subjects) of 3313 studies identified were included for analysis. Standardized mean difference (SMD) was computed, and meta-analysis was performed.
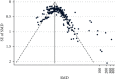
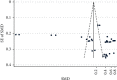
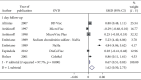
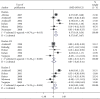
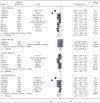
Results: A total of 3313 records were retrieved including 1114 from database search and 2199 from grey literature search. Significant increase in postoperative IOP in 1-day follow-up with Healon (SMD = 0.37, CI: [0.07, 0.67]), Viscoat (SMD = 0.29, CI: [0.13, 0.45]), Provisc (SMD = 0.46, CI: [0.17, 0.76]), and Soft Shell (SMD = 0.58, CI: [0.30, 0.86]) was computed. On the other hand, results implied a nonsignificant increase in postoperative IOP with Healon GV (SMD = 0.07, CI: [-0.28, 0.41]), Healon5 (SMD = 0.15, CI: [-0.33, 0.64]), 2% HPMC (SMD = 0.32, CI: [-0.0, 0.64]), and OcuCoat (SMD = 0.26, CI: [-0.37, 0.9]). Additionally, a nonsignificant reduction in postoperative IOP was inferred with Viscoat + Provisc (SMD = -0.28, CI: [-2.23, 1.68]).
Conclusion: Improvement in IOP was shown with Viscoat + Provisc. Additionally, IOP nonsignificant upsurge was observed with Healon GV, Healon5, 2% HPMC, and OcuCoat compared to significant upsurge with Healon, Viscoat, and Soft Shell.
Copyright © 2020 Monali S. Malvankar-Mehta et al.
Conflict of interest statement
The authors declare that there are no conflicts of interest regarding the publication of this paper.
Figures










Similar articles
-
Corneal Outcomes Following Cataract Surgery Using Ophthalmic Viscosurgical Devices Composed of Chondroitin Sulfate-Hyaluronic Acid: A Systematic Review and Meta-Analysis.Clin Ophthalmol. 2023 Jul 24;17:2083-2096. doi: 10.2147/OPTH.S419863. eCollection 2023. Clin Ophthalmol. 2023. PMID: 37521151 Free PMC article. Review.
-
Intraocular pressure after bilateral cataract surgery using Healon, Healon5, and Healon GV.J Cataract Refract Surg. 2002 Apr;28(4):617-25. doi: 10.1016/s0886-3350(01)01262-7. J Cataract Refract Surg. 2002. PMID: 11955901 Clinical Trial.
-
Preclinical Safety Evaluation of Ophthalmic Viscosurgical Devices in Rabbits and a Novel Mini-Pig Model.Ophthalmol Ther. 2019 Mar;8(1):101-114. doi: 10.1007/s40123-019-0167-9. Epub 2019 Feb 18. Ophthalmol Ther. 2019. PMID: 30778776 Free PMC article.
-
Intraocular pressure development in the rabbit eye after aqueous exchange with ophthalmic viscosurgical devices.J Cataract Refract Surg. 2000 Aug;26(8):1247-52. doi: 10.1016/s0886-3350(00)00407-7. J Cataract Refract Surg. 2000. PMID: 11008057
-
iStent as a Solo Procedure for Glaucoma Patients: A Systematic Review and Meta-Analysis.PLoS One. 2015 May 27;10(5):e0128146. doi: 10.1371/journal.pone.0128146. eCollection 2015. PLoS One. 2015. PMID: 26018579 Free PMC article.
Cited by
-
Advantages of Hyaluronic Acid and Its Combination with Other Bioactive Ingredients in Cosmeceuticals.Molecules. 2021 Jul 22;26(15):4429. doi: 10.3390/molecules26154429. Molecules. 2021. PMID: 34361586 Free PMC article. Review.
-
Narrative review after post-hoc trial analysis of factors that predict corneal endothelial cell loss after phacoemulsification: Tips for improving cataract surgery research.PLoS One. 2024 Mar 21;19(3):e0298795. doi: 10.1371/journal.pone.0298795. eCollection 2024. PLoS One. 2024. PMID: 38512953 Free PMC article. Review.
-
Elevated Intraocular Pressure Immediately after Cataract Surgery and Future Risk of Primary Open-Angle Glaucoma in the IRIS® Registry (Intelligent Research in Sight).Ophthalmol Sci. 2025 Jun 11;5(6):100851. doi: 10.1016/j.xops.2025.100851. eCollection 2025 Nov-Dec. Ophthalmol Sci. 2025. PMID: 40727324 Free PMC article.
-
Physical Characteristics, Clinical Application, and Side Effects of Viscoelastics in Ophthalmology.J Curr Ophthalmol. 2024 Aug 10;35(4):313-319. doi: 10.4103/joco.joco_178_23. eCollection 2023 Oct-Dec. J Curr Ophthalmol. 2024. PMID: 39281404 Free PMC article. Review.
-
Corneal Outcomes Following Cataract Surgery Using Ophthalmic Viscosurgical Devices Composed of Chondroitin Sulfate-Hyaluronic Acid: A Systematic Review and Meta-Analysis.Clin Ophthalmol. 2023 Jul 24;17:2083-2096. doi: 10.2147/OPTH.S419863. eCollection 2023. Clin Ophthalmol. 2023. PMID: 37521151 Free PMC article. Review.
References
Publication types
LinkOut - more resources
Full Text Sources

