Deep Vein Thrombosis Secondary to Extrinsic Compression: A Case Report
- PMID: 33133798
- PMCID: PMC7586351
- DOI: 10.7759/cureus.11160
Deep Vein Thrombosis Secondary to Extrinsic Compression: A Case Report
Abstract
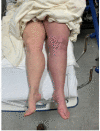
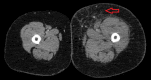
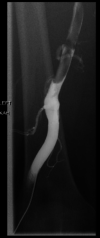
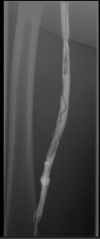
May-Thurner syndrome (MTS) is defined as extrinsic venous compression by the arteries of the iliocaval system. The most common manifestation of MTS is compression of the left common iliac vein by the right common iliac artery. May-Thurner syndrome is pathologically seen in 2%-5% of patients presenting with symptomatic deep vein thrombosis (DVT). As an anatomic variant, the prevalence is predicted to be much higher as most patients with MTS anatomy are asymptomatic and do not seek evaluation. Symptomatic clinical presentations can include left lower extremity pain, swelling, skin discoloration, ulceration, and venous claudication. Here we present a patient with symptomatic MTS. A 64-year-old female with no pertinent past medical history presented with complaint of worsening left lower extremity swelling and pain. Clinical picture was concerning for phlegmasia cerulea dolens and ultrasound was bypassed in favor of a CT scan of the lower extremities bilaterally. The CT showed occlusion of the deep veins of the left leg secondary to stenosis of the left common iliac vein just posterior to the right common iliac artery; a finding consistent with MTS. Interventional radiology performed a catheter-directed thrombolysis with stenting of the left common iliac and external iliac veins. The patient clinically improved and was discharged with anticoagulative therapy. May-Thurner syndrome is a condition that typically manifests due to external anatomic compression of the left common iliac vein. It is our belief that patients (with the appropriate risk factors) presenting with signs and symptoms consistent with proximal lower extremity DVT would benefit from further radiographic studies to fully evaluate for iliocaval venous stenosis and subsequent catheter-directed thrombolysis with endovascular stenting.
Keywords: deep vein thrombosis (dvt); endovascular catheter-directed thrombolysis; endovascular stenting; interventional radiology; may-thurner's syndrome.
Copyright © 2020, Singh et al.
Conflict of interest statement
The authors have declared that no competing interests exist.
Figures
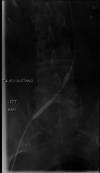
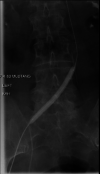
Similar articles
-
Magnetic resonance venography in the diagnosis and management of May-Thurner syndrome.Vasc Endovascular Surg. 2002 Jan-Feb;36(1):51-7. doi: 10.1177/153857440203600109. Vasc Endovascular Surg. 2002. PMID: 12704525
-
Nonnegligible causes of symptoms of acute lower extremities--3 cases of May-Thurner syndrome with deep vein thrombosis.Thromb J. 2021 Apr 19;19(1):25. doi: 10.1186/s12959-021-00278-7. Thromb J. 2021. PMID: 33874947 Free PMC article.
-
Surgical Thrombectomy, Fibrinolysis, Angioplasty and Stenting: A Combined Approach for Treatment of a May-Thurner Syndrome Presenting as Phlegmasia Cerulea Dolens.Rev Port Cir Cardiotorac Vasc. 2017 Jul-Dec;24(3-4):188. Rev Port Cir Cardiotorac Vasc. 2017. PMID: 29701417
-
Treatment of May-Thurner syndrome with catheter-directed thrombolysis and stent placement, complicated by heparin-induced thrombocytopenia.Cardiovasc Surg. 1998 Dec;6(6):607-13. doi: 10.1016/s0967-2109(98)00086-6. Cardiovasc Surg. 1998. PMID: 10395265 Review.
-
May-Thurner syndrome and other obstructive iliac vein lesions: meaning, myth, and mystery.Vasc Med. 2015 Feb;20(1):74-83. doi: 10.1177/1358863X14560429. Epub 2014 Dec 10. Vasc Med. 2015. PMID: 25502563 Review.
Cited by
-
Iliac vein compression syndrome by lumbar degenerative changes is associated with deep vein thrombosis after total knee arthroplasty.Arch Orthop Trauma Surg. 2023 Sep;143(9):5833-5842. doi: 10.1007/s00402-023-04811-3. Epub 2023 Feb 17. Arch Orthop Trauma Surg. 2023. PMID: 36799994
-
Staged Treatment of Phlegmasia Cerulea Dolens in a Patient with Iliac Vein Compression Syndrome and Deep Vein Thrombosis: A Case Report.Vasc Specialist Int. 2023 Mar 31;39:8. doi: 10.5758/vsi.230006. Vasc Specialist Int. 2023. PMID: 37006139 Free PMC article.
References
-
- The cause of the predominantly sinistral occurrence of thrombosis of the pelvic veins - R. May, J. Thurner, 1957. Thurner J. https://journals.sagepub.com/doi/abs/10.1177/000331975700800505 SAGE J. 1957 - PubMed
-
- May-Thurner Syndrome. [Jul;2020 ];Mousa Mousa, Albier Y. http://www.uptodate.com/contents/may-thurner-syndrome?search=may%2Bthurn... UpToDate, July. 2019
-
- Iliac vein compression -- its relation to iliofemoral thrombosis and the post-thrombotic syndrome. Cockett FB, Thomas ML, Negus D. http://www.ncbi.nlm.nih.gov/pmc/articles/PMC1841147 Br Med J. 1967 - PMC - PubMed
-
- Iliac vein compression in an asymptomatic patient population. Kibbe MR, Ujiki M, Goodwin AL, et al. http://www.ncbi.nlm.nih.gov/pubmed?term=15111841. J Vasc Surg. 2004;39:937–943. - PubMed
-
- Detection of deep-vein thrombosis by real-time B-mode ultrasonography. Lensing AW, Prandoni P, Brandjes D, et al. http://www.ncbi.nlm.nih.gov/pubmed?term=2643771. N Engl J Med. 1989;320:342–345. - PubMed
Publication types
LinkOut - more resources
Full Text Sources
Research Materials
Miscellaneous
